IJCRR - 6(14), July, 2014
Pages: 32-37
Date of Publication: 22-Jul-2014
Print Article
Download XML Download PDF
PREVALENCE OF CRYPTOCOCCAL MENINGITIS AMONGST HIV SEROPOSITIVE CASES FROM A TERTIARY CARE HOSPITAL
Author: Rajani Sharma, Nandini Duggal, Shalini Malhotra, Dinesh Shrivastava, Charoo Hans
Category: Healthcare
Abstract:Background: Cryptococcal meningitis has emerged as an important opportunistic central nervous system (CNS) infection in Human immunodeficiency virus (HIV) positive patients. It is associated with a high mortality rate hence early diagnosis is necessary to improve the prognosis. Objectives: This study was undertaken to determine the prevalence of cryptococcal meningitis in HIV seropositive cases as well as to determine the correlation with CD4 counts. Methods: A total of 50 patients suspected to be suffering from chronic meningitis were subjected to cerebrospinal fluid (CSF) analysis (including India ink preparation, culture by conventional methods and antigen detection). Results: The prevalence of cryptococcal meningitis in this study was 30%. Outcome was fatal in 6/15 cases showing a mortality rate of 40 percent. The patients with CD4 count < 50 cells/ul had highest mortaliy rate i.e. 50%. Conclusion: High prevalence and mortality rate of cryptococcal meningitis in HIV-infected patients require a high index of suspicion and routine mycological surveillance to establish an early diagnosis and appropriate management.
Keywords: Cryptococcus neoformans, HIV, Immunocompromised, Meningitis
Full Text:
INTRODUCTION
Cryptococcal meningitis is an opportunistic fungal infection which is relatively rare in immunocompetent individuals and occurs when host immune status becomes impaired. The predisposing conditions include HIV infection, diabetes, immune-suppressive therapy after solid organ transplantation, hematological malignancies, etc [1]. Cryptococcal meningitis is difficult to diagnose clinically as presenting symptoms are indistinguishable from other causes of subacute and chronic meningitis. It is associated with a high mortality rate, hence early diagnosis is necessary to avoid complications. Since the onset of acquired immunodeficiency syndrome (AIDS) epidemic, cryptococcal meningitis has emerged as an important opportunistic CNS infection in HIV positive patients [2, 3]. According to NACO and UNAIDS estimates [4], 2-3.1 million people were living with HIV infection in India and 33.4 million people worldwide at the end of 2008. It has been found that early diagnosis and appropriate treatment of cryptococcal meningitis can reduce the HIV related morbidity and mortality significantly. The present study was undertaken with a view to find the prevalence of cryptococcal meningitis in HIV seropositive cases. The correlation between CD4 count and the occurrence of cryptococcal meningitis in these cases was also analyzed.
MATERIAL AND METHODS
This study was conducted in the department of Microbiology of P.G.I.M.E.R and associated Dr. Ram Manohar Lohia Hospital, New Delhi between 2010 and 2011. Fifty HIV seropositive patients with clinical suspicion of chronic meningitis were enrolled in the study. CSF samples from these patients were received and processed for diagnosis of suspected cryptococcal meningitis. CSF sample was inoculated on two sets of SDA (Sabouraud’s Dextrose Agar) and they were incubated at 25°C and 37°C, separately, over a period of 4 weeks. All the cultures were examined daily during the first week and twice a week during the next 3 weeks. An India ink preparation of all the CSF samples was made to examine the presence of capsulated budding yeast cells. Latex agglutination on CSF samples was performed by using cryptococcal antigen detection kit (Meridian diagnostics). Further characterization of Cryptococcus isolates was done by various microbiological tests like sugar assimilation and fermentation, growth on Niger seed agar and on Canavanine glycine bromothymol blue agar. CD4 count estimation was done using FACS caliber (Beckton and Dickinson) system.
