IJCRR - 6(1), January, 2014
Pages: 53-62
Print Article
Download XML Download PDF
DISTALLY BASED SURALIS FASCIOCUTANEOUS FLAP IN THE ARMAMENTARIUM OF THE ORTHOPAEDIC TRAUMA SURGEON
Author: Mohammed Lafi Al-Otaibi
Category: Healthcare
Abstract:Introduction: To present the experience of an Orthopaedic Surgeon, certified consultant with no microsurgery or plastic surgery qualification working at a level one trauma center in managing soft tissue coverage of lower one third of tibia, ankle and the heel. Patients and Methods: Four patients, three males and one female, with soft tissue defect of lower one third tibia, ankle and the Heel requiring soft tissue cover were treated from August 2008 to August 2010. The Distally based suralis fasciocutaneous flap was harvested from the posterior aspect of the calf. The pedicle pivot is at least 5 cm proximal to the lateral mallelous to allow anastomosis with the peroneal artery via the constant peroneal perforators. Skin incision was started along the mid line of the calf posteriorly stoping 5 cm at least proximal to lateral malleolus which the fascial pedicle would be taken. The subdermal layer dissected to expose the sural nerve, accompanying superficial sural vessels and short saphenous vein.1 The subcutaneous facial pedicle elevated, with a width of 3cm to include the nerve and these vessels will pivot. At the proximal margin of the flap, the nerve and the vessels were ligated and severed.2 The skin island was elevated with the deep fascia. The donor site defect was covered with a split thickness skin graft from epsilateral thigh. Results: Well tolerated procedure by all patients, no plastic surgery or reoperation was need for any of the four cases, Survival of all flaps, maintenance of orthopaedic fixation, one flap showed some venous engorgement which subsided gradually in a few days. Complete take of all split skin graft over donor site bed. Conclusion: Distally based Sural artery flap is a good choice for reconstruction of soft tissue defects of lower 1/3 tibia, ankle and foot. The procedure is easy and should be done by an Orthopaedic surgeon when needed.
Keywords: Soft tissue defects distally based sural artery flap, Lower 1/3 tibia, ankle & foot.
Full Text:
INTRODUCTION
Defects in Soft tissue accompanying fractures of lower 1/3 tibia, ankle and foot are a challenging problem facing orthopaedic surgeon's world wide. Hospitals with no plastic surgery departments where these patients usually being treated put there orthopaedic surgeons at the challenge.3 Distal third of tibia is subcutaneous and not forgiving in terms of soft tissue problems usually arise in situations such as open fractures or pilon fracture. Wound problems of the hind foot complicating Calcaneus fracture or after its open reduction and internal fixation is another challenging site for soft tissue coverage. Different forms of soft tissue cover are available e.g., Random cutaneous, arterial cutaneous (axial), musculocutaneous, muscle, fasciocutaneousand free flaps with their own indications, advantages and disadvantages. The distally based Sural artery flap, first described as a distally based neuro cutaneous flap by Masquelet et al.,4 is skin island flap supplied by the vascular axis of sural nerve. He reported, using colored latex injection studies in 1992, the blood supply to the skin from the arteries accompanying the nerves and described the concept of neuro cutaneous island flap. The objective of this paper was to present our experience of soft tissue cover of lower 1/3 of tibia, ankle and foot treated by an Orthopedic surgeon without any special training, and also the reliability of this flap.
PATIENTS AND METHODS
Approved by the Ethical Committee in our center four patients, three males and one female, with soft tissue defect of lower 1/3 tibia ankle and foot requiring soft tissue cover were treated from May 2008 to may 2010. The patient’s age ranged from 14 to 36 Years (mean 25 Years). Two of the wounds were over the distal third of the tibia, one on the lateral malleolus and one on the lateral aspect of hind foot. All four cases underwent same surgical technique as shown Figures 1 to 12. Donor flaps sutured in place or stabled over a haemovac drain and with no tension at the edges. The limb is warped in enough cotton and immobilized in Ankle foot orthosis to prevent pressure on the flap Fig -12. The procedure is done without tourniquet and all patients were given prophylactic dose of antibiotics, wounds inspected second post operative day as the drain removed. Oxygenation via face mask to keep saturation above 95% and assuring enough oxygen tention at the wounds as they heel. All patients kept in hospital until wounds heal and sutures removed.
RESULTS
The mechanism of injury was road traffic accident in three patients with open fracture tibia Fig-13 in two patients one is skeletally immature with growth plate injury Fig-14 and open ankle fracturein the third patient, the fourth case after operative treatment of fracture of the calcaneum complicated by wound necrosis Fig-15. Reveres flow suralis flap used in all cases (Table 1). All flaps survived.one flap showed slight venous congestion which subsided within a few days. Complete take of split skin graft over the donor site. No loss of sensation persisted at two years post op.
