IJCRR - 4(16), August, 2012
Pages: 108-115
Print Article
Download XML Download PDF
STUDY OF SERUM ADENOSINE DEAMINASE AS AN EFFECTOR OF OXIDATIVE STRESS IN DIABETES MELLITUS TYPE 2
Author: B. Sree Hari Babu, D.Lakshmi Lalitha, P.K Behera, D.S.S.K Raju
Category: Healthcare
Abstract:Diabetes Mellitus (DM) is the most common disorder characterized by metabolic abnormalities and long term complications. Hyperglycemia is considered a primary cause of diabetic vascular complications and is associated with oxidative stress. The purpose of this study was to investigate the role of hyperglycemia in generating oxidative stress if any, in DM Type 2. The study was carried out in 55 patients of DM Type 2 and also in 50 healthy controls. The patients were divided into two groups Group I (n=35) comprising patients of DM Type 2 with out complications and Group II (n=21) comprising patients of DM Type 2 with complications. Various parameters like Adenosine Deaminase (ADA) activity which is found to be a marker of abnormal lymphocyte response and a producer of reactive oxygen species (ROS), Malondialdehyde (MDA) which is a parameter to study increased oxidative stress leading to lipid peroxidation and Superoxide dismutase (SOD) activity which is an indicator of antioxidant status were taken into consideration to establish the existence of oxidative stress in DM Type 2. Glycosylated hemoglobin (HbA1c) was also assessed to determine the status of diabetic control. The parameters like HbA1c, serum ADA and serum MDA were significantly raised in DM Type 2 cases (both Group I and Group II) when compared to controls. Likewise the mean serum SOD was significantly lower in DM Type 2 patients (both Group I and Group II) as compared to Control group. When the levels of HbA1c, serum ADA and serum MDA in Group II patients of DM Type 2 when compared with those of Group I patients of DM Type 2, they were significantly increased. Likewise the serum SOD in Group II patients of DM Type 2 registered a significant decline as compared to Group I patients of DM Type 2. These alterations in DM Type 2 especially in Group II are ascribed to increased glycation, T-lymphocyte response, oxidative stress and limited defense against the radicals ,which act as harbinger of various metabolic complications.
Keywords: HbA1c; ADA; MDA; SOD; Oxidative stress; Lipid Peroxidation.
Full Text:
INTRODUCTION
Diabetes mellitus (DM) is a complex metabolic disorder characterised by chronic hyperglycemia with disturbances of carbohydrate, lipid and protein metabolism resulting from defects in insulin secretion, insulin action or both. DM Type 2 is a heterogenous group of disorders characterised by variable degrees of insulin resistance and impaired insulin secretion contributing to hyperglycemia. The metabolic dysregulation associated with DM causes secondary pathophysiological changes in multiple organ systems that impose a tremendous burden on individual. It is the leading cause of end stage renal disease, non traumatic lower extremity amputation and adult blindness.With an increasing incidence world wide, DM is likely to continue to be a leading cause of morbidity and mortality. The identification of distinct pathogenic processes in DM Type 2 has important potential therapeutic implications. Hyperglycemia, which is due to insulin resistance, impaired insulin secretion and increased glucose production resulting from environmental and genetic factors acting together is considered as the diagnostic parameter1 . The long term control of DM is judged by levels of glycated hemoglobin (HbA1c). The purpose of this study was to investigate the role of hyperglycemia in generating oxidative stress, if any, in Type 2 DM. To this effect, various parametes like Adenosine Deaminase (ADA) activity which is found to be a marker of abnormal lymphocyte response and a producer of reactive oxygen species (ROS), Malondialdehyde (MDA) which is a parameter to study increased oxidative stress leading to lipid peroxidation and Superoxide dismutase (SOD) activity which is an indicator of antioxidant status were taken into consideration, to establish the existence of oxidative stress in DM Type 2.