RESULTS
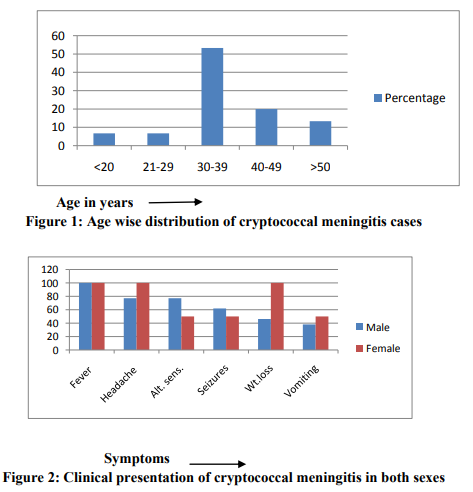
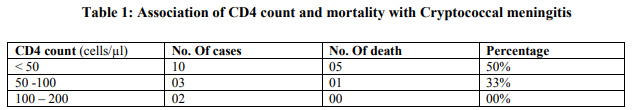
Out of fifty HIV positive patients with clinical suspicion of chronic meningitis, fifteen patients (30% isolation rate) were found to be positive for Cryptococcus. The positivity rate of India ink, culture on SDA and cryptococcal antigen test was found to be 100%. Cryptococcal meningitis was found to be more common in 30-39 yrs. age group with male: female ratio of 13:2. [Figure1] The most common symptom of cryptococcal meningitis was fever which was present in all the patients followed by headache for more than 2 weeks duration seen in 77% of males and in 100% female patients. Altered sensorium was seen in 77% of males and 50% of females while seizures were seen in 62% of males and 50% of females. [Figure 2] Amongst the fifteen patients of Cryptococcal meningitis, CD4 count <50 cells / ul was seen in 10 patients, 3 patients had CD4 counts between 50-100 cells/ul and remaining 2 had CD4 counts between100-200 cells/ul. Outcome was fatal in 6 out of 15 Cryptococcal meningitis cases. Thus, mortality rate was 40%. The patients with CD4 count < 50 cells/ul had highest mortality rate i.e. 50%. [Table 1]
DISCUSSION Cryptococcus is an opportunistic fungal infection and cryptococcal meningitis has become the most common lethal opportunistic fungal infection in people with HIV and AIDS. In these patients, cryptococcal meningitis is usually incurable, and individuals who survive the initial infection are given lifelong antifungal therapy to reduce the likelihood of relapse [2]. In our study cryptococcal meningitis was found in 15 out of 50 patients i.e. in 30% of patients which was higher compared to other studies done in India [5, 6]. The reason being the study was not community based, but rather than an institutional study where high risk cases were present and that too in the late stage of their disease. The India ink stain of CSF from HIV-infected patients in our study was positive for 100%, which is higher than the figure documented in the Western literature [3]. The significantly higher positivity rate of the India ink stains among the HIV seropositive patients reflects the greater fungal load in these patients. In a study [7], CSF
India Ink examination was positive in 96.29% as compared to 85% reported in another one [8],while cryptococcal antigen was found to be positive in all the patients in both these studies which are similar to our observation also. The sensitivity of culture was found to be 100% in our study which is comparable to the above mentioned studies [7, 8]. The age of the patients with cryptococcal meningitis in this study ranged from 19 to 55 years; the male: female ratio being 13:2. This finding is similar to the study by Manoharan et. al. [9], who had observed the highest incidence of cryptococcal infection (16/31) in the 30-40 yrs. age group with male patients predominantly affected (29/31). Common involvement of male gender may reflect a difference of exposure rather than a difference in host susceptibility. Cryptococcal meningitis may have an acute, subacute or chronic presentation in HIV-infected patients, requiring a high index of suspicion. More than 75% of the patients with cryptococcal meningitis in HIV-infected patients had fever, most patients also had headache, but a substantial number may not had these manifestations. In our study, fever (93.33%) was the most common presenting symptom of cryptococcal meningitis in HIV-infected patients, followed by headache (80%), altered sensorium (73.33%) and seizures (60%). In a study by Patel et. al. [7], headache (96.29%) was the single most common presenting symptom followed by vomiting (77.77%) and fever (66.66%). A study from Lucknow [10] showed headache in 39 (89.5%), fever in 34 (78.9%), altered sensorium in 11 (23.7%), neck rigidity in 6 (13.2%), seizure in 4 (10.5%) patients whereas, Lakshmi V et. al. [6], observed headache in 31−92% cases, fever in 49−79% and altered sensorium in 71−79%. The CD4 cell count is the main predictor of an HIV patient's immunologic state. In the present study, the CD4 cell count ranged from 12 to 202 cells/µl. Median CD4 cell count of the whole group was 56 cells/µl. This is in accordance with the observation that cryptococcal meningitis presents in late stage of HIV infection and a major cause of death in HIV-infected patients with CD4 cell count <100 cells/µl [3,6,8,11,12 ]. Untreated cryptococcal meningitis is universally fatal. Studies from African countries have reported a very high mortality (64%) [13], while the morbidity and mortality in HIV patients with cryptococcal meningitis in developed countries is 2.5–15% [14, 15]. In our study the mortality rate was found to be 40% which is quite higher than the other Indian studies [7, 8, 10]. The high result in the present study could be due to it being a hospital based study, where high risk cases were present mostly as referral cases from outside Delhi and also the sample size being small as compared to other studies.