DISCUSSION
Previously, mostly lower limb flaps were based on the concept of random skin flap design, thus were limited by a certain length-to-width ratio (usually 1:1 in the lower extremity). Ponten flaps had length-to-width ratios as great as 3:1. These flaps have been referred to as Ponten super flaps. The concept of a neuroskin island flap has been first developed and applied by Masquelet4 as he reported its use in six clinical cases for coverage of some specific areas of the lower limb and gained attention since 1992. Cormack and Lamberty classified fasciocutaneous flaps according to their vascular anatomy.5 Mathes and Nahai also discussed the classification of fasciocutaneous flaps.6 Tolhurst, Haeseker, and Zeeman demonstrated a 15% greater survival length in flaps that included fascia.7 Cormack and Lamberty classified fasciocutaneous flaps based on vascular anatomy.Circulation to a fasciocutaneous flap is based on the prefascial and subfascial plexuses. There are also arterial plexuses at the subdermal and subcutaneous levels. These plexuses are supplied by regional arteries that may enter the deep fascia through an underlying muscle (musculocutaneous), through the septum between underlying muscles (septocutaneous), or through a direct cutaneous branch. Often, more than one source of blood supply to a particular area of skin or a particular muscle is present. If one of these arteries is ligated, the skin and fascia continue to receive blood supply from an alternative source. The arteries generally are accompanied by paired venae comitantes and are reasonably consistent in their location. In the extremities, many perforators pierce the septa between long slender muscles, while musculocutaneous perforators tend to supply the skin over the broad flat muscles of the trunk. Because of the directionality of the fascial plexus, particularly in the extremities, the orientation of the flap is important. Chan and colleagues8 in their study proved that early vascularized soft-tissue closure has long been recognized to be essential in achieving eventual infection-free union. The question of whether muscle or fasciocutaneous tissue is superior in terms of promoting fracture healing remains unresolved. In this article, the authors review the experimental and clinical evidence for the different tissue types and advocate that the biological role of flaps should be included as a key consideration during flap selection. Ebrahimi et al.9 concluded that reverse sural flap is a useful and versatile reconstructive method in patients with gunshot wounds of the lower leg and foot. Mukherjee et al.10 studied prospectively 20 cases and fined that Perforator flaps are a reliable option for closure of soft tissue defects of lower limb irrespective of size, location and depth. There is minimal donor site morbidity. It has the advantage of rapid dissection, flap elevation and reliable skin territory. As no special equipment is required it can be replicated in smaller centers also. Zayakova11 as other researchers proved the pedicle fascio cutaneous and muscle flaps are used in reconstructive surgery to treat large and deep defects of the lower leg. Full tissue coverage, functional recovery and good aesthetic results are achieved with minimum damage to the donor site. In addition, the surgical procedure is relatively short and easy to perform, and it doesn’t require microsurgical skills and instruments. Esezobor et al.12 mentioned in their study, though the loss of sensation on the area innervated by the sural nerve may resolve within some months after the use of reverse sural artery flap, preserving sensation on the foot is an advantage especially in patient with sensoneural problem. In some selected patients that require flap cover for the upper part of the distal 3rd and the mid 3rd on the ipsilateral leg, the sural nerve preserving sural artery flap is an option. Its area of coverage on the contralateral leg may extend to the whole of distal 3 rd. This is possible as long as the pivot of the flap is not more than 5cm distal to the level of the point where the sural nerve pierces the deep fascia and the arc of rotation is not more than 100°. Elsaftawy et al.13 reported 16 cases and find the reverse sural flap, technically easy, offers a viable, low-risk alternative to free and perforator-based flaps. Proving carrying the lowest risk of complication and failure. Chen Wang et al.14 concluded in a study involving 16 consecutive cases that The distally based flap pedicled with the lateral sural nerve and lesser saphenous vein was a reliable source for repairing soft tissue defects in the lower leg and foot due to its advantages of infection control, high survival rate, and sufficient blood supply without the need to sacrifice a major blood vessel Chang et al.15 stated that the reconstruction of the distal third leg and weight-bearing heel, especially when complicated with infection and / or dead space, remains a challenge in reconstructive surgery. The distally based sural neurofasciomyocutaneous flap has been proved a valuable tool in repair of the soft tissue defects of those areas. a modified distally based sural neurofasciomyocutaneous flap including the distal gastrocnemius muscle component was designed and used for repairs of the soft tissue defects in the distal lower limb and plantar heel pad in six patients. The blood supplies of flaps comprised either the peroneal perforator and adipofascial pedicle or the peroneal perforator only.