MATERIALS AND METHODS
The study comprised of 55 patients between age groups 45-65 years of both sexes of DM Type 2 reporting to MIMS, Nellimarla, Vizianagaram for treatment.The patients were divided into Group I (DM Type 2 without complications) and Group II (DM Type 2 with complications). The criteria for the diagnosis of DM were the same as the one which was given by the National Diabetes Data Group 1999. 50 healthy subjects of similar age, sex and socioeconomic status served as controls.The controls were free from any major ailment which could alter the parameters under study. Informed consent was taken from the patients and subjects who participated in the present study. Institutional ethical committee approval has also been obtained. Blood was drawn in the fasting state for Fasting Blood Sugar (FBS) in the fluoridated vial. For HbA1c estimation, the sample was collected in heparinized vial.The samples were collected in plain vials for the estimation of serum ADA, MDA and SOD.Sera were separated from samples and analysis was done. FBS was estimated by GOD-POD method (Trinder 1969)2 .HbA1c was estimated by the method of Trivelli et al 19793 .ADA was estimated by the method of Giusti 19844 .MDA was measured by colorimetric assay with 2- thiobarbituric acid by the method of Satoh 19785 . SOD was estimated by the method of Kakkar et al 19846 .
DISCUSSION
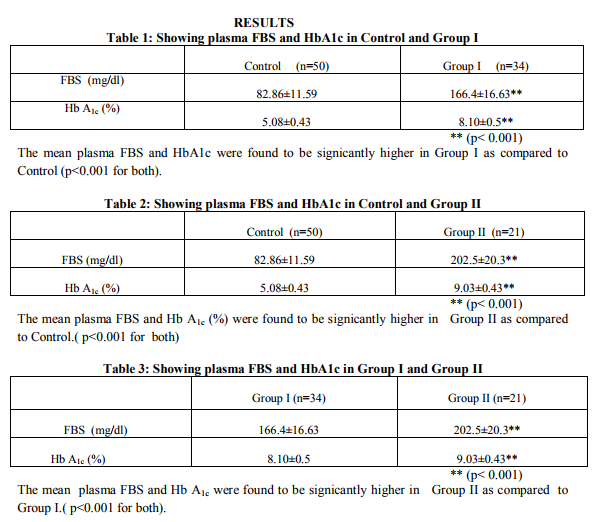
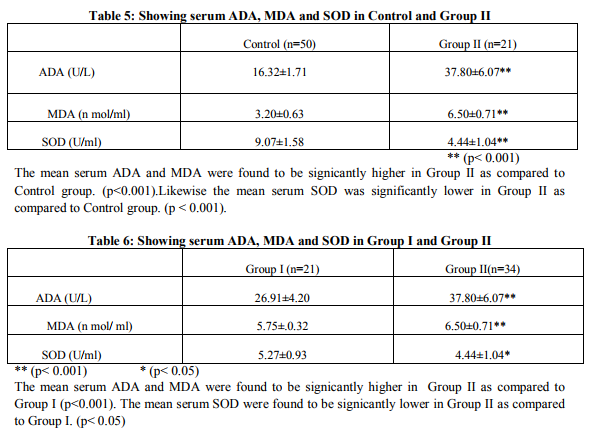
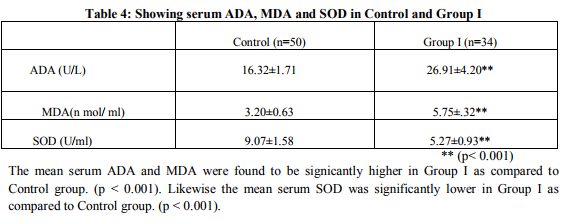
The diagnosis of DM in the present study was based on criteria issued by consensus panel of experts from National Diabetes Data Group (NDDG) 19797 and World Health Organisation (WHO) 19808 , According to these criteria, DM was diagnosed on the basis of the fasting plasma glucose ≥ 126 mg/dl and symptoms of diabetes. The classic symptoms of DM include polyuria, polydypsia, polyphagia and unexplained weight loss. The principal complications associated with DM are retinopathy, neuropathy, nephropathy, angiopathy, susceptibility to infection, dyslipidemia, ketoacidosis and hyperosmolar hyperglycemic non ketotic coma. It is observed that in the present study the mean fasting plasma glucose level was significantly raised in both Group I without complications(166.4mg/dl±16.63) and Group II with complications (202.5 mg/dl±20.3) as compared to Control Group(82.86 mg/dl ±11.59). This rise is statistically significant (p<0.001; Table 1&2). The mean values of FBS in both the groups confirmed to the criteria laid down by WHO for diagnosis of DM. The comparison of plasma FBS between Group I and Group II (Table 3) established a higher level in the later and the increase was statistically significant (p< 0.001). Hyperglycemia is due to insulin resistance, impaired insulin secretion and increased glucose production resulting from environmental and genetic factors in DM Type2. The long term control of DM is judged by levels of glycated hemoglobin (HbA1c). Glucose reacts spontaneously and non- enzymatically with free amino groups on hemoglobin (Hb) to form covalent glycated hemoglobin. The extent of glycation depends on the average blood glucose to which hemoglobin is exposed and on the half life of hemoglobin. Several glycated derivatives of hemoglobin exist, derived from the reaction of Hb with glucose, glucose6phosphate etc. These are collectively known as HbA1. The principal constituent of HbA1 is the one formed with glucose itself, termed as HbA1c, which normally comprises about 5% of circulating hemoglobin (Becket et al 