Other opportunistic infections found in the study group: HIV infection is the strongest of all known risk factors for the development of tuberculosis. Adequate cell mediated immunity is the crucial host defence against M. tuberculosis. As HIV infection primarily affects the components of cellmediated immunity, therefore in HIV infected individuals, latent tuberculosis infection get reactivated. Moreover, the infection is poorly contained following reactivation, resulting in widespread dissemination causing extrapulmonary disease. We found that beside cryptococcal meningitis, tuberculosis and oral candidiasis were the most common opportunistic infections in HIV-infected patients. Twenty six percent of these patients had more than one associated illness, and oral candidiasis and tuberculosis were the most frequently encountered combination. This observation is in consonance with two large studies [6, 16] on HIV-infected patients reported from the Indian subcontinent. Laxmi et. al., found that cryptococcal meningitis was associated with pulmonary tuberculosis in 28.21% cases and lesions suggestive of oral candidiasis in 17.9%., whereas Kumarswamy et. al. observed pulmonary tuberculosis in 49.3% and oropharyngeal candidisis in 54.5% cases. Since pulmonary tuberculosis is endemic in India, we frequently see an association of this disease with cryptococcal meningitis, unlike reports from the West, where disease due to Pneumocystis jiroveci is a more frequent coexistent illness [12]. Out of 15 patients suffering from cryptococcal meningitis in the present study, three patients (20%) had concurrent pulmonary tuberculosis, one (7%) had abdominal tuberculosis and six (40%) had lesions suggestive of oral candidiasis. Lakshmi et. al. [6], noted concurrent pulmonary tuberculosis in 28.21% cases and lesions suggestive of oral candidiasis in 17.9%. In a study from South Africa [13], associated illnesses were diagnosed in 80% of the 44 HIV-positive patients. These associated illnesses were, more commonly tuberculosis (32%), generalized lymphadenopathy (46%), and oral thrush (46%). CONCLUSION This study concludes that cryptococcal meningitis should be suspected in all cases of chronic meningitis among HIV infected persons as clinical picture may be confusing with tubercular meningitis. Emphasis should be given on conventional methods of diagnostic approach, which is possible in most of the diagnostic laboratory set up in India. India ink examination is a simple test for resource poor settings in developing countries like India. In view of high prevalence of cryptococcal meningitis in HIV patients, India ink examination should be done in all CSF samples with clinical suspicion of chronic meningitis. Latex agglutination test for cryptococcal antigen and culture are other sensitive and specific tests for the diagnosis of cryptococcal meningitis.
ACKNOWLEDGEMENT
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed. Authors are grateful to IJCRR editorial board members and IJCRR team of reviewers who have helped to bring quality to this manuscript.
References:
1. Clark TA, Hajjeh RA. Recent trends in the epidemiology of invasive mycosis. Curr Opin Infect Dis 2002; 15: 569-74.
2. Bicanic T, Harrison TS. Cryptococcal meningitis. British Medical Bulletin 2005; 72:99-118
3. Casadevall A, Perfect JR: Cryptococcus neoformans. 1st edition. Washington: American Society for Microbiology Press; 1998. 3
4. UNAIDS – AIDS Epidemic Update 2009:www.unaids.org 4
5. Jaiswal SP, Hemwani N, Sharma N, Athale S, Chitnis DS. Prevalence of fungal meningitis, among HIV positive and negative subjects. Indian J Med Sci 2002; 56:325-9. 5
6. Lakshmi V, Sudha T, Teja VD, Umabala P. Prevalence of central nervous system Cryptococcosis in Human Immunodeficiency Virus reactive hospitalized patients. Indian J Med Microbiol 2007; 25:146-9.
7. Patel A.K., Patel KK., Ranjan R., Shah S., Patel J.K. Management of cryptococcal meningitis in HIV infected patients: Experience from western India. Indian J Sex Transm Dis 2010; 31:22-26.
8. Kumar S, Wanchu A, Chakrabarti A, Sharma A, Bambery P, Singh S. Cryptococcal meningitis in HIV infected: Experience from a North Indian tertiary centre. Neurol India 2008; 56:444-49.
9. Manoharan G, Padmavathy BK, Vasanthi S, Gopalte R. Cryptococcal meningitis among HIV-infected patients. Indian J Med Microbiol 2001; 19:157-8.
10. Prasad KN, Agarwal J, Nag VL, Verma AK, Dixit AK, Ayyagiri A. Cryptococcal infection in patients with clinically diagnosed meningitis in a tertiary care centre. Neurol India 2003; 51:364-366.
11. Crowe SM, Carlin JB, Stewart KI, Lucas CR, Hoy JF. Predictive value of CD4 lymphocyte numbers for the development of opportunistic infections and malignancies in HIV-infected persons. J Acquir Immune Defic Syndr 1991; 4:770-6.
12. Powderly WG. Cryptococcal meningitis and AIDS. Clin. Infect. Dis.1993; 17:837–842.
13. Moosa MYS, Coovadia YM. Cryptococcal Meningitis in Durban, South Africa: A Comparison of Clinical Features, Laboratory Findings, and Outcome for Human Immunodeficiency Virus (HIV)-Positive and HIV-Negative Patients. Clinical Infectious Diseases 1997; 24:131-4.
14. Cameron ML, Barlett JA, Gallis HA, Waskin HA. Manifestations of pulmonary cryptococcosis in patients with acquired immunodeficiency syndrome. Rev Infect Dis 1991; 13:64-7.
15. Lipson BK, Freeman WR, Beniz J, et. al. Optic neuropathy associated with cryptococcal arachnoiditis in AIDS patients. Am J Ophthalmol 1989; 107(5):523-7.
16. Kumaraswamy N, Solomon P, Flaningan TP, Hemalatha R, Thyagarajan SP, Mayer KH. Natural history of human immunodeficiency virus disease in southern India. Clin Infect Dis 2003;36:79-85.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License