IJCRR - 6(3), February, 2014
Pages: 07-15
Print Article
Download XML Download PDF
A COMPARATIVE STUDY OF EARLY ONSET VERSUS LATE ONSET NEONATAL SEPSIS WITH SPECIAL REFERENCE TO BACTERIOLOGICAL, DEMOGRAPHIC AND CLINICAL PROFILE
Author: Kuhu Pal, Arnab Kumar Samanta, Ritesh Singh
Category: Healthcare
Abstract:Introduction: Neonatal sepsis is classically divided into early onset sepsis (EOS) and late onset sepsis (LOS) depending upon the time of onset of sepsis. Aims: To determine the differences in bacteriological, demographic and clinical profile between EOS and LOS, if any. Setting and Design: A prospective study was carried out in a tertiary care centre of Eastern India from March 2011 to February 2012. Methods: Neonates with less than 28 days age, associated with a clinical diagnosis of sepsis were included in the study. Blood was collected aseptically for culture and isolates were identified in conventional way and antibiotic sensitivity test was done by Kirby Bauer disc diffusion method. Epidemiological parameters, clinical features were compared in the light of culture report. Statistical analysis used: Chi square test, ANOVA and multivariate regression analysis. Results: Out of 230 clinically suspected septic neonates, 72.6% of neonates presented with EOS and 27.4% with LOS. None of the bacteria except Klebsiella sp. was significantly associated with EOS (P=0.043). Almost identical result was observed between EOS and LOS, when demographic parameters including gender, birth weight, gestational age, mode of delivery, outcome and clinical presentation were compared. Caesarean section was significantly associated with increased morbidity in cases of EOS (multivariate P value 0.018). Conclusion: There was no statistically significant difference in epidemiological, clinical and bacteriological profile between EOS and LOS except a few. So it is better to judge the two groups of neonatal sepsis as one and universal.
Keywords: Demography, Early onset sepsis, Late onset sepsis, Microbiological spectrum
Full Text:
NTRODUCTION
Neonatal Sepsis is defined as a clinical syndrome characterized by signs and symptoms of systemic infections accompanied with bacteraemia in the first month of life.[1] Symptoms occurring within the age of 3 days are considered as early onset sepsis (EOS). Late onset sepsis (LOS) usually occurs after 3 days of life. This distinction has thought to have a clinical relevance, due to difference in peripartum pathogenesis.[2] In EOS neonates acquire infection by the organisms colonized in mothers’ genitourinary tract. But late onset sepsis is either nosocomial or community acquired.[3] But, this conventional difference may not be relevant today, as alteration in genital flora by intrapartum medication or prolonged hospital stay and failure to maintain proper asepsis during delivery may lead to intermixing of causative agents of EOS and LOS.[4,5] The aim of the study was to evaluate the microbiological, demographic, and clinical characteristics of EOS and LOS and to determine the differences in these two groups of neonates if any.
MATERIALS AND METHODS
Study design: This was a hospital based singlecentred prospective study. Study area: Study was carried out in the Neonatal Care Unit, Department of Paediatrics of a tertiary care centre of eastern part of Bengal. Study population: Neonates with less than 28 days age, with clinical signs of sepsis, including refusal of feed, lethargy, respiratory distress, abdominal distension, vomiting, hypothermia etc born inside this hospital as well as referred from different centres were enrolled in this study. Exclusion criteria: Babies who had received antibiotics before collection of blood samples, having surgical problems, chromosomal or congenital anomalies were excluded from the study. Neonates who were referred to higher centres or who left the hospital against medical advice before proper diagnosis were also excluded from the study. Study period: March 2011 to February 2012. Study was carried out after getting permission from Institutional Ethics Committee. Written informed consent was obtained from parents/guardians of neonates who participated in this study. Procedure: Each neonate was assessed by a paediatric resident. Medical records of all neonates with suspected sepsis were reviewed for demographic characteristics (birth weight, gestational age, gender, type of delivery, associated risk factors) and babies were followed till recovery or death. 2 ml of blood was collected maintaining proper aseptic technique and 1ml was inoculated in 5 ml of brain heart infusion broth with 0.025 % sodium polyanethol sulfonate. Another 1ml was used for testing other haematological parameters. The blood culture broth was incubated aerobically at 370 C. Blind subculture was done on 24hrs, 48 hrs, 72 hrs, then on 7th day. Any sign of growth in between was followed by subculture. Media used for subculture were 5% sheep blood agar, chocolate agar and Mac Conkeys agar (Himedia Laboratories). In suspected cases of meningitis CSF was collected and cultured in chocolate agar and blood agar media. Isolates were identified by colonial morphology, Gram staining as well as standard biochemical tests. Aerobic spore bearers and diphtheroids, wherever grown were regarded as contaminants. The remaining isolates were included in the analysis. Antimicrobial sensitivity test was done by Kirby Bauer disc diffusion method following guidelines provided by Clinical and Laboratory Standards Institute (CLSI).[6] The clinical manifestations and demographic parameters were compared with blood culture reports. Presence of any of the clinical features was considered as indicator of morbidity. Statistical analysis: Percentages and Mean ± SD (Standard Deviation) were used to express the categorical variables and quantitative variables respectively. Differences in distribution were analysed by Chi square test and ANOVA. By multivariate regression analysis, Odds Ratio (OR) and 95% confidence interval for OR was also calculated. The statistical analysis was done using Statistical Package for Social Sciences (SPSS) version 16.0.
