IJCRR - 6(20), October, 2014
Pages: 21-24
Date of Publication: 20-Oct-2014
Print Article
Download XML Download PDF
TOTAL ANTIOXIDANT ACTIVITY - A BIOMARKER IN ORAL PRECANCER PATIENTS
Author: Chitra Purohit, Suman Jain, Jaspreet Kaur
Category: Healthcare
Abstract:With weakened antioxidant defenses, body cells and tissues become prone to develop dysfunction and/or disease. Then, the maintainance of adequate antioxidant levels, but not overdosage, is essential to prevent or even manage a great number of disease conditions. Total antioxidant activity (TAA) could be a reliable biomarker of diagnosis and prognosis of oral precancerous lesions like oral leukoplakia (OL) and oral submucous fibrosis (OSMF), although several cautions for its use should be carefully done ( choice of appropriate method, use of other antioxidant biomarkers such as cell antioxidants, genetic antioxidant \? response elements or antioxidant vitamins and use of valuable oxidative biomarkers ). TAA could be useful to evaluate nutritional interventions with antioxidant \? rich foods on disease risk and prevention. The present study was thus undertaken and an attempt was made to correlate the serum levels of lipid peroxidation, assessed by thio barbituric acid reactive substances (TBARS) and total antioxidant activity (TAA) in relation to oral precancer lesions. The results of this study indicate that imbalance in the redox status of oral precancer patients may be due to enhanced lipid peroxidation and compromised antioxidant defenses.
Keywords: Oral leukoplakia, Total antioxidant activity, Oral submucous fibrosis, Oxidative stress, Oral precancer
Full Text:
INTRODUCTION
Exceptional advances in biomedical sciences since the past century gives opportunities to understand the molecular basis of disease that could result in new strategies for treatment and prevention of diseases. Today, more than 70 pathologies are intrinsically associated with oxidative stress and its biochemical consequences, like peroxidation of lipids (1) measured by assessing thio barbituric acid reactive substances (TBARS). OSMF is a premalignant (2) and crippling (3) condition of the oral mucosa. Leukoplakia is the most common precancerous lesion of the oral mucosa. Oral cancer is generally preceded by benign lesions or conditions that share the same etiologic factors with oral cancer and exhibit the same site-habit relationships. Individuals with oral precancer such as OSMF and leukoplakia run a 69 times higher risk to develop oral cancer compared to tobacco users who do not have precancer (4). Into the origin of these pathophysiologies, there is a mitochondrial dysfunction and subsequent imbalance between releasing of reactive oxygen and synthesis of defective antioxidant systems, resulting in oxidative stress (5). The total antioxidant activity (TAA) measures the antioxidant capacity of all antioxidants in a biological sample and not just the antioxidant capacity of a single compound. Thus measurement of lipid peroxidation product, TBARS and total antioxidant activity is valuable in oral premalignant diseases to assess oxidative burden because they reflect the bioavailability of antioxidants as well as their increased utilization to scavenge lipid peroxidation products.
