IJCRR - 13(20), October, 2021
Pages: 143-148
Date of Publication: 24-Oct-2021
Print Article
Download XML Download PDF
Comparative Study of Outcome of Patients with ST-Segment Elevation Myocardial Infarction in Diabetics and Non-Diabetics
Author: Mankar Parikshit Gajanan, Thorat Sanjay Tukaram, Virendra C. Patil
Category: Healthcare
Abstract:Introduction: Although myocardial infarction is often depicted as a modern disease it was recognized before the modern era. There were references to what could be recognized today as angina pectoris, myocardial infarction and sudden death in ancient Egyptian, Greek, Biblical and the lmudic sources. Coronary angiogram performed 6-9 days showed patent vessel in all patients of group-I as compared to only 2 patients of group-II. Ejection Fraction (EF) increased from 38% to 47% in group I as compared to unchanged 40% as assayed by gated b ejection fraction lood pool imaging after 35 days. Aim: The aim here is to compare the outcome of patients with ST-Segment Elevation Myocardial Infarction (STEMI) myocardial infractions in diabetics and non-diabetics. Method: The method that we have adopted for our research is carried on patients admitted to the Medical Intensive Care Unit (MICU) of Krishna Institute of Medical Sciences, Karad over 18 months from October 2018 to March 2020. This study was approved by the institutional ethics and protocol committee. Protocol number 0257/2018-2019. Result: We studied 160 patients, 80 nondiabetic and 80 diabetic patients of 'ST'- Segment myocardial infarction in Krishna institute of medical sciences and research centre, Karad. Out of 160 patients in the present study majority of the cases were from 60-69(38.8%) years of age. Duration of hospital stay was significantly higher in diabetic patients compared to non-diabetic patients (p=0.023). No significant difference was observed in the final outcome (deaths and discharge) between the two groups. Conclusion: Failed thrombolysis in acute myocardial infarction was more in diabetic 'ST' segment elevation myocardial infarction patients as compared to non-diabetic 'ST' segment elevation myocardial infarction patients. Even when promptly receiving thrombolytics, the outcome in the diabetic group, both in terms of mortality and morbidity was worse as compared to the nondiabetic group.
Keywords: St-segment, Myocardial Infarction, Diabetic, Coronary artery, Thrombolysis, Hypotension
Full Text:
Introduction:
Although myocardial infarction is often depicted as a modern disease it was recognized before the modern era. There were references to what could be recognized today as angina pectoris, myocardial infarction and sudden death in ancient Egyptian, Greek, Biblical and lmudic sources. William Heberden in 1768 presented his classic description of angina pectoris in a lecture before the Royal College of Physicians and it was published in 1772.1dam Hammer, a physician in Monneheim is credited with the first antemortem diagnosis of coronary thrombosis with an autopsy showing a clot in a coronary artery in 1898. Sir William Osler in 1910, delivered a lecture to the Royal College of Physicians, which noted that he had found the condition to be more common amongst his private or upper-class patients than the poorer classes he saw at St. Bartholomew’s hospital, noting also the tendency of the disease to have a familial disposition. He thus combined the modern etiological theories of the interaction between environment and genetics.2
Favaloro RG et al. in 1971 developed the first effective coronary bypass grafting using reversed saphenous veins. He also concluded that treating an acute MI with coronary bypass grafting within 6 hours of onset could reverse the effects of acute MI limit infarct size and improve MI postoperatively. Berg and colleagues from Spokane, Washington in 1975 published one of the first papers advocating the use of Coronary artery bypass grafting (CABG) for the treatment of acute MI and showed the benefit of surgical intervention by decreasing mortality rates significantly when revascularization was accomplished in < 6 hours.3Anderson et al. in 1983 randomized 50 patients with chest pain of fewer than four hours duration and persistent ST-segment elevation, Intracoronary streptokinase treated patients had significant improvement in global ejection fraction 10 days after therapy. The reperfusion rate in streptokinase treated patients was 79% with significant improvement in echocardiographic wall motion index and less loss of R-wave amplitude compared to control. A trend towards decreased mortality occurred in the streptokinase-treated group, but it did not reach statistical significance.4
