IJCRR - 14(6), March, 2022
Pages: 59-63
Date of Publication: 15-Mar-2022
Print Article
Download XML Download PDF e-Pub
Frequency of Hyperkalemia in Patients with Paraphenylenediamine Poisoning at a Tertiary Care Hospital
Author: Abdul Malik Mujahid, Asma Binte Saad, Mahriq Fatima, Hassan Shabir, Muhammad Umer Farooq, Shohreh Ahmadi
Category: Healthcare
Abstract:Introduction: Paraphenylenediamine is a low-cost and readily available hair dye in Pakistan. It is highly toxic and lethal substance when ingested. This study was conducted to determine the frequency of hyperkalemia in patients with PPD poisoning.
Objective: To determine the frequency of hyperkalemia in patients with PPD-poisoning at a tertiary care hospital.
Material and Methods: A descriptive case series study was conducted at Teaching Hospital Dera Ghazi Khan, from 1st January, 2019 to 30th June, 2020. A total of 87 patients fulfilling the inclusion criteria were enrolled. After the approval from hospital ethical Committee, informed consent was obtained from all the patients. Once registered, 3 ml venous blood sample was drawn and sent to the hospital laboratory (after every 12 hours) for serum potassium levels to diagnose hyperkalemia. Data was entered and analyzed using SPSS-23.
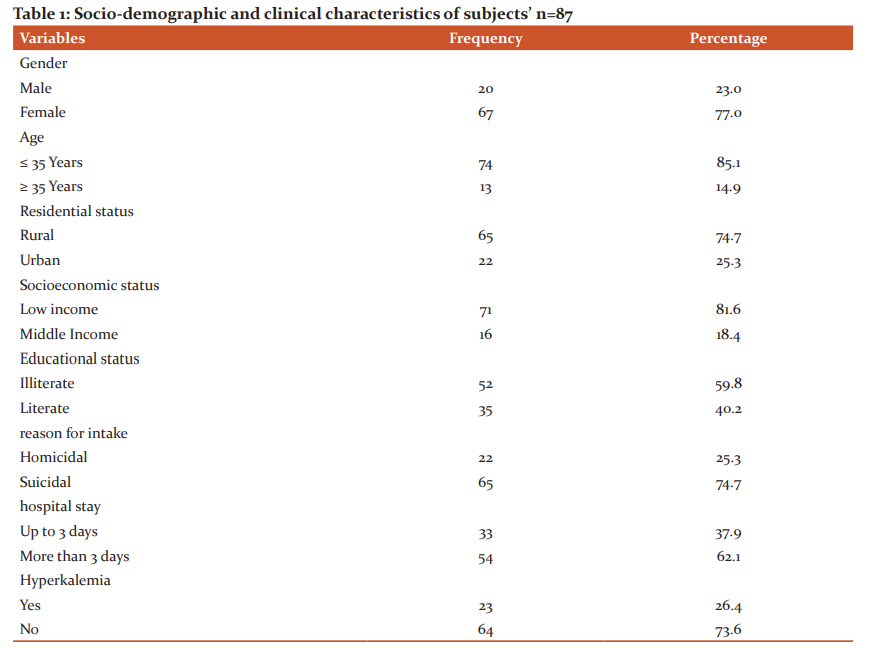
Results: Out of 87 cases, 20 (23.0 %) were male while 67 (77.0 %) were female patients. Mean age was25.69 \? 7.43 years with age range of 18-45 years. 65 patients (74.7 %) belonged to rural areas and 22 (25.3 %) to urban areas. Poor socioeconomic status was noted in 71 (81.6%) while 16 (18.4%) were of middle income. Out of 87 cases, 52 (58.9%) were illiterate and 35 (40.2%) were literate. Reason for intake was homicidal in 22 (25.3%) and suicidal in 65 (74.7%). Mean hospital stay was 6.23 \? 3.39 days and 54 (62.1 %) had hospital stay for more than 3 days. Mean serum potassium level was 5.10 \? 0.45 mmol/L and hyperkalemia was noted in 23cases (26.4%).
Conclusion: High frequency of hyperkalemia was noted in our study among patients with Paraphenylenediamine poisoning and resulted in prolong duration of hospitalization.
