IJCRR - 13(13), July, 2021
Pages: 13-17
Date of Publication: 05-Jul-2021
Print Article
Download XML Download PDF
Evaluation of Impact Strength of Silver Nano-Particles Reinforced Heat-Activated Polymethylmethacrylate (Pmma) Resin at Various Proportions
Author: Suganya S, Ahila SC, MuthuKumar B, Vasantha Kumar M
Category: Healthcare
Abstract:Introduction: Impact strength of denture base resin is an important factor for making a durable dental prosthesis. Reinforcement with nanoparticles improves the performance of any kind of medical and dental prosthesis. Purpose: To evaluate and compare the impact strength of heat-activated polymethylmethacrylate resin reinforced with Silver nanoparticles in the ratio of 4:1, 3:1, 2:1 to the weight of denture base resin. Materials and Method: According to the ISO 1570, the die was made with a dimension of 55x10x10 mm with a 'V' shaped notch in the centre. The die was duplicated with putty material and the wax patterns were made in baseplate wax and poured into the mould. Then the synthesis of silver nanoparticles was done by reduction method and incorporated into the heat-activated polymethyl methacrylate (PMMA) resin in the ratio of 0:1 4:1, 3:1, 2:1 (Group A (control), Group B, Group C, and Group D) to the weight of denture base resin. The samples were polymerized at a temperature of 74\?C for 8 hours. Then the impact strength was calculated with Charpy's tester. Comparison of impact strength within the group was done using one way ANOVA. Results: On comparing the impact strength of conventional heat-activated PMMA resin with PMMA resin reinforced with silver nanoparticles at 4:1,3;1,2;1 showed the significant value P < 0.001, hence the result is 99.9% statistically significant. Conclusion: The impact strength of heat-activated polymethylmethacrylate resin reinforced with silver nanoparticle in the ratio of 4:1,3;1,2;1 was more than the conventional heat-activated PMMA resin.
Keywords: Impact strength; Polymethyl methacrylate resin; Silver nanoparticle
Full Text:
INTRODUCTION
Removable dental prosthesis is most widely utilized to replace missing teeth in dental applications.1 Polymethyl methacrylate (PMMA) is the commonly used material to fabricate denture base by heat-curing technique since the 1940s.2 Polymethacrylate (PMMA) resins have dominated the denture base market since their introduction in 1937.3 It satisfies most of the requirements of denture base materials in terms of good esthetics, ease of processing and separability, reasonable cost, etc. However, it has relatively poor resistance to impact and flexural forces that may affect denture design and life span.4
Most dentures fractures are caused by the combination of fatigue and impact failure, whereas for mandibular dentures, 80% of fractures are caused by impact and involves very high repair costs worldwide.5 Ahmed and Ebrahim 6 found that nearly 70% of dentures had broken within the first 3 years of their delivery.
Impact failures usually occur out of the mouth as a result of a sudden blow to the denture or by accidental dropping.7The PMMA has a low modulus of elasticity, low impact strength, and low flexural strength but it has many characteristics,8 made it used as denture base material such as ease in processing, stability in the oral environment, lightweight, excellent aesthetic properties, low cost, low water absorption, and can easily recharge and repaired its shape.9,10
Recent researches showed that the physical and mechanical properties of denture base materials were improved by the addition of fillers to PMMA resin material fibres like polyethene, aramid, carbon and Kevlar were used for reinforcement of denture base resin. But the carbon and Kevlar fibres gave a black tint to the denture base resin which will affect the esthetics of the denture.8
With the advent of nanotechnology, silver nanoparticles have been synthesised and have been shown potent antimicrobial properties. Silver nanoparticles have been shown unique interaction with bacteria, fungi. They are smaller in size hence they possess physical, chemical and biological properties distinction from bulky material. The smaller particle with a larger surface area provides potent antibacterial action at a lower filler level and avoiding negative influence on mechanical properties. Although the literature related to silver nanocomposites reported with antimicrobial application in the medical field,11 very few studies about the addition of silver particles to denture base resins have been published. Hence this study was done to evaluate and compare the impact strength of heat-activated polymethylmethacrylate resin reinforced with Silver (Ag) nanoparticles in the ratio of 4:1, 3:1, 2:1 to the weight of denture base resin. A hypothesis was formulated that the impact strength of silver nanoparticles reinforced heat polymerized PMMA resin would be similar to conventional denture base resin.