In the GISSI study conducted in 1986, a total of 11806 patients were randomized to either intravenous streptokinase or control within 12 hours of symptom onset. At 21 days overall hospital mortality was 10.7% in streptokinase versus 13% in control, an 18% reduction. The benefit was most striking in patients treated within 3 hours (relative risk 0.74) from symptom onset, it remained statistically significant in the 3-6 hour group (0.80). A non-statistically significant reduction of mortality in the 6 to 9 hour (0.87) group and this difference reversed in the 9 to 12 hours group (relative rate 1.19) probably because the numerator and denominator in the late treated group were very small producing unstable estimates.5 Leoncini M et al. in 1994 evaluated the effectiveness of late thrombolysis (6-24 hours) in 15 patients with pre and post-treatment perfusion scintigraphy with TC99m sestamibi. 7 patients with perfusion recovery (group-1) showed a significant decrease in uptake score compared to 8 patients with absent or minimal perfusion recovery after thrombolysis (group-II). Defect score further reduced in group-I patients along with the decrease in asynergic score assayed by 2D echo significantly after 35 days compared to group II patients. Coronary angiogram performed 6-9 days showed patent vessel in all patients of group-I as compared to only 2 patients of group-II. EF increased from 38% to 47% in group I as compared to unchanged 40% as assayed by gated blood pool imaging after 35 days. Thus, it was demonstrated that it is still possible to obtain effective reperfusion and the consequent salvage of jeopardized tissue demonstrated by the recovery of both regional and global left ventricular function.6, 7
Complications
(A) Bleeding
Thrombolysis aims to lyse the thrombus in the artery and establish blood flow since this process involves activation of the plasminogen and the expected complication is bleeding. A thrombus which is preventing a vascular leak in a blood vessel is also lysed and leads to bleeding. Bleeding can occur in various places and is usually classified as either 1 Intracranial or 2 Systemic
1 Intracranial
Recent studies signify the incidence and risk factor for intracranial haemorrhage. The risk is around 0.3 - 0.5 %. These complications are rarely diagnosed because a massive infarct or haemorrhage may cause sudden death before imaging studies could be done and the death is usually attributed to a cardiac cause.
In the ISIS-318 trial 0.4% without heparin, 0.6% with heparin the risk of ICH is more with the heparin used group than the other. However, there was decreased risk of thrombotic stroke when heparin was used. IV heparin use in STEMI has increased the risk for intracranial haemorrhage but the risk of an ischemic stroke is less.
2 Systemic bleeding
The thrombolysis patient is at high risk for any invasive procedures and also for coronary Angiogram or PTCA.
(B)Immunologic complications
The active compound of streptokinase is produced by beta-hemolytic streptococcus; since it is a common pathogen it leads to frequent allergic reactions. These allergic manifestations are acute and delayed. Delayed is characterized by fever, arthralgia, leukocytoclastic vasculitis, renal failure, interstitial pulmonary abnormalities.
(C)Hypotension
Hypotension occurs in MI due to failure of ventricles to pump blood, inadequate filling of ventricles etc. Hypotension may occur following thrombolysis due to the massive release of vasodilatory chemokines like HMWK and bradykinin. In a trial it was established that fall of 35 mmHg in systolic BP in patients treated with streptokinase and that 38% had systolic BP <90 mmHg transiently. Hypotension documented in GISSI-2 trial 4.4% with streptokinase.8 In ISIS-3 trial 6.8% with streptokinase.9
The fall in Blood pressure which occurs in patients treated with streptokinase is due to an allergic reaction and it responds well to I.V. Fluids and anti-allergic medication and other supportive measures
(D)Myocardial rupture of reperfusion injury
Myocardial reperfusion may lead to the release of chemokines from dying cells and leads to further inflammation and also occlusion of micro-circulation by the inflammatory cells.
A study conducted by Essen R et al. showed late thrombolysis may cause reperfusion injury and even cause myocardial rupture leading to death.
This Myocardial rupture was more in patients’ thrombolysis after 12 hours of symptom onset and occurs due to the dissection of the free wall of the ventricle which is infarcted.10
(E)Thromboembolic Complications
Patients with longstanding valvular heart disease may have a clot in the chambers of the heart and this may be partially lysed and may be embolised to the systemic circulation leading to fatal complications.