MATERIALS AND METHODS
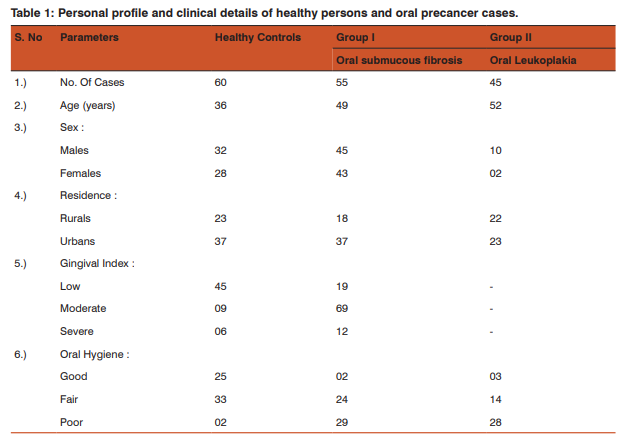
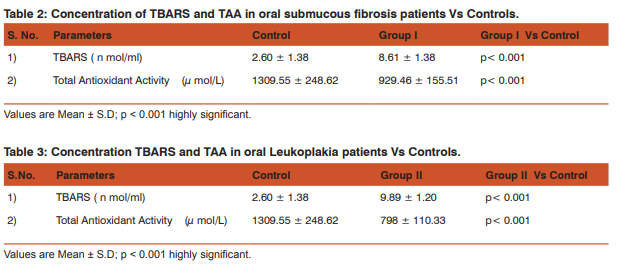
The present study was carried out in department of Biochemistry, Darshan Dental College and Hospital, Udaipur. The ethical committee of Darshan Dental College approved the study. Of the routine OPD patients reporting to department of Oral Medicine and Oral Pathology, Darshan Dental College and Hospital, Udaipur, patients suspicious of OSMF and oral leukoplakia were selected. The relevant history of each patient was recorded. Only those patients who did not have any systemic diseases and/or not received any therapy prior to study were subjected to punch biopsy from buccal mucosa. After confirmation from histopathology, they were included in the OSMF/ oral leukoplakia (OL) group. 60 age and sex matched healthy subjects without any clinically obvious oral le sions or systemic diseases were selected as the control group. The subjects for the study were grouped asGroup 1 (OSMF): 55 patients having oral submucous fibrosis. Group 2 (OL): 45 patients having oral leukoplakia. 5 ml. fasting venous blood was collected from antecubital vein of each individual into plain sterile tube. The sample was then allowed to clot at room temperature and was then centrifuged at 3000 rpm for 10 min. to separate the serum. Immediately this serum was used for estimation of lipid peroxidation as evidenced by the formation of thio barbituric acid reactive substances (TBARS) which was estimated in serum by the method of Buege and Aust, 1978 (6). The pink colored chromogen formed by the reaction of 2-thiobarbituric acid with the breakdown products of lipid peroxidation was read at 535 nm. Total antioxidant activity (TAA) was assessed by the method of Benzie and Strain, 1999 (7) in serum. At low pH, reduction of a ferric tripyridyl-triazine (Fe+3TPTZ) complex to the ferrous form can be monitored by measuring the change in absorption at 593 nm. The reaction is non-specific and therefore the change in absorbance corresponds to the combined or ‘Total’ reducing power of the electron donating antioxidants present in the reaction mixture. The results thus obtained were tabulated and analyzed using student’s unpaired ‘t’ test. RESULTS The personal profiles and clinical parameters of all the subjects under study are shown in Table-1. In the present study, the levels of TBARS and TAA were compared between the control group and OSMF group and also between the control group and OL group. Comparison among control and OSMF group showed a statistically significant increased levels (p < 0.001) of TBARS and decreased levels (p < 0.001) of TAA among OSMF group (Table -2). Similar significant increased levels (p < 0.001) of TBARS and decreased levels (p < 0.001) of TAA among OL group (Table -3).
DISCUSSION
In the present study, mean serum levels of TBARS and TAA were compared between control and OSMF group and between control and OL group. The mean level of TBARS was increased in the OSMF group (Table -2) and OL (Table -3) compared to control . The statistical evaluation by using student’s ‘t’ test , showed that the difference in levels of TBARS between control and OSMF group and also between control and OL group was statistically significant ( p < 0.001 ) . These findings were similar to Gupta et al (8) and Metkari et al (9) who also reported similar significant increase in the lipid peroxidation in OSMF cases as compared to controls. It is established that lipid peroxidation increases with severity of the disease reflecting the extent of tissue injury. The increase in lipid peroxidation product in OSMF and OL as compared to control group may be due to poor antioxidant system, excessive free radical formation due to various tissue abuse habits and decomposition of PUFA present in membrane (9, 10). TAA was found to be significantly decreased in case of oral precancer (both OSMF and OL) patients. Positive correlation between low plasma antioxidant level and tumour burden have been reported by Subapriya et al (10). Functional compromise of antioxidant defense mechanisms has been documented in a wide variety of malignancies (11, 12). Malignant cells may sequester antioxidants from the circulation to supply the demands of a growing tumour (13). The increase in blood lipid peroxides and decrease in TAA seen in oral precancer patients , place these patients in a high – risk category. Thus, determination of TAA and lipid peroxidation may be useful in evaluating oral precancer disease. Further studies on patho-mechanism of ROS-mediated carcinogenesis and implication of protective dietary antioxidants may be beneficial for chemoprevention of oral precancer and thus oral cancer.
