IJCRR - 7(3), February, 2015
Pages: 29-31
Print Article
Download XML Download PDF
OSTEOMA CUTIS -A CASE REPORT
Author: C. Nirmala, Lakshmi S., Dayananda S. Biligi, A. R. Raghupathi
Category: Healthcare
Abstract:Case report: We present an interesting case of Osteoma Cutis in a 70 year old women with a large plaque lesion on the scalp and multiple nodules with discharging sinuses in the fingers of both the hands since 30 years.
Discussion: Osteoma Cutis is a rare slow growing, benign ossifying disorder characterized by deposition of bony nodules in the dermis and occurs more frequently in women. There are two types of Osteoma cutis ,Primary and Secondary. Primary Osteoma Cutis is characterized by denovo bone formation in the skin. Secondary Osteoma Cutis is more common, seen in 85% of cases, as a sequel of various disorders. Conclusion: The final diagnosis of Osteoma Cutis cases are based on clinical features, clinical evaluation, phosphorous- calcium metabolism, skin biopsy and radiological imaging.
Keywords: Osteoma cutis, Benign ossifying disorder
Full Text:
INTRODUCTION
Osteoma Cutis is a rare benign ossifying disorder characterized by deposition of bony nodules in the dermis and occurs more frequently in women. In Osteoma Cutis, mesenchymal stem cells differentiate into bone outside the normal skeletal system(4).There are two types of Osteoma Cutis Primary and Secondary. Primary Osteoma Cutis is less common and occurs in 15% of patients and Secondary Osteoma Cutis is common and occurs in 85% of patients(1).
CASE REPORT
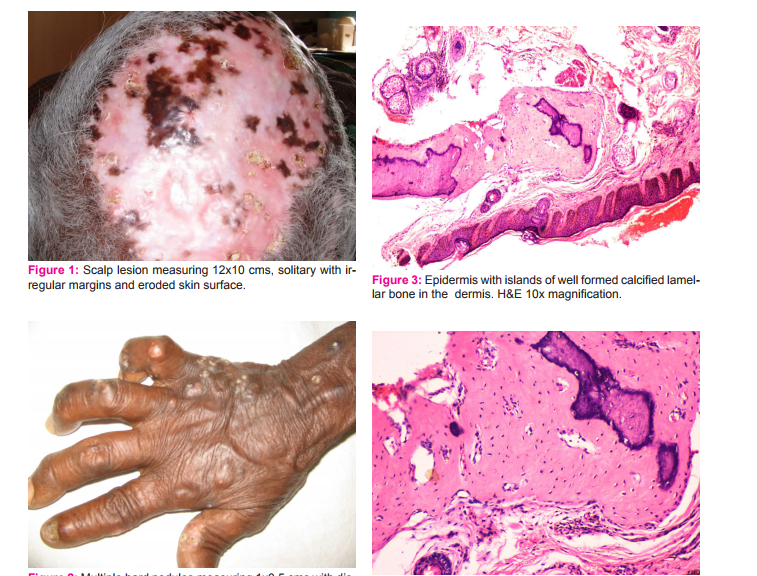
A 70 year old female presented with slow growing plaque like lesions over the scalp and multiple nodules over the hands of 30 years duration. The scalp lesion is seen extending into the frontal region of the face. On examination Scalp lesion measured 12 x 10 cms, solitary with irregular margins (Figure 1). The skin over the surface was eroded, underlying tissue appeared pinkish in colour. On palpation the lesion was bony hard in consistency and fixed to the underling skull bone. Margins showed multiple discharging sinuses and discharging chalky white material. Multiple tiny hard nodules measuring 0.5 – 1cm with discharging sinuses were also seen in fingers of both the hands (Figure 2). Skin biopsy from both the scalp and hand lesions was taken and subjected to histopathological examination. Microscopy on routine Haemotoxylin and Eosin staining showed presence of islands of well formed calcified lamellar bone tissue in the dermis with presence of few osteocytes (Figure 3 & Figure 4). The over lying epidermis appears unremarkable. No other underlying cutaneous pathology was observed. Various investigation of complete blood counts, Serum calcium, phosphorous, electrolytes, Liver and Renal function tests were normal. There was no history of trauma or previous cutaneous lesions. Based on the medical history, clinical and histopathological findings, diagnosis of Primary Osteoma Cutis was confirmed.