2006)9 . It is observed that in the present study the mean Hb A1c level was significantly raised in both Group I (8.10%±0.5) and Group II (9.03%±0.43) as compared to Control Group (5.08%±0.43) This rise is statistically significant (p<0.001;Table 1&2 ). The mean values of HbA1c in both the groups exceeded 5%. HbA1c once formed stays within the red cell for its life time. Since half life of the red cell is 60 days, HbA1c value reflects the average level of blood glucose over the previous 1-2 months. The comparision of HbA1c between Group I and Group II (Table 3) established a higher level in the later and the increase is statistically significant (p< 0.001) indicating poor diabetic control responsible for the incidence of micro and macro vascular complications. ADA is an enzyme of purine metabolism. It acts on adenosine and other adenosine nucleoside analogues. It plays a crucial role in lymphocyte proliferation and differentiation (Hovi 1976)10, and shows highest activity in Tlymphocytes (Sullivan 1977)11. It is an enzyme distributed in the human tissues and was considered as a good marker of cell mediated immunity (Baghanha 1990)12 . It is observed that in the present study the mean serum ADA is significantly increased in both Group I (26.91 U/L ±4.20) and Group II (37.80 U/L ±6.07) as compared to Control Group (16.32 U/L±1.71). This increase is statistically significant ( p<0.001 ;Table 5) . Hoshino et al 199413 , Kurthul et al 200414, Prakash et al 2006 15 and Mokthari et al 2010 16 reported in their study an increased level of serum ADA associated with hyperglycemia in DM Type2.High serum ADA activity in DM Type2 might be due to abnormal T-lymphocyte responses or proliferation and its release into circulation which depends on altered insulin levels (Shivaprakash et al 2006)15. This increased level of ADA in diabetic patients could result in increased hypoxanthine which oxidizes into xanthine and uric acid by xanthine oxidase and concomitant generation of free radicals (Siddiqi et al 2011)17. The comparision of serum ADA between Group I and Group II (Table 6) established a higher level in the later and the increase is statistically significant (p< 0.001) indicating an increased T-lymphocyte proliferation and free radical production in DM Type 2 with complications. It is observed that in the present study the mean serum MDA was significantly increased in Group I (5.75 n mol/ml±.0.32) and Group II (6.50 n mol/ ml ± 0.71) ) when compared to Control Group (3.20 n mol/ ml ±0.63). This increase is statistically significant (p < 0.001; Table 4, 5). The various mechanisms included in the increase of serum MDA in DM Type 2 include: a) Chronic Hyperglycemic status in Diabetes mellitus Type 2 favours auto oxidation of glucose which is subjected to enediol rearrangements that result in the formation of an enediol radical anion. (Githanjali et al2010)18 . b) Chronic Hyperglycemic status in Diabetes mellitus Type 2 also favours non enzymatic glycation reaction thereby leading to advanced glycosylation end products (AGE). Glycation of proteins can lead to direct release of O2 - (superoxide radical) and hydrogen peroxide through specialized receptors for AGE (Abuja and Albertini 2001)19 . c) Increased level of serum ADA in diabetic patients could result in increased hypoxanthine which oxidizes to xanthine and uric acid and accompanying generation of free radicals. (Siddiqi et al 2011)17 . The free radicals generated by above reactions are exteremely reactive.When a free radical reacts with a