Assessment of Myocardial Reperfusion
Coronary artery patency and myocardial reperfusion can be assessed soon after the completion of administration of thrombolytic therapy and also following discharge of such a patient from the hospital. Hence it can be assessed in two stages (a) Early assessment and (b) Late assessment.
Conjunctive Treatment
Thrombin Antagonists and Antiplatelet Agents
Two major limiting factors for the clinical benefits of thrombolytic therapy are:
1. One fourth to one-fifth of the thrombus in coronaries are not thrombolysed
2. One in 10 patients develop re-occlusion of the thrombolyzed vessel
These are caused by increased clotting activity at the site of occlusion where the atherosclerotic plaque is present. Thrombin, the main enzyme in the clotting pathway stimulates the fibrin and causes platelet activation and the thrombus is formed. These pro-coagulant cells are activated further by the clotting factors and this leads to a vicious cycle leading to thrombus formation and occlusion of the vessel. The treatment plan involves activating fibrinolysis and inhibit the clotting pathway and inhibiting the factors that favour clotting. Heparin and platelet inhibitors are the main drugs used to inhibit clotting and inhibit platelet aggregation and prevent clot formation. But these drugs may cause bleeding when used in conjunction with fibrinolysis. Hence highly selective drugs with less complication are needed to prevent resistance to fibrinolysis and reocclusion.
This is the rationale behind the use of antiplatelet drugs in acute STEMI along with fibrinolytic therapy, these drugs inhibit platelet plug formation and also act on the atherosclerotic plaque and stabilise it, and these drugs however in some cases may cause bleeding leading to fatal complications like intra- cerebral haemorrhage.
Combination Therapy
The mechanism of formation of thrombus in a coronary artery justifies the use of combination therapy i.e. anticoagulant and anti-platelet drugs along with fibrinolysis.
The commonly used combination is heparin, aspirin with fibrinolysis shows a benefit and increased efficacy of thrombolysis and prevents re-occlusion of a thrombolysed vessel. Besides the benefit, these drugs cause an increase in hemorrhagic complications especially when the patient is planned for an invasive procedure like angiogram or PTCA, several trials are demonstrating both the beneficial effects of this combination of heparin, aspirin and fibrinolytic and the increased risk of bleeding associated with combination, in GISSI-2 study the hemorrhagic complications are more with the use of streptokinase compared with other fibrinolytic drugs.
Aim:
The study aims to compare the outcome of patients with STEMI myocardial infractions in diabetics and non-diabetics.
Objectives:
• To study STEMI in diabetics.
• To study STEMI in non-diabetics.
• To analyse the hypothesis drawn by comparing STEMI in diabetics and non-diabetics.
Methods:
This study was a comparative study. The study was carried on patients admitted to the Medical Intensive Care Unit (MICU) of Krishna Institute of Medical Sciences, Karad over 18 months from October 2018 to March 2020. This study was conducted over 18 months. (October 2018 to March 2020). This study was approved by the institutional ethics and protocol committee. Protocol number 0257/2018-2019. The sample size is calculated based on the study conducted by Varshit Hathi et al. according to the formula.11
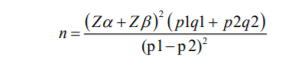
Zα = 1.96 Type I error at 5% level of significance Zβ = 0.842 Type II error
p1 = 180 out of 186 non-diabetics = 96.77% q1 =100 – p1 = 3.23%
p2 = 174 out of 208 diabetics = 83.65% q2 =100 – p2 = 16.35%
n = (1.96 + 0.842)2 [(96.77 x 3.23) + (83.65 x 16.35)]
(83.65 - 96.77)2
n = 76.64
For better yield = 80 patients per group
Inclusion criteria:
• Patients with STEMI coming to the hospital within 12 hours of onset chest pain
• Known diabetic or newly diagnosed during the hospital stay
• Non-diabetics
• Positive troponin-I test
Exclusion criteria:
• Patients presenting after 12 hours of the onset of symptoms
• Patients with contraindications for thrombolysis
• Patient with the symptom of Congestive heart failure and Coronary Artery Disease
• Patients with type 1 diabetes mellitus
• Patient on drug therapy with drugs known to cause cardiomyopathy (eg. Daunorubicin, Bleomycin, Adriamycin etc.