Keywords: Paraphenylenediamine poisoning, Hyperkalemia, Serum Potassium, Tertiary care Hospital, Hair dye, Suicidal
Full Text:
INTRODUCTION:
Poisoning is one of the common ways of suicide and deliberate self-harm.1 In underdeveloped countries including Pakistan where poverty is common due to unemployment and the literacy rate is low, use of Paraphenylenediamine has become a common method of poisoning as it is readily available and cheap in the market. PPD ingestion causes different signs and symptoms due to the involvement of multiple organs. It is brown or black-colored solid substance, a derivative of para-phenylaniline and easily soluble in H2O2.2,3,4 PPD is metabolized by electron oxidation with cytochrome P450 peroxidase to form a reactive compound called benzoquinone diamine. This can be further oxidized to a substance known as Brandowaski's base, reported causing anaphylaxis.
The first case of PPD poisoning was reported in 19245 when a barber accidentally developed toxicity while handling the dye. Hair Dye Poisoning is highly uncommon in developed countries due to strict formulary regulations; however, in developing world like Asia and Africa, it is emerging as a common means of suicide. In southeast Asia especially in India, use of hair dye as a suicidal tool is reported to have a mortality rate reaching up to 24 percent even with treatment4. As there is no antidote available for PPD poisoning, only early recognition of symptoms and timely management is the key treatment option to avoid adverse effects. Paraphenylenediamine is a major toxic substance in hair dye which can cause life-threatening neck and facial edema, laryngeal edema that may need emergency tracheostomy or endotracheal intubation to secure airway and muscle damage that may cause rhabdomyolysis and lead to acute renal failure.6
PPD poisoning is associated with a significant increase in morbidities and mortalities and is more common in females as compared to males and is more prevalent in lower social classes. In Pakistan, most incidents are reported from Sindh and Punjab related to hair dye poisoning.7, 8 Hair dye powder is readily available and its excessive use in this area has led to clinical implications of its toxicity that may accidental or suicidal. A study conducted by Haider et al.,9 has reported 34.4 % hyperkalemia in patients presenting with PPD poisoning.
This study has been proposed to document hyperkalemia in patients with PPD poisoning as we commonly treat such patients in our daily practice but no such study has been done in our local population (Dera Ghazi Khan). The results of this study will generate baseline database of our local population and help clinicians to anticipate such adverse events in early stages which will lead to the proper management of such cases.
OBJECTIVE: To determine the frequency of hyperkalemia in patients with PPD-poisoning at a tertiary care hospital
MATERIAL AND METHODS:
A descriptive case series study was conducted at the Department of Medicine, Teaching Hospital Dera Ghazi Khan from 1st January, 2019 to 30th June, 2020. A total of 87 cases were enrolled through a non-probability, consecutive sampling. All the patients with PPD poisoning with either gender; between 15 – 60 years were included and patients with past history of kidney and chronic liver disease were excluded. After the approval from hospital ethical review committee (NO.7925/Teach: Hosp: D.G.Khan/ Dated 16/12/2018), informed consent was taken for each patient. A pre-designed proforma (ANNEXURE-1) was used to collect information regarding reason for intake (suicidal, homicidal, accidental), level of education, location (urban, rural), duration of hospital stay, gender, age and family income. Once registered, 3 ml venous blood sample was drawn and sent to the hospital laboratory (after every 12 hours) for serum potassium levels to diagnose hyperkalemia. Data was entered and analyzed by a consultant physician with 10 year of post-fellowship experience using SPSS-23. Descriptive statistics was applied to calculate mean and standard deviation for the age, hospital stay and Serum potassium level. Frequencies and percentages were calculated for categorical variables like gender, age groups, reason for intake, residential status, family income, level of education and hyperkalemia. Effect modifiers like age, residential status, family income, level of education, duration of hospital stay, gender and reason for intake were controlled by stratification. Post stratification chi-square test was applied to see their effect on hyperkalemia. P-value equal or less than 0.05 was considered as significant.