normal compound; other free radicals are generated through propagation phase. Peroxidation of poly unsaturated fattyacids in plasma membrane by free radicals leads to loss of membrane functions.Lipid peroxidation and consequent degradation products such as malondialdehyde are seen in biological fluids (Vasudevan 2011)20. The comparison of MDA between Group I and Group II (Table 6) established a higher level in the later and the increase is statistically significant (p< 0.001) indicating more lipid damages leading to the destruction of fine architecture and integrity of the membranes responsible for its complications. SOD is an enzyme that repairs cells and reduces the damage done to them by free radicals by its antioxidant properties.It is observed that in the present study the mean serum SOD is significantly decreased in Group I (5.27 U/ml ±0.93) and Group II (4.44 U/ml ±1.04) when compared to Control Group (9.07 U/ml ±1.58). This decrease is statistically significant (p < 0.001; Table 4, 5).It has been reported that diabetic patients have significant defects of antioxidant protection (Aria et al 1989, Lin 1996 and Zbronska et al 1995) as manifested by a decrease in serum SOD. This decrease can be explained as follows: a) The decrease of superoxide dismutase activity might be due to the increase of glycosylated SOD that leads to the inactivation this enzyme (Aria et al 1989)21 b) The SOD activity is further decreased due to loss of its cofactors Zn2+ and Cu2+ in DM Type 2 (Lin 1996, Zbronska et al 1995) 22 ,23 . The comparison of SOD between Group I and Group II (Table 6) established a lower level in the later and the decrease is statistically significant (p< 0.05) indicating lowered antioxidant status in DM Type 2 with complications.
CONCLUSION
In the present study, it has been established that the various complications in DM Type 2 may be linked to the alteration in two of the biochemical parameters: HbA1c.and free radical generation. Statistically significant increase in HbA1c in complicated DM Type 2 in comparison to uncomplicated DM Type 2 indicates an improper diabetic control which is responsible for the higher incidence of micro and macro vascular complications. High serum ADA activity, formation of enediol radical ion and advanced glycosylation end products contribute to the generation of excess free radicals, as evidenced by a statistically significant rise in serum MDA and are responsible for inflicting gross damage to cell membranes and initiating as well as aggravating various complications of DM Type 2.The significant decrease of SOD in DM Type 2 as explained also contributes to the damage caused by the free radicals because of the curtailed defensive mechanism against them.
ACKNOWLEDGEMENT
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors /publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed
References:
1. Braunwald E, Fauci AS, Kasper DL, Hauser SL, Longo DL, Jamesor JL. Harrison’s principles of Internal Medicine Mc Graw Hill .2003;333: 2109-2105. 2. Trinder P. Blood sugar estimation by GODPOD method. Ann. Clin. Biochem.1969; 6: 24-27.
3. Trivelli, LIA.et al Glycosylated Hemoglobin estimation by Ion Exchange Resin Method .New Eng.J.Med 1971; 284:353.
4. Giusti G, Galanti B. Colorimetric method.Adenosine deaminase In: In Bergmeyer Hu, (Ed). Methods of enzymatic analysis, 1984; 3rd ed. Weinheim: Verlag chemie: 315-24
5. Satoh K. Serum lipid peroxide in cerebro vascular disorders determined by a new colorimetric method. Clin.Chim.Acta 1978; 90: 37-43.