RESULTS
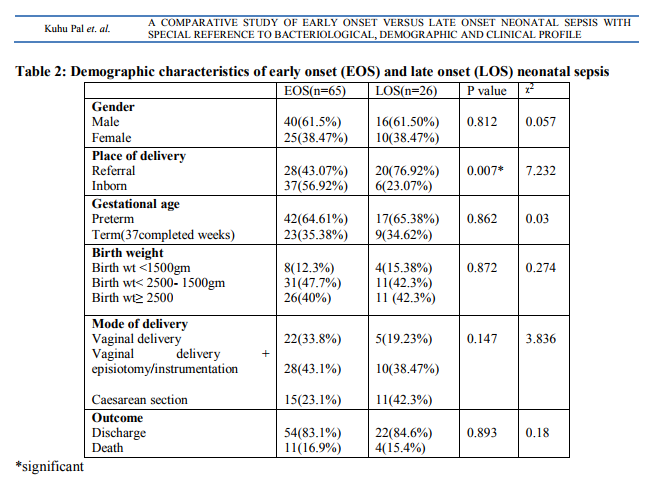
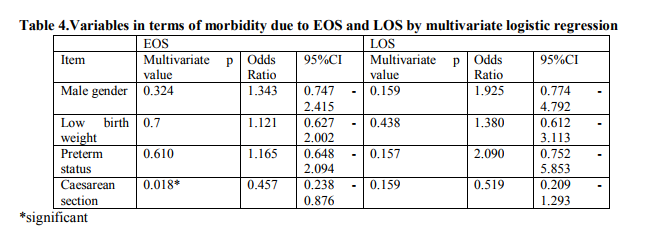
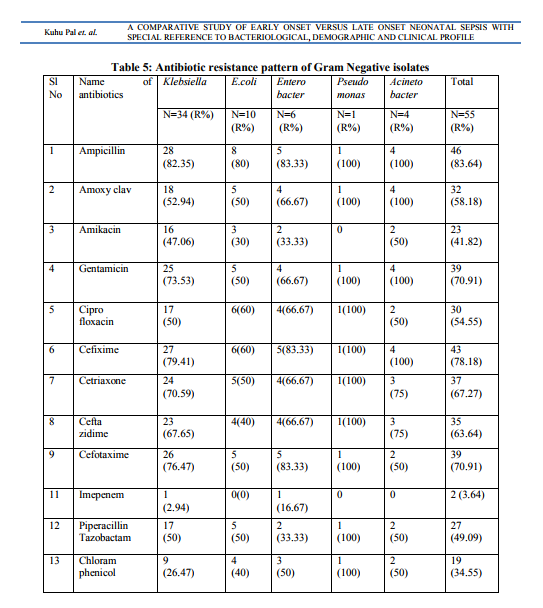
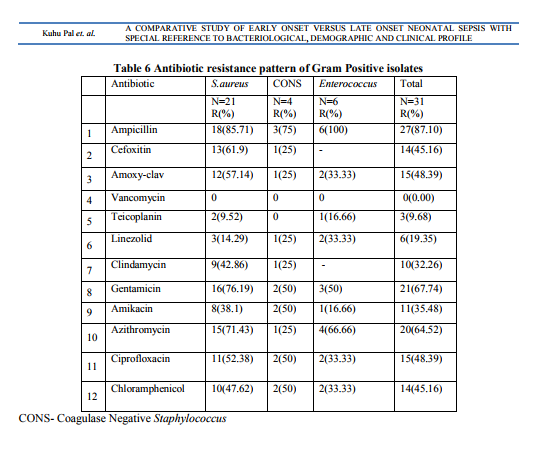
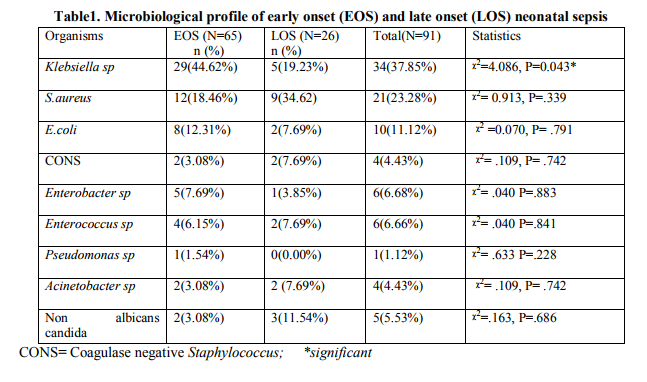
Two hundred and thirty neonates with suspected sepsis were followed. Incidence of EOS (167/230=72.6%) was more than LOS (63/230=27.4%) in this institution. Gram negative bacilli (GNB) were the major offender 45/65=69.2%) of EOS, whereas Gram positive cocci (GPC) were responsible for 50% (13/26) of LOS. Staphylococcus aureus was in the leading role (9/13=69.2%) in LOS. Klebsiella sp was the most common organism responsible for EOS followed by Staphylococcus aureus , E.coli , Enterobacter sp . The contribution of Klebsiella sp was more in EOS than LOS [29(44.62%) versus 5(19.23%), P value= 0.043]. The spectrum of organisms causing neonatal sepsis has been shown in Table 1. No particular organism was exclusively isolated from either EOS or LOS. Five CSF samples sent for bacteriological culture were found to be sterile. Demographic characteristics of EOS and LOS have been shown in Table2. There was no significant difference in different parameters of EOS and LOS except place of delivery. The neonates who had been referred from other centres were more prone to develop LOS. Male female ratio was 1.6:1 in both EOS and LOS. Mean Birth weight of babies with EOS was 2.3 ± 0.49 kg. Mean gestational age was 36 ± 2 weeks and these were almost similar in LOS group. Majority of newborns were delivered by vaginal delivery (76.9%) compared to caesarean