MATERIALS AND METHOD
Preparation of silver nanoparticles
For the synthesis of silver nanoparticles chemical reduction method was followed in which the silver nanoparticles were prepared by dissolving 2.52 g of silver nitrate (Merck Specialities Pvt Ltd, India) in 15 mL of deionised water to get a solution of 1 mole. Then 2.23 g of sodium borohydride (Sisco Laboratories Pvt Ltd, India) mixed in 30 mL of deionised with a magnetic stirrer to get a solution of 2 moles in a conical flask. Then the silver nitrate solution is transferred to a burette and then allowed to drop slowly into sodium borohydride solution in a conical flask and mixed with a magnetic stirrer to prevent agglomeration. The temperature around the conical flask was controlled by placing ice cubes. As the stirring process continues, the agglomerates of silver nanoparticles start forming. Then the agglomerates of silver nanoparticles were washed with deionized water, centrifuged, and dried in an incubator at 65°C overnight. It is then ground with a mortar and pestle.
Sample preparation
According to the ISO 1570, a metal die was made with a dimension of 55x10x10mm with a ‘V’ shaped notch in the centre. The notch is 2mm deep and at an angle of 45° to the horizontal plane. Polyvinylsiloxane (Aquasil, Dentsply, India) putty was used as duplicating material to create a mould space for the fabrication of wax patterns. Baseplate wax (Hindustan modelling wax, India) was used for fabricating the wax pattern.
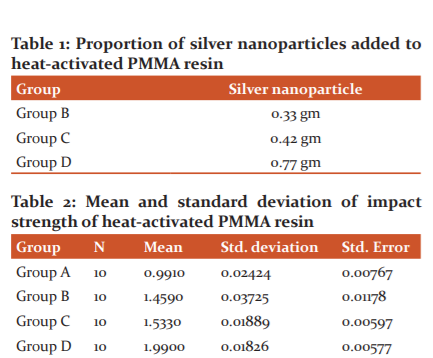
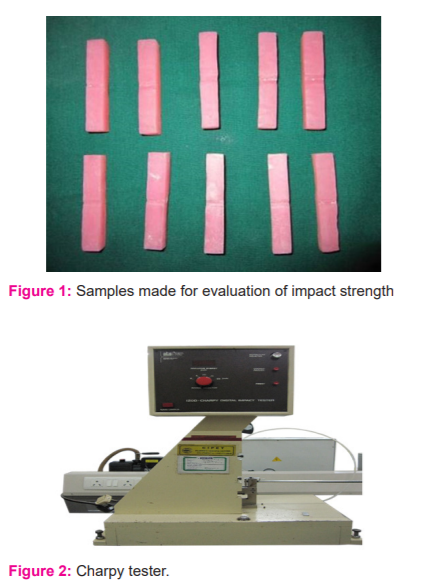
A total number of forty wax patterns (Figure.1) were thus made for the preparation of heat-cured acrylic resin samples with silver nanoparticles for evaluating the impact strength. Heat cure acrylic denture base (Dental Products of India) was chosen as the material for fabricating the samples. The synthetic nanoparticle which was made earlier was mixed with the heat-activated polymer in the ratio of 4:1, 3:1, 2:1 was considered as a control- no nanoparticles (Group A), Group B, Group C, and Group D to the weight of denture base resin with a mortar and pestle. (Table.1)
For the packing of resin, a compression moulding technique was followed. The hydraulic press (Silfradent, India) was used at 1500 Psi to apply pressure for 3 hours. The curing cycle followed was a long curing cycle and hence the entire flask with the packed material was polymerized at a temperature of 74°C for 8 hours (Delta poly bath, India).
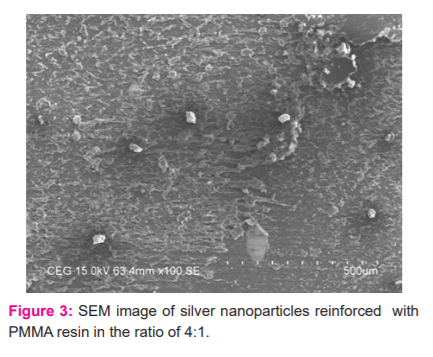
The fabricated samples are then evaluated for impact strength under Charpy tester (Izod digital Charpy impact tester, Blue star India). (Figure.2) Then the samples were analysed under Scanning Electron Microscope (Phenom X, Phenom-World B V, Netherland) for the distribution of silver nanoparticles. (Figure 3, 4 and 5)
Statistical analysis used
The impact strength values were statistically analyzed using SPSS version 22.0 (Armonk, NY: IBM Corp). Power analysis was done to establish the sample size at a 99.9% confidence interval. Comparisons within the group were done using One way ANOVA.