RESULTS:
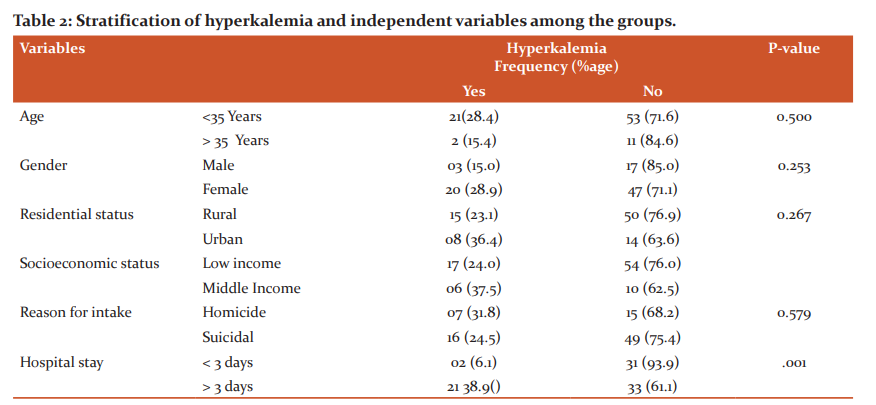
A total of 87 patients were included in study. Out of these, 20 (23.0 %) were male patients while 67 (77.0 %) were female patients. Mean age was 25.69 ± 7.43 years with age range in 18-45years. Majority of our study cases i.e. 74 (85.1 %) were aged up to 35 years. Out of these 87 cases, 65 (74.7 %) belonged to rural areas and 22 (25.3 %) belonged to urban areas. Poor socioeconomic status was noted in 71 (81.6%) while 16 (18.4%) were of middle income. 52 patients (58.9%) were illiterate and 35 (40.2%) were literate. Reason for intake was homicidal in 22 (25.3%) and suicidal in 65 (74.7%). Mean hospital stay of our study cases was 6.23 ± 3.39 days and 54 (62.1 %) had hospital stay for more than 3 days. Mean serum potassium level was 5.10 ± 0.45 mmol/L and hyperkalemia was noted in 23 (26.4%) (Table No.1). Hyperkalemia was stratified with regards to gender, age, residential status, socioeconomic status, literacy, reason for intake and hospital stay. Length of hospital stay showed a significant relationship with hyperkalemia (Table No. 2)
DISCUSSION:
A poison is chemical agent that produces adverse effects when enter the human body. Intoxication by hair dye is very common in Pakistan and this is usually attributed to the active ingredient Paraphenylenediamine (PPD). Some other hair dyes exist where the active ingredient is different from PPD e.g. NTD and other aromatic amine compounds. Intoxication can be either topical or oral or inhalational route. Cutaneous absorption and ingestion produce sever local reactions and systemic effects. There were significant biochemical and histopathological changes noted in cases admitted to the hospital. Death may occur following ingestion or absorption of small amount although the lethal dose reported in the literature is ten gram. The usual patterns of intoxication are Suicidal about (84percent), Accidental especially in children due to ingestion (eight %), Homicidal about (6percent) or through skin absorption when used for cosmetic purpose (two %). In mild cases, allergic reaction caused by use of hair dye usually involves the upper eyelids and ear, while in more advance cases there may be complete closure of eyelids and allergic contact dermatitis reaction may become widespread 10.
In our study, 20 (23.0 %) were male patients while 67 (77.0 %) were female patients. Similar results have been reported in many different studies showing PPD ingestion being more common in young female population. A study conducted by Tanweer et al.11 has reported around 78 percent female gender predominance and the study by Elgamel et al.10 has also reported about 80percent females in PPD Poisoning which is comparable with our study results. A study conducted by Ishtiaq et al.12 has also reported that seventy-one % females were involved in this poisoning. A study conducted by Kondle et al.13 has also reported eighty-two percent female gender involved. Another study by Sakuntala et al.14 and Khan et al.15 has reported about 81 percent and sixty five percent female preponderance respectively which are in compliance with our study results.
Mean age of our study cases was 25.69 ± 7.43 years with age range of 18-45 years. The majority of our study cases i.e. 74 (85.1 %) were aged up to 35 years. A study conducted by Tanweer et al.11 reported 23.21 ± 8.2 years mean age of the patients which is close to our study results. A study conducted by Ishtiaq et al.12 and Kondle et al.13 has also reported mean age 22 ± 3.4 years and 23.8 ± 7.8 years respectively and Khanet al.15 has also reported 21 years mean age, similar to that of our study results.
Out of 87 study cases, 65 (74.7 %) belonged to rural areas and 22 (25.3 %) to urban areas. Poor socioeconomic status was noted in 71 (81.6%) while 16 (18.4%) were of middle income. A study conducted by Ishtiaq et al.12 has reported 72 percent of patients from lower socioeconomic status and 74 percent from rural areas which are comparable with our study results. Another study by Khan et al.15 has also reported sixty-five % PPD poisoning cases belonged to poor families and 64.30 percent were illiterate. Reason for intake was homicidal in 22 (25.3%) and suicidal in 65 (74.7%). A study conducted by Tanweer et al.11 has also reported 82 percent suicidal intentions which is close to our study results. The mean hospital stay of our study cases was 6.23 ± 3.39 days and 54 (62.1 %) had a hospital stay for more than 3 days. A study conducted by Tanweer et al.11 has also reported 9.5 day mean duration of hospitalization which is in compliance with our study results.