• Patient associated with any comorbid condition (Chronic liver disease, history of previous MI, Malignancy, any thyroid therapy, chronic kidney disease)
Informed written consent:
The patients fulfilling the selection criteria were briefed about the nature of the study and included in the study after obtaining written informed consent.
Data collection:
Patients fulfilling selection criteria were selected on a consecutive basis for study. Patients were interviewed to obtain demographic characteristics such as age and sex, presenting complaints, diabetic history and history of other co-morbidities. These patients were subjected to clinical examination and the findings including vitals and systemic examination findings were noted. These findings were recorded on a predesigned and pretested proforma.
Result:
We studied 160 patients, 80 nondiabetic and 80 diabetic patients of ‘ST’- Segment myocardial infarction in Krishna institute of medical sciences and research centre, Karad. Out of 160 patients in the present study majority of the cases were from 60-69(38.8%) years of age. The mean age observed in the non-diabetic group was 61.4+12.1 years and in the diabetic group, it was 59.6+10.4 years. Out of the total of 160 patients enrolled in study 101(63.1%) were males and 59(36.9%) were females. Eighty non-diabetic patients were included of the 48(60%) were males and 32(40%) were females. Eighty diabetic patients were included of the 53(66.3%) patients were males and 27(33.8%) were females.
Anterior wall myocardial infarction was seen most commonly in 100(62.5%) patients followed by inferior wall MI in 56(35%) patients followed by posterior wall MI in 4(2.5%) patients. Failed ST-Segment resolution was seen in 32(40%) diabetic patients and 13(16.3%) non-diabetic patients. Thus failed resolution was observed to be more common in the diabetic group(p=0.00083). No significant difference in percent ST-Segment resolution in ECG was observed between the two thrombolytic agents; Streptokinase and Reteplase used in the study. The mean ejection fraction observed in diabetic and non-diabetic was not significantly different after thrombolysis. No significant difference was observed in ejection fraction between the two groups; diabetics and non-diabetics based on the anatomical location of myocardial infarction.
Duration of hospital stay was significantly higher in diabetic patients compared to non-diabetic patients(p=0.023). No significant difference was observed in the outcome (deaths and discharge) between the two groups. Mean HbA1c in the diabetic group was significantly higher than the non-diabetic group(p<0.001).In the lipid profile mean triglyceride levels in the diabetic group was observed to be significantly higher than in the non-diabetic group(p=0.011). No significant difference was observed between HDL and LDL levels in diabetic and non-diabetic groups.
Discussion:
The incidence of CAD is two times more in diabetic males and four times more in postmenopausal diabetic females when compared to respective non- diabetics. CAD contributes one-third to the death of diabetics after the age of 40. It is characterized by premature age of onset. In diabetics, the incidence and prevalence of triple vessel disease are also more as the distribution of fibrous plaques is also more. The outcome of acute myocardial infarction treated with fibrinolytic therapy can be evaluated by measurement of ST-Segment resolution at 90 minutes after thrombolysis, in 12 lead ECG.12
Demographic profile and frequency distribution of age groups
There were 101 males(63.1%) and 59 females(36.9%) in present study. The male to female ratio was 1.71. Out of 101 males, 53 males were in a diabetic group whereas 48 males were in the non-diabetic group and out of 59 females 27 were in the diabetic group and 32 were in the non-diabetic group.
Shahriar Iqbal et al. in their study found that most of the study subjects out of their 100 subjects were male which was 58%(29) in the diabetic group 88%(44) in the non-diabetic group and females were 42%(21) and 12%(6) in diabetic and non-diabetic groups respectively.13 Male to female ratio in their study was 2.70 which was higher than the present study. In another study by RK Singh et al., there were 176 males (77.2%) out of 228 patients and 52 females(22.8%) and their male: female ratio is 3.38 which is also higher than the present study.[14] Varshit Hathi et al. in their study had 166 male(79.81%) diabetics and 42 female(20.19%) diabetics out of a total of 208 diabetic patients with STEMI compared to 124 males(66.66%) and 62 females(33.33%) in the non-diabetic group.11
Location of Myocardial Infarction
The present study found that among 160 patients in diabetic and non-diabetic study groups anterior wall myocardial infarction was most common in both study groups including 100 patients(62.5%) amongst the total patients.56 patients(35%) were having inferior wall myocardial infarction and only 4 patients(2.5%) presented with posterior wall myocardial infarction.