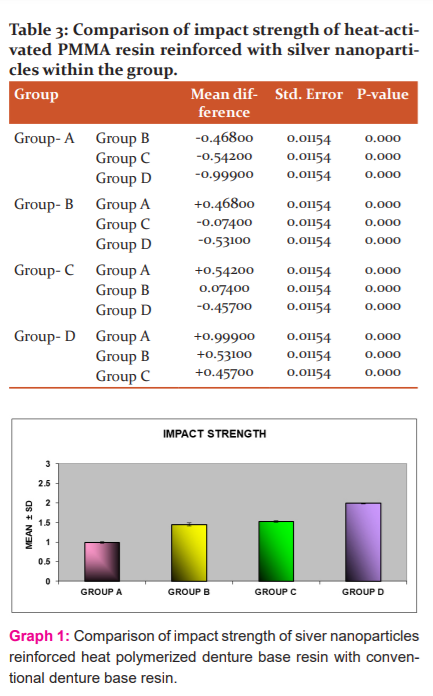
RESULTS
The mean, standard deviation and standard error of impact strength of Group A, Group B, Group C, and Group D. were 0.9910 ± 0.02424, 1.4590 ±0.03725, 1.5330 ±0.01889, 1.9900 ± 0.01826 J/mm respectively. (Table2) showed the P-value <0.001, hence the impact strength silver nanoparticles reinforced heat-activated PMMA resin showed 99.9% significant impact strength compared to the control group. (Table 3) Graph.1represents the impact strength values obtained with the control group and silver nanoparticles in the ratio of 4;1, 3:1, 2:1 to PMMA resin.
DISCUSSION
PMMA resin has been used as a denture base material for more than 70 years. The properties that have contributed the most to the success are excellent appearance, simple processing and easy repair.12 Besides its favourable characteristics, this material has relatively poor mechanical properties such as low toughness and fatigue resistance, to be used as denture bases resulting in repeated fractures requiring repair.13 The Charpy type test selected for the present study has been used by investigators to evaluate the impact strength of denture base acrylic resins.14-17
The reinforcement of ZrO2 nanoparticles with heat-cure denture base resin decreased the impact strength of the resin but increased the dimensional accuracy and fit of the denture base.18According to a study conducted by Abdulkareem and Hatim,19 its was concluded that samples prepared from PMMA resin is a biocompatible material and silver nanoparticles exhibited the good level of compatibility.
In this study, the mean values of impact strength of control group A were 0.9910±0.02424 J/mm, for group B 1.4590±0.03725 J/mm, for group C 1.5330±0.01889 J/mm and 1.9900 ±0.01826J/mm for group D. On comparison of the mean values between the control and other groups showed a significant p-value < 0.001 and hence the result was 99.9% significant.
Synthetically prepared nanoparticle forms non agglomerated discrete particles that are likely to penetrate molecules of polymers getting themselves distributed homogenously in the resin molecular chain to produce nanocomposites. Interpretation of the chemistry of this reaction has shown that the silver nanoparticles influenced the formation of the molecular chain by its penetration and bonding molecules thereby increasing the molecular weight of polymers. The corresponding increased values could also be due to decreased ability of the polymer to flow during chain reactions from manipulating to the processing stage. Further increased strength also occurs due to alteration of relaxation behaviour generated by nano-agglomerates of silver nanoparticles incorporated into the polymer matrix. This reaction is responsible for the effects of intermolecular forms affecting the chain stiffness resulting in higher impact strength of acrylic resin.
The limitations of the study are that the distribution of silver nanoparticles in PMMA resin was uncertain and also it affects the esthetics due to its colour hence, could be used only for the palatal and the lingual contours.