SUMMARY AND CONCLUSION :
It is evident from the present study that by estimation of lipid peroxidation and total antioxidant activity in circulation of oral precancer patients, the degree of oxidative damage of the disease can be assessed. Further, TAA evaluation, used with other oxidative stress and antioxidant defense biomarkers, may constitute the first step in search for a healthy oral status. The treatment plan can be improved by correcting the underlying deficiency of antioxidants. It might help for successful management of this condition, thereby arresting it in early stages and avoiding the possible consequences of oral precancer and oral cancer.
ACKNOWLEDGEMENT
Authors sincerely thank Darshan Dental College and Hospital, Udaipur for extending all the facilities for conducting the work. Authors acknowledge the immense help received from the scholars whose articles are cited & included in reference of this manuscript. The authors are also grateful to authors /editors /publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
References:
1. Ferrari CKB. Oxidative stress pathophysiology: Searching for an effective antioxidant protection. Int Med J. 2001; 8:175-184.
2. Pindborg JJ. Oral submucous fibrosis as a precancerous condition. J Dent Res. 1966; 45: 546-53.
3. Dave RP. Oral submucous fibrosis. A clinical and etiological study. J Indian Dent Assoc. 1987; 59: 46-51.
4. Melrose RJ. Premalignant oral mucosal diseases. J Calif Dent Assoc. 2001; 29: 593-600.
5. Kusano C, Ferrari B. Total Antioxidant capacity : a biomarker in biomedical and nutritional studies. J of Cell and Mol Biol. 2008; 7: 1-15.
6. Buege JA, Aust SD. The Thiobarbituric Acid assay methods. Enzymol. 1978; 52: 306.
7. Benzie I, Strain JJ. Ferric reducing/ antioxidant power (FRAP) assay. Methods in enzymology (oxidation stress). 1999; 299: 15-27.
8. Gupta S, Reddy MV, Harinath BC. Role of oxidative stress and antioxidants in aetiopathogenesis and management of oral submucous fibrosis. Ind J Clin Biochem. 2004; 19: 138-141.
9. Metkari SB, Tupkari JV, Barpande SR. An estimation of serum malondialdehyde, superoxide dismutase and vitamin A in oral submucous fibrosis and its clinicopathologic correlation. J oral Maxillofac Pathol. 2007; 11: 23-7.
10. Subapriya R, Kumaraguruparan R, Nagini S. Oxidant-Antioxidant Status in Oral Precancer and Oral Cancer Patients. Toxicology Mechanisms and Methods. 2003; 13: 77-81.
11. Balasenthil S, Sahoo GC, Nagini S. Circulatory lipid peroxidation and antioxidants in pharyngeal cancer patients. J Biochem Mol Biol Biophys 2000; 4: 359-362.
12. Skrzydlewska E, Stakiewicz A, Sulkowska M, Kasacka I. Antioxidant status and lipid peroxidation in colorectal cancer. J Toxicol Environ Health. 2001; 62:213-222.
13. Buzby GP, Mullen JL, Steih TP, Roasto EF. Host tumour interactions and nutrient supply. Cancer. 1980; 45:2940- 2947.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License