Amongst diabetic patients, 52(65%) patients were having anterior wall myocardial infarction whereas in the non-diabetic group 48(60%) patients were having anterior wall myocardial infarction. Inferior wall myocardial infarction was seen in 26 (32.5%) and 30(37.5%) patients in diabetic and non-diabetic groups respectively. Posterior wall MI was seen in 2(2.5%) patients in each group.
In a study done by RK Singh et al. anterior wall myocardial infarction was seen in 68.9%(157) patients and inferior wall MI was seen in 31.1% of patients which is the same as the present study.14
JD Newman et al. in his study on 4845 patients found that inferior wall myocardial infarction was most common in the study population which constituted 37.2% of the cases, anterior wall myocardial infarction was found in 32.8% of patients, 13.2% of patients were having posterior wall MI and remaining patients (16.8%) were having multiple site infarcts.15 These findings are not consistent with the present study. These differences could be because of differences in the sample size and duration of the study.
Comparison of ST Resolution among Non-diabetic and Diabetic groups concerning agent used
In the present study streptokinase and reteplase, two thrombolytic agents were used. Out of 160 patients, 100 patients were thrombolysed with streptokinase and the remaining 60 patients were thrombolysed with reteplase. 29(36.3%) diabetic patients and 31 (38.8%) non-diabetic patients were thrombosed with reteplase whereas 51(63.8%) diabetics and 49(61.3%) non-diabetic patients were thrombosed with streptokinase.27(27%) patients thrombolised with streptokinase showed complete resolution, 41(41%) patients showed partial resolution whereas 32(32%) patients showed complete resolution.22(36.7%) patients thrombolysed with reteplase showed complete resolution, 25(41.7%) patients showed partial resolution, and 13(21.7%) patients showed complete resolution. No significant difference was observed in the percent resolution of the two agents (p=0.276).
The INJECT trial done to evaluate the efficacy of reteplase over streptokinase showed reteplase is as effective as streptokinase which is following the present study.16 In a study done by RK Singh et al. with reteplase 204(90.5%) patients showed 50% resolution whereas, in the study done by Shah K et al..14, 15 73.75% patients achieved 50% reduction in ST-Elevation.
Conclusion:
The present study concludes that failed thrombolysis in acute myocardial infarction was more in diabetic ‘ST’ segment elevation myocardial infarction patients as compared to non-diabetic ‘ST’ segment elevation myocardial infarction patients. In the present study, it was observed that the incidence of anterior wall MI was more and showed male predominance. In the present study, it was observed that successful thrombolysis was more in the non-diabetic group. There was no obvious difference in outcome amongst the two different thrombolytic agents used. In the present study, we found that no there was no significant difference in left ventricular ejection fraction between diabetic and non-diabetic groups post thrombolysis. Hypertriglyceridemia was observed in diabetic patients in comparison with non-diabetic patients. In the present study duration of hospital stay was observed to be more in the diabetic group compared to the non-diabetic group. We conclude that even when promptly receiving thrombolytics, the outcome in the diabetic group, both in terms of mortality and morbidity was worse as compared to the non-diabetic group.
Acknowledgement: We acknowledge the contribution of our university and department for the unending support.
Conflict of Interest: There is no conflict of Interest
Source of Funding: No Source of Funding
Author's Contribution: This is a collaborative work among all authors. Parikshit Gajanan Mankar, Sanjay Tukaram Thorat, performed the statistical analysis, wrote the protocol, and wrote the first draft of the manuscript. Parikshit Gajanan Mankar, Virendra.C. Patil managed the literature searches. All the authors read and approved the final manuscript.