DISCUSSION
Osteoma Cutis is characterized by formation of morphologically normal bone within the dermis or in the subcutaneous tissue. In Osteoma Cutis, mesenchymal stem cells differentiate into bone outside the normal skeletal system(4). There are two types of Osteoma Cutis Primary and Secondary. Primary Osteoma Cutis is less common and seen in 15% of patients and secondary Osteoma Cutis is commoner and seen in 85% (1). Histological evaluation of the lesions on skin biopsy show lamellar bone completely calcified and inhabited by osteocytes in the deepest layer of the skin (reticular layer), the area around the nodules are less calcified and presents metaplastic areaof fibroblast to osteoblast which is confirmed on electron microscopy(1). Primary Osteoma Cutis is characterized by denovo bone formation in the skin without a known associated or pre-existing cutaneous disorder . Primary Osteoma Cutis has four different clinical variants – solitary, widespread, plaque like and multiple miliary osteomas of the face(3). Four main syndromes associated with Primary Osteoma Cutis are Albrights hereditary Osteodystrophy, Fibrodysplasia of Progressive Ossification, Osseous Progressive Heteroplasia and Plate like Osteoma Cutis(5). Albright’s Hereditary Osteodystrophy includes features of Pseudohypoparathyroidism , pseudo pseudohypoparathyroidism. Clinical features includes obesity, short stature, brachydactyly, round Facies(4). In the Genetic level, there is heterozygous inactivating germ line mutation of the GNAS gene causing abnormal expression or function of the α-subunit of the stimulatory G-protein adenyl cyclase. This results in reduced inhibitory control of cellular induction to osteoblast differentiation in ectopic sites(4) resulting in heterotrophic ossification originating in fat cells(6). Progressive osseous heteroplasia is characterized by dermal ossification of cutaneous, subcutaneous and deep connective tissues(6). Fibrodysplasia of Progressive Ossification is unique in the mechanism of bone formation is endochondral. The other three entities show more clinical overlap as they all involve intramembranous ossification that begins in dermis(4). Secondary Osteoma Cutis occurs as a sequel to multiple disorders including nevi, scleroderma, pilomatricoma, dermatomyositis, basal cells carcinoma, scars, cutaneous inflammation, trauma, calcification, fibrous proliferation and venous stasis, syringoma ,epidermoid cyst(1). In some cases transepidermal elimination of fragments of bone within the channels lined by epidermis and leading to the surface is seen. The patient in the present study presented with lesion in scalp and fingers of both hands. The most affected areas reported are the scalp, face, chest, breast, extremities and buttocks(7). Lesions do not cause pain or any other symptoms .They arise as single or multiple papules, nodules, plaques or miliary lesions. In a review of literature seven cases of non-congenital forms that had no abnormalities in calcium or phosphate metabolism were detected and no inflammatory conditions preceded the disease(8). Pathogenesis of Osteoma Cutis is still obscure. Some feel Primary Osteoma Cutis may be nevoid and may develop from embryonal nest. Where as in metaplastic osteomas, trauma and inflammation lead to damage of the tissue in course of time, some of the foci damage may become calcified, eventually ossified to masses of bone. Treatment: These patients are treated with topical application of Retinoic acid and surgical excision. Surgical excision was a simple treatment with a quick recovery, minimal scarring and no local recurrence(1).
CONCLUSION
The final diagnosis of these cases are based on clinical features,clinical evaluation,phosphorous –calcium metabolism,skin biopsy and radiological imaging.
ACKNOWLEDGEMENT
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
Source of Funding: Nil
Conflict of Interest: None
References:
1. NA Montecionos Ayariri, FX Nahas, MV Jardini Barbosa, AB Farah, J de Arimatéia Mendes, LM Ferreira. Isolated primary osteoma cutis of the head: Case report. Can J Plast Surg 2006;14(1): 33-36.
2. Osteoma cutis. Indian J Dermatol Venereol Leprol 1996;62:178-9.
3. Sethuraman G, Malhotra AK, Khaitan BK, Kumar R, Sharma VK, Kabra M, et al. Osteoma cutis in pseudohypoparathyroidism. Clin Exp Dermatol 2006;31:225-7.
4. Acquired platelike osteo ma cutis Neelam Vashi MD, Julie Chu MD, Rishi Patel MD, Dermatology online Journal 17 (10):1, 2011.
5. Bowman PH, Lesher JL Jr. Primary multiple military osteoma cutis and exogenous ochronosis Cutis 2001; 68:103.
6. Unilateral progressive osseous heteroplasia Eur J Dermatol 2009; 19 (3): 214-5
7. Boschert MT, Puckett CL. Osteoma cutis of the hand. Plast Reconstr Surg 2000; 105:1017-8.
8. Haro R, et al. Plaque-like osteoma cutis with transepidermal elimination. J Cutan Pathol 2009;36:591.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License