section(CS) (23.1%) in EOS but reverse situation was observed in LOS, where 42.1% babies were delivered by CS. Mortality rate due to EOS and LOS remained almost equal. Majority of newborns with neonatal sepsis presented with refusal of feed (52.7%) and respiratory distress (24.1%). These features were true for both EOS and LOS (Table 3). Multivariate logistic regression analysis showed that morbidity was significantly higher in babies delivered by caesarean section in EOS group (P=0.018) only. No significant differences were seen in morbidity indicators based on the male gender, low birth weight, pre term status of the neonates (Table 4). Antimicrobial susceptibility testing from blood culture isolates revealed that Gram negative bacilli were highly resistant to ampicillin (83.64%), cefixime (78.18%), gentamicin (70.91%) and cefotaxime (70.91%). Pseudomonas sp and Acinetobacter sp showed resistance to almost all the common drugs used. Four of the Klebsiella sp and one E.coli were identified phenotypically as extended spectrum beta lactamase (ESBL) producers (9.09%). Almost 50% of the GNB were resistant to piperacillin – tazobactam, and amoxycillin- clavulanic acid. Imepenem was found to be the most sensitive drug followed by amikacin and chloramphenicol (Table 5). Gram positive cocci were also quite resistant to ampicillin (87.10%), azithromycin (64.52%) and gentamicin (67.74%). Thirteen (61.9%) Staphylococcus aureus were screened as Methicillin resistant Staphylococcus aureus (MRSA). But no Vancomycin resistant Staphylococcus aureus (VRSA) was reported (Table 6).