The mean serum potassium level was 5.10 ± 0.45 mmol/L and hyperkalemia was noted in 23 (26.4%). A study conducted by Haider et al.9 has reported 34.4 % hyperkalemia in patients presenting with PPD poisoning.
CONCLUSION:
A high frequency of hyperkalemia was noted in our study among patients with Paraphenylenediamine poisoning and resulted in a prolonged duration of hospitalization. There is a dire need for proper legislation and implementation of law enforcement regarding the readily availability of the PPD on the counter for its control and prevention as it is associated with a significant increase in adverse events after ingestion.
Acknowledgment
The authors acknowledge the immense help received from the scholars whose articles are cited and included in the references of this manuscript
Source of Funding
None
Conflict of interest
None
Authors Contribution
Dr. Abdul Malik Mujahid.
Principal contributor, conceptualization, and design of research work, final approval
Dr. Asma Binte Saad
Writing of manuscript, collection of data
Dr. Mahriq Fatima
Literature search, statistical analysis
Dr. Hassan Shabir
Co contributor, data collection, drafting
Dr. Muhammad Umer Farooq
Data analysis, plagiarism correction, literature search
Dr. Shohreh Ahmadi
Result analysis, review of the manuscript
References:
-
Shah MMA, Ahmed S, Arafat SMY. Demography and risk factors of suicide in Bangladesh: a six-month paper content analysis. Psy J. 2017; 2017:3047025.
-
Sakuntala P, Khan PM, Sudarsi B, Manohar S, Siddeswari R, Swaroop K. Clinical profile and complications of hair dye poisoning. Int J Sci Res Pub. 2015;5(6):1–4.
-
Khan N, Khan H, Khan N, Ahmad A, Shah F, Rahman AU et al. Clinical presentation and outcome of patients with paraphenylenediamine (kala-pathar) poisoning. Gomal J Med Sci. 2015; 14(1):3–6.
-
Kondle R, Pathapati RM, Saginela SK, Malliboina S, Makineedi VP. Clinical profile and outcomes of hair dye poisoning in a teaching hospital in Nellore. ISRN Emerg Med. 2012; 624253:5.
-
Nott HW. Systemic poisoning by hair dye. Br Med J. 1924;1(3297):421–2. 78
-
Umair SF, Amin I, Urrehman A. Hair Dye poisoning: "An early intervention". Pak J Med Sci. 2018 Jan-Feb; 34(1):230-32.
-
Naqvi R, Akhtar F, Farooq U, Ashraf S, Rizvi SA. From diamonds to black stone; myth to reality: Acute kidney injury with Paraphenylenediamine poisoning. Neph J.2015;20(12):887–91.
-
Bokutz M, Nasir N, Mahmood F, Sajid S. Hair dye poisoning and rhabdomyolysis. J Pak Med Assoc. 2015;65(4):425–26
-
Haider SH, Sultan A, Salman Z, Waris S, Bandesha Y. Paraphenylenediamine poisoning: clinical presentations and outcomes. Anaesth Pain Inten Care. 2018;22(1):43-7.
-
Elgamel AA, Ahmed NO. Complications and management of hair dye poisoning in Khartoum. Sudan Med Monit 2013;8:146-52
-
Tanweer S, Saeed M, Zaidi S, Aslam W. Clinical Profile and Outcome of Paraphenylenediamine Poisoning. J Coll Phy Surg Pak. 2018;28(5):374-77.
-
Ishtiaq R, Shafiq S, Imran A, Masroor Ali Q, Khan R, Tariq H, et al. Frequency of Acute Hepatitis Following Acute Paraphenylene Diamine Intoxication. Cureus. 2017 Apr 21;9(4):e1186.
-
Kondle R, Phatapati RM, Saginela SK, Malliboina S, Makineedi VP. Clinical profile and outcome of hair dye poisoning in a teaching hospital in Nellore. ISRN Emerg Med. 2012; 6 (2):42-53.
-
Sakuntala P, Khan PM, Sudarsi B, Manohar S, Siddeswari R, Swaroop K. Clinical profile and complications of hair dye poisoning. Int J Sci Res Pub. 2015;5(6):1-4.
-
Khan MA, Akram S, Shah HBU, Hamdani SAM, Khan M. Epidemic of Kala Pathar (Paraphenylene Diamine) Poisoning: an Emerging Threat in Southern Punjab. J Coll Phy Surg Pak. 2018;28(1):44-7.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License