6. Kakkar P, Das B, Viswanathan PN. “A modified spectrophotometric assay of superoxide dismutase”. Ind J Biochem Biophysics 1984; 21: 130-2.
7. Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. National Diabetes Data Group. Diabetes .1979; 28:1039–57.
8. WHO Expert Committee on Diabetes Mellitus: second report. World Health Organ Tech Rep Ser. 1980; 646: 1–80.
9. Geofrey Becket, Simon Walker, Peter Rae, Peter Ashby .Lecture notes, Clinical Biochemistry, 2006;7: 152.
10. Hovi T, Smyth JF, Allison AC,Williams SC.Role of adenosine deaminase in lymphocyte proliferation.Clin Exp Immunol 1976;23:395-403.
11. Sullivon JL, Oxborne WRA, Wedgewood RJ.Adenosine deaminase in activity in lymphocytes.Br J Haematol1977;37:157-8.
12. Baghanha MF,Pego A,Lima MA et al.Serum and pleural adenosine deaminase correlation with lymphocyte populations.Chest 1990;87:605-10.
13. Hoshino T, Yamada K, Masuoka K, et al. Elevated adenosine deaminase activity in the serum of patients with DM. Diabetes Res Clin Pract 1994; 25: 97-102.
14. Kurthul N, pence S, Akarsu E et al.Adenosine deaminase activity in the serum of type 2 diabetis patients.Acta Medica (HradecKralove) 2004; 47(1):33-5.
15. Shiva Prakash M, Chennaiah S,Murthy YSR,Anjaiah E,Anandha Rao S,Suresh C ,Altered Adenosine Deaminase Activity in Type 2 Diabetes Mellitus, JIACM 2006; 7(2): 114-17.
16. Mokhtari M, Hashemi M, Yaghmaei M, Molashahi F, Shikhzadeh A, Niazi A, Ghavami S. Serum adenosine deaminase activity in gestational diabetes mellitus and normal pregnancy. Arch Gynecol Obstet. 2010; 281:623–626.
17. Siddiqi SS, Ahmad J, Islam N, Ashraf SMK, Mishra SP. A Study on the Modulation of Adenosine Deaminase (ADA) Activity in Monocytes of Type 2 Diabetic Patients by Antioxidants. JIACM 2011; 12(2): 113-6
18. Gitanjali G,Sudeep G,Neeraja,Mili G,Deepak A, Priyanka S. The effect of hyperglycemia on some Biochemical parameters in Diabetes Mellitus.Journal of Clinical and Diagnostic Research, october 2010; 4: 3181-3186.
19. Abuja PM, Albertini R. Methods for monitoring oxidative stress, lipid peroxidation and oxidation resistance of lipoproteins. Clin Chim Acta. 2001 Apr; 306(1-2):1-17.
20. Vasudevan DM, Sreekumari S, Vaidyanadhan K, Text book of Biochemistry.Jaypee Brothers Medical Publishers 2011;20:239.
21. Aria K, Lizuka S, Tada Y, Oikawa K, Taniguch N. Increase in the glucosylated form of erythrocyte Cu, Zn-superoxide dismutase in diabetes and close association of the nonenzymatic glucosylation with the enzyme activity. Biochem Biophys Acta 1989; 924:292 – 6.
22. Lin J. The association between copper ions and peroxidativereaction in diabetic cataract. Nippon Ganka Gakkai Zasshi1996;100 (9):672 – 9.
23. Zbronska H, Grzeszczak W, Jendryczko A, Zbronski R, Kuzniewicz R. Activity of superoxide dismutase in erythrocytes and leukocytes and levels of zinc and copper in blood of patients with diabetes. Effects of diabetic treatment on examined parameters. Pol Arch Med Wew 1995; 94(3):228 – 34.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License