CONCLUSION
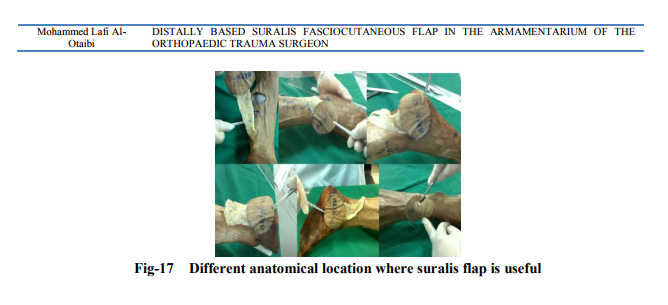
Distally based Sural artery flap is a good choice for reconstruction of soft tissue defects of lower 1/3 tibia, ankle and foot (Fig 17). The procedure is easy and should be done by an Orthopaedic surgeon when needed.











References:
REFERENCES
1. Motamed S, Yavari M, Mofrad HRH, Reza R, Shahraki FN. Distally based sural artery flap without sural nerve. Acta Medica Iranica 2010; 48(2): 127-9.
2. Ali MA, Chowdhury P, Ali M, Ifteker Ibne Zuha, Dev J. Distally-based sural island flap for soft tissue coverage of ankle and heel defects. J Coll Physicians Surg Pak. 2010; 20(7): 475-7.
3. Ponten B. The fasciocutaneous flap: its use in soft tissue defects of the lower leg. Br J Plast Surg. 1981; 34(2):215-20.
4. Masquelet AC, Romana MC, Wolf G. Skin island flaps supplied by the vascular axis of the sensitive superficial nerves: anatomic study and clinical experience in the leg. Plast Reconstr Surg. 1992; 89(6):1115-21.
5. Cormack GC, Lamberty BG. A classification of fascio-cutaneous flaps according to their patterns of vascularisation. Br J Plast Surg. 1984; 37(1):80-7.
6. Mathes SJ, Nahai F. Reconstructive Surgery: Principles, Anatomy, and Technique. New York: Churchill Livingstone; 1997.
7. Tolhurst DE, Haeseker B, Zeeman RJ. The development of the fasciocutaneous flap and its clinical applications. Plast Reconstr Surg. 1983; 71(5):597-606.
8. Chan JK, Harry L, Williams G, Nanchahal J. Soft-tissue reconstruction of open fractures of the lower limb: muscle versus fasciocutaneous flaps Plast Reconstr Surg. 2012; 130 (2): 284e-295e.
9. Ebrahimi A, Nejadsarvari N, Koushki ES. Experience With Reverse Sural Flap to Cover Defects of the Lower Leg and Foot. Trauma 2012; 16(4): 178-81.
10. Mukherjee MK, Parwaz MA, Chakravarty B, Langer B. Perforator flap: A novel method for providing skin cover to lower limb defects. Medical Journal Armed Forces India 2012; 68: 328-34.
11. Zayakova YK. Application of pedicle flaps for wound coverage of lower leg. J IMAB 2013, 19(1):382-386; DOI: 10.5272/jimab.2013191.382.
12. Esezobor EE, Nwokike OC, Aranmolate S, Onuminya JE, Abikoye FO. Sural nerve preservation in reverse sural artery fasciocutaneous flap-a case report. Ann Surg Innov Res. 2012; 6(1):10. doi: 10.1186/1750- 1164-6-10.
13. Elsaftawy A, Jab?ecki J, Domanasiewicz A, Paruzel M, Kaczmarzyk J, Kaczmarzyk L. Treatment possibilities of reverse-flow sural flap in covering the defects of lower extremities. Pol Przegl Chir. 2013; 85(4):192- 7. doi: 10.2478/pjs-2013-0029.
14. Wang C, Xiong Z, Xu J, Huang H, Li G. The distally based lateral sural neuro-lesser saphenous veno-fasciocutaneous flap: anatomical basis and clinical applications J Orthopaed Traumatol. DOI 10.1007/s10195- 012-0202-2.
15. Chang SM, Zhang K, Li HF, Huang YG, Zhou JQ, Yuan F, Yu GR. Distally based sural fasciomyocutaneous flap: anatomic study and modified technique for complicated wounds of the lower third leg and weight bearing heel. Microsurgery. 2009; 29(3): 205-13. doi: 10.1002/micr.20595.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License