References:
1. Schlant RC, Alexander RW, O'Rourke RA, Hurst JW. The Heart, Arteries, and Veins: Volume One. McGraw-Hill; 1994.
2. Sleight P. Myocardial infarction. In: Weatherall DJ, Ledingham J.G.G., Warrell D.A. editors Oxford Textbook of Medicine, 5th Edition. Oxford; Oxford Press: 2018. P. 2331-2348.
3. Berg R Jr, Selinger SL, Leonard JJ, Coleman WS, DeWood M. Acute evolving myocardial infarction. A surgical emergency. J. Thorac. Cardiovasc. Surg. 1984;88(11):902-906.
4. Anderson JL, Marshall HW, Bray BE, Lutz JR, Frederick PR, Yanowitz FG, Datz FL, et al.. A randomized trial of intracoronary streptokinase in the treatment of acute myocardial infarction. N Engl J Med, 1983; 308(6): 1312-8.
5. Gruppo Italiano Per lo Studio della Streptochinasi nell’ Infarto miocardico (GISSI). Effectiveness of intravenous thrombolytic treatment in acute myocardial infarction. Lancet 1986;1(2): 397-402.
6. Leoncini M, Marcucci G, Santoro GM, Sciagrà R, Bini L, Bisi G, et al.. [Late thrombolysis in acute myocardial infarct. Demonstration of myocardial tissue salvage by the assessment of pre- and post- thrombolytic perfusion and left ventricular function]. G Ital Cardiol. 1994;24(11):1359-70.
7. Zairis MN, Lyras AG, Makrygiannis SS, Psarogianni PK, Adamopoulou EN, Handanis SM, et al.. Type 2 diabetes and intravenous thrombolysis outcome in the setting of ST-elevation myocardial infarction. Diabetes Care. 2004;27(4):967-71.
8. Effectiveness of intravenous thrombolytic treatment in acute myocardial infarction. Gruppo Italiano per lo Studio della Streptochinasi nell'Infarto Miocardico (GISSI). Lancet. 1986;1(2):397-402.
9. ISIS-3: a randomized comparison of streptokinase vs tissue plasminogen activator vs anistreplase and aspirin plus heparin vs aspirin alone among 41,299 cases of suspected acute myocardial infarction. ISIS-3 (Third International Study of Infarct Survival) Collaborative Group. Lancet. 1992;339(3):753-70.
10. Von Essen R, Schmidt W, Uebis R, Edelmann B, Effert S, Silny J, et al.. Myocardial infarction and thrombolysis. Electrocardiographic short-term and long-term results using precordial mapping. Br Heart J. 1985;54(7):6-10.
11. Hathi V, Anadkat M. A Comparative Study of In-Hospital Outcome of Patients with ST-Segment Elevation Myocardial Infarction with and Without Diabetes Mellitus, after Thrombolytic Therapy; In Government Hospital of Rajkot, Gujarat, India. J Assoc Physicians India. 2017;65(11):22-25.
12. Sulehria SB, Nabeel M, Awan AK. Failure of Streptokinase Therapy in Diabetic and Non-Diabetic Patients Presenting with ST-Elevation Myocardial Infarction Pak J Med Health Sci. 2014;8(3):750-52.
13. Iqbal, S., Bari M, S. Bari, M. Islam, M. Majumder, M. A. Islam, et al. A Comparative Study of St Segment Resolution between Diabetic and Non-Diabetic ST-Segment Elevation Myocardial Infarction Patients following Streptokinase Thrombolysis Cardiovasc. J.2019;11(2):118-122.
14. Singh RK, Trailokya A, Naik MM. Post-Reteplase Evaluation of Clinical Safety & Efficacy in Indian Patients (Precise-In Study). J Assoc Physicians India. 2015;63(4):30, 32-5.
15. Shah I, Hafizullah M, Shah ST, Gul AD, Iqbal A. Comparison of the efficacy and safety of thrombolytic therapy for st-elevation myocardial infarction in patients with and without diabetes mellitus. Pak Heart J 2012; 45 (01): 3338.
16. INJECT Investigators. International Joint Efficacy Comparison of Thrombolytics. Randomized, double-blind comparison of reteplase double-bolus administration with streptokinase in acute myocardial infarction (INJECT): trial to investigate equivalence. Lancet. 1995;346(8971):329-36.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License