CONCLUSION
Within the limitations of the study, the authors concluded the impact strength of heat-activated polymethylmethacrylate resin reinforced with silver nanoparticle in the ratio of 4:1,3:1,2:1 by weight was found to be 1.45 J/mm, 1.53 J/mm and1.99 J/mm, which was statistically significant compared to conventional heat-activated polymethylmethacrylate resin. Hence the impact strength of heat polymerized denture base resin was increased by the addition of silver nanoparticles.
Acknowledgement: Nil
Financial support: Nil
Conflicts of interest: The authors declared that there is no conflict of interest.

References:
1.Jancar J, Hynstova K, Pavelka V.Toughening of denture base resin with short deformable fibres.Comp Sci Technol.2009;69:457-62.
2.Fernanda CPPS, Heitor P, Vieira A, Garcia LFR, Consani S.Impact and fracture resistance of an experimental acrylic polymer with elastomer in different proportions. Mater Res. 2009;12:415-18.
3.Hargreaves AS.polymethylmethacrylate as a denture base material in service. J Oral Rehabil. 1975;2:97-104.
4.O’Brien WJ.Dental materials and their selection. 2nd ed. Chicago (IL).Quintessence Pub.1997; 5:85-86.
5.Hari PA, Kalavathy DS, Mohammed HS. Effect of glass fibre and silane treated glass fibre reinforcement on the impact strength of maxillary complete denture. Ann Essences dent. 2011;3:7-12.
6.Ahmed MA, Ebrahim MI.Effect of zirconium oxide nanofillers addition on the flexural strength, fracture toughness, and hardness of heat-polymerized acrylic resin.World J Nano Sci Eng. 2014;4:50-57.
7.Gupta A, Tewari RK.Evaluation and comparison of transverse and impact strength of different high strength denture base resins.Indian J Dent Res. 2016;27:61-65.
8.Vojdani, M,Khaledi AAR.Transverse strength of reinforced denture base resin with metal wire and E glass fibres. J Dent Teh Univer Med Sci. 2006;3:159-166.
9.Engelmeier RL.The history and development of posterior denture teeth-introduction, part II: Artificial tooth development in America through the nineteenth century.J Prosthodont. 2003;12:288-301.
10.Rama KA, Suresh S, Venkata RA, Kishore G, Nagaraj U. Influence of Fiber Reinforcement on the Properties of Denture Base Resins. J Biomat Nanobiotech. 2012;4:91-7.
11.Correa JM,Morie M,Sanches HL,Da Cruz AD,Poiate E Jr,Poiate IA.Silver nanoparticles in dental biomaterials.Int J Biomater. 2015;1:1-9
12.Furno F et al.Silvernanoparticles and polymeric medical devices: a new approach to prevention of infection. J Antimicrob Chemother. 2004;54:1019-24.
12.Schreiber CK.Polymethylmethacrylate reinforced with carbon fibers.Br Dent J. 1971;130:29-30.
13. Phoenix RD.Denture base materials.Dent Clin North Am. 1996,40;113-120.
14.Dogan OM,Bolayir G,Keskin S, Dogan A, Bek B, Boztug A.The effect of esthetic fibres on the impact resistance of a conventional heat-cured denture base resin.Dent Mat J. 2007;26:232-239.
15.Memon MS,Yunus N,Razak AA.Some mechanical properties of a highly cross-linked, microwave-polymerized, injection-moulded denture base polymer.Int J Prosthodont. 2001;14:214-18.
16.Straioto FG,Ricomini Filho AP, Fernandes Neto AJ,Del Bel Cury AA. Polytetrafluorethylene added to acrylic resins: mechanical properties. Braz Dent J. 2010;21:55-59.
17.Giampaolo ET, Pavarina AC.Effect of reline material and denture base surface treatment on the impact strength of a denture base acrylic resin.Gerodontology. 2010;27:62-69.
18.Begum SS, Ajay R, Devaki V, Divya K, Balu K, Kumar PA. Impact strength and dimensional accuracy of heat-cure denture base resin reinforced with ZrO2 nanoparticles: An in vitro study. J Pharm Biol Sci. 2019;11:S365-70.
19.Abdulkareem MM, HatimNA.Evaluation of the biological effect of adding aluminium oxide, silver nanoparticles into microwave treated PMMA powder.Int J En Res Sc Tech Eng . 2015;4:172-78.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License