DISCUSSION
Among 230 suspected cases of neonatal sepsis blood culture was positive in 91 (39.56%) neonates. Of which incidence of EOS was 71.4%. This was in accordance with the studies done by V Sundaram,[5] M.N Shah,[7] A Hafsa,[8] but reverse result was seen in studies in Nepal,[9] South India,[10] Taiwan[11] and Johannesburg.[12] The causes of this discordance might be due to the fact that those centres were running as referral centres without facility of delivery and consideration of timeframe of EOS as 48hrs. Another possible explanation for a lower incidence of LOS in this study might be the early discharge policy of the neonatal unit. The most common organism causing EOS was found to be Klebsiella sp followed by Staphylococcus aureus, E. coli, whereas predominant organism in LOS was Staphylococcus aureus. This result was similar to a study done in northern India.[5] Pivotal role of enteric Gram negative bacilli especially Klebsiella sp in EOS was also ascertained in a couple of studies in Eastern India,[13,14] Bangladesh[8] and Nepal.[9] Along with Staphylococcus aureus, E.coli was the found to be responsible for LOS in a study in Nepal.[9] Studies from different parts of the world,[11,12,15,16] showed that Gram positive organisms were responsible for more than 60% of LOS and coagulase negative staphylococcus was the major culprit. But a study in Iran[17] showed that Enterobacter sp was the predominant organism of both EOS and LOS. Disagreement of bacteriological profile of EOS and LOS in different regions was the essence of a continuous surveillance of the aetiology of neonatal sepsis. Types of organisms isolated in EOS and LOS were more or less similar except Klebsiella sp which was closely associated with EOS (P value=0.043). In the present study, neonatal sepsis was significantly higher in low birth weight and preterm babies (P value 0.027 and 0.00 respectively). But no significant diversity of demographic parameters including birth weight, gestational age, gender, mode of delivery, outcomes, were observed between EOS and LOS except place of delivery. Referred neonates were more prone to develop LOS. This was in concordance with a study in South India,[10] Iran[17] and Nepal.[18] Birth weight served as a differentiating factor for LOS and EOS in a study in South India [10] but that was not prominent in this study. Mortality in EOS was higher than LOS group in Bangladesh[8] and Iran[15] but in present study it was almost same in EOS and LOS. Overall case fatality rate due to sepsis is 16.4% which was found to be quite similar to a studies done in Johannesburg Hospital (20.8%)[12] and Iran (19%).[15] Clinical presentation of EOS and LOS were similar in this study simulating the result of an Iranian study.[17] Refusal to feed was the most common presenting feature followed by respiratory distress, lethargy and hypothermia in our study and studies from Nepal[18] and West Bengal[13] whereas respiratory distress was the chief complaint of the study in Iran.[19] Multivariate regression analysis showed caesarean section was associated with increased morbidity in cases of EOS but no significant differences were seen in morbidity rates based on gender, birth weight, and preterm status. This was comparable to a Study in Tehran.[17] Though Signore C[20] et al showed that caesarean delivery was associated with increased morbidity in neonates, but not associated directly with sepsis. So this might be due to co-morbidity that had occurred after Caesarean delivery. None of the demographic factors was found to be associated with increased risk of LOS. As seen across the rural India [13] and Bangladesh[8],result of this study also revealed that most of the cases of sepsis were caused by multidrug resistant bacteria. Among them, Gram negative bacteria showed high resistance to ampicillin, gentamicin and cephalosporin group of drugs. Emergence of ESBL (9.09%) was a threat to the clinician but it was less than the incidence of ESBL found in a NICU of Iran (44%).[15] In contrast to a study in rural Bengal[6],where more than 80% cases were found to be resistant to amikacin and ciprofloxacin, 50% of GNB were resistant to these drugs in this hospital. Imepenem remains as the only effective drug against these notorious pathogens. Incidence of MRSA was 61.9 %. Similar finding has been reported elsewhere.[15] Vancomycin, teicoplanin and linezolid were recovered as the most effective drugs for gram positive cocci. Similar findings have been reported in previous studies done in eastern India.[14] The high prevalence of multidrug resistant organisms in this study indicates an association of neonatal sepsis with treatment failure, higher morbidity and mortality and increased cost. Limitation of this study was that, we did not consider maternal genital flora or any maternal risk factors which might have a major contribution to the outcome of babies.
CONCLUSION
This study reflected the fact that neonates were suffering from EOS and LOS in this hospital with almost same epidemiological and clinical presentation with very little differences in microbiological profile. Gram negative organisms were predominant isolates of sepsis so, their source is to be searched for and necessity of infection control measures is to be emphasized. Collection of up-to-date data would strengthen local information system, ultimately enabling policy-makers and programme planners to use existing resources more effectively to achieve a better and effective goal to reduce mortality as well as morbidity caused by neonatal sepsis
ACKNOWLEDGEMENTS
We would like to thank the colleagues and staffs of Department of Paediatrics and Microbiology for their help to pursue this work. We want to acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript and also grateful to authors/editors/publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed
References:
REFERENCES
1. Klein Jo. Bacterial Sepsis and Meningitis. In: Remington JS, Klein Jo.eds. Infectious diseases of fetus and newborn and infants. 5 theds. W B Saunders Co. Philadelphia; 2001:943-984.
2. Guha D.K, Saili A. Guha R, Aggarwal A. Common Infections in the Newborn. In: Neonatology – Principles and Practice. Guha D.K; 3rd eds. Jaypee Brothers Medical Publishers (P) Ltd. New Delhi, India; 2005: 654 – 672.
3. Stoll BJ. Infection of the Neonatal Infant. In Nelson’s Text Book of Paediatrics; Behrman RE, Kleigman RM, Jenson HB. 18theds; WB Saunders Co.2006; 794-811.
4. A.K. Zaidi, W.C. Huskins, D. Thaver et al., Hospital acquired neonatal infections in developing countries, Lancet 2005; 365 : 1175–1188.
5. Sundaram V, Kumar P and Narang A. Bacterial profile of early versus late onset neonatal sepsis in a North Indian tertiary care centre: Heading towards a change. Journal of Pediatric Infectious Diseases 2009; (4): 241– 245
6. Clinical and Laboratory Standards Institute. Performance standards for antimicrobial disk susceptibility tests. Approved standard M2- A10. Wayne, PA: Clinical and Laboratory Standards Institute; 2009
7. Shah M. N. and. Desai P. B. Clinical and bacteriological profiles of blood culture positive sepsis in newborns.IntJ. of Pharm. and Life Sci. 2011; 2(9):1041-1045
8. Hafsa A, Fakruddin M, Hakim MA, Sharma JD. Neonatal bacteremia in a neonatal intensive care unit: analysis of causative organisms and antimicrobial susceptibility. Bangladesh Journal of Medical Science 2011; 10 (3) ;187-194
9. Shrestha NJ, Subedi KU, Rai GK. Bacteriological Profi le of Neonatal Sepsis: A Hospital Based Study. J Nepal Paedtr Soc 2011;31(1):1-5.
10. Kuruvilla A K, Pillai S, Jesudason M and Jana A K. Bacterial profile of sepsis in a Neonatal Unit in South India. Indian Pediatrics 1998; 35:851-858
1. Jia-Horng Jiang, Nan-Chang Chiu, Fu-Yang Huang, Hsin-An Kao, Chyong-Hsin Hsu, Han-Yang Hung et al . Neonatal sepsis in the neonatal intensive care unit: characteristics of early versus late onset. J Microbiol Immunol Infect 2004;37:301-306
12. Motara F, Ballot DE, Perovic O. Epidemiology of neonatal sepsis at Johannesburg hospital. The Southern African journal of Epidemiology and Infection 2005;3: 90-93
13. Viswanathan R, Singh Arun K, Ghosh C, Dasgupta S, MukherjeeS,and Basu S. Profile of Neonatal Septicaemia at a District-level Sick Newborn Care Unit. J Health Popul Nutr 2012;30(1):41-48
14. Pal K, Samanta A K. Bacteriological profile and antimicrobial resistance pattern in early onset neonatal sepsis: challenge to the physician. Int J Cur Res Rev 2013; 5 (6):51- 58
15. Yilmaz N O, Agus N, Helvaci M, Kose S, Ozer E, and Sahbudak Z. Change in Pathogens Causing Late-onset Sepsis in Neonatal Intensive Care Unit in Izmir, Turkey. Iranian Journal of Pediatrics 2010; 20 (4): 451-458
16. Joseph CJ, Wee Bin Lian W B, Yeo C L. Nosocomial Infections (Late Onset Sepsis) in the Neonatal Intensive Care Unit (NICU). Proceedings of Singapore Healthcare 2012; 21(4): 238-244
17. Afsharpaiman S,Torkaman M, Saburi A,Farzaampur A, Amirsalari S, Kavehmanesh Z. Trends in incidence of neonatal sepsis and antibiotic susceptibility of causative agents of two neonatal intensive care units in Tehran.I.R. Iran. Journal of Clinical Neonatology. 2012;1(3):124-130.
8. Khinchi Y. R, Kumar A, Yadav S. Profile of Neonatal sepsis. Journal of college of Medical Sciences-Nepal, 2010; 6 (2): 1-6
19. Mosayebi Z, Movahedian AH, Soori T. Clinical and bacteriological chartacteristics of neonatal sepsis in an intensive care unit of Kashan, Iran: A 2 years descriptive study. Arch Pediatr Infect Dis. 2013;1(2):61-64
20. Signore C.Klebanoff M. Neonatal morbidity and mortality after elective caesarean delivery. Clin Perinatol 2008; 35: 361-371
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License