IJCRR - 14(7), April, 2022
Pages: 49-54
Date of Publication: 05-Apr-2022
Print Article
Download XML Download PDF
A Study to Compare the Effect of Conventional Knee Exercises & Macquarie Injury Management Group (Mimg) Protocol on Pain & Functional Mobility in Patients with Primary Osteoarthritis Knee- An Interventional Study
Author: Yashasvi Shukla
Category: Healthcare
Abstract:Introduction: Osteoarthritis is a disorder of the diarthrodial joint, a slow degenerative disease clinically characterized by pain, loss of range of motion. On x-ray seen as reduced joint space, formation of osteophytes and deformity. Manual therapy has been proved to be an effective treatment method in knee osteoarthritis (OA), but there is a need to investigate the effectiveness of MIMG manual therapy technique. There is limited evidence on the effect of MIMG protocol in knee OA. Aim: To find the effectiveness of MIMG protocol on pain and range of motion in knee osteoarthritis. Methodology- 38 subjects with the diagnosis of knee OA stage II and III on Kellegren Lawrence classification were recruited from Shree K.K. Sheth physiotherapy Centre, Rajkot, Gujarat. An interventional study was conducted on 38 subjects. Result: The outcome measures MIMG protocol is effective as conventional exercises in treating OA knee. Conclusion: MIMG can be suggested as one of the treatment protocols.
Keywords: Primary OA knee, Macquarie Injury Management Group Protocol, Pain, Functional mobility, Joint disease, Degradatio
Full Text:
INTRODUCTION
Osteoarthritis (OA) is a degenerative joint disease and the most common form of chronic disorder of synovial joints1 in aging population.2 It is the most frequent joint disease with a prevalence of 22% to 39% in India.2 Knee Osteoarthrosis (OA) is one of the most prevalent musculoskeletal complaints worldwide, affecting 30–40% of the population by the age of 65 years.
Primary osteoarthritis of the knee is associated in 90% of cases with varus deformity. Worldwide estimates indicate that 9.6% of men and 18% of women above 60 years of age have symptomatic OA2but knee involvement is seen equally in both genders from 55-64 years of age.4 The pathophysiology states that osteoarthritic changes are due to an imbalance between the degradation and synthesis process of the articular cartilage.
The most widely used classification scheme for the diagnosis OA is based on the radiological appearance of the joint, which is known as Kellgren and Lawrence classification of Osteoarthritis. Grade I and II according to Kellgren-Lawrence Grading Scale4 or the participants fulfilling the following criteria of the American College of Rheumatology (ACR). (ACR): ACR clinical and radiological criteria: 1) Knee pain for most days of the prior month. 2) Osteophytes at joint margins on X-ray. 3) Synovial fluid typical of osteoarthritis (laboratory). 4) Age 40 years. 5) Morning stiffness 30 min. 6) Crepitus on active joint motion. OA present if items 1, 2 or 1, 3, 5, 6 or 1, 4, 5, 6 are present.3 Radiographs add little to the accuracy of the clinical diagnosis. But in Osteoarthritis of the knee muscle strength and pain are more explanatory of functional loss than radiograph findings.
According to a study done on by Roddy et al.,(2005), aerobic walking and quadriceps strengthening exercises helped patients to decrease pain and improve functional activities. However, there are few studies regarding the effects of exercise on postural stability and balance in OA patients.5
The Macquarie Injury Management Group (MIMG) knee protocol is a new technique in manual therapy developed by Dr. Henry Pollard, a practicing sports clinical scientist based in Sydney. MIMG knee protocol is an approach that includes two techniques myofascial mobilization and myofascial manipulation. It was introduced by the MIMG group, Australia. The techniques involved are the myofascial mobilization technique and myofascial manipulation technique.6
Short-wave diathermy (SWD) is a high-frequency current generated by an oscillator circuit that allows electrons to oscillate at a frequency of 27.12 MHz.7 Pain can be measured for severity on a visual analog scale. It is one of the most basic pain measurement tools. The reliability of VAS is 0.60 to 0.77 and validity is 0.64 to 0.84.8 The WOMAC is a disease-speci?c self-report multidimensional questionnaire assessing pain, stiffness, and physical functional disability. The original WOMAC is available in two formats, visual analog scales (VAS) and ?ve Likert boxes, with similar metric properties.9
MATERIALS AND METHODS
Study design: An interventional study.
Sampling technique: Purposive sampling and group allotment by random sampling
Study setting: K.K Sheth Physiotherapy college.
Sample size: Total 38 subjects (divided into 2 groups).
Study population: males and females with OA knee.
Study duration: 6 sessions per week (two weeks).
Method of data collection:
A total 38 patients were selected for the study by giving consideration to inclusion and exclusion criteria. All the subjects were explained the purpose and the test procedures & written consent was obtained. Ethical clearance was given by the Saurashtra University panel, Rajkot, Gujarat, India.
SELECTION CRITERIA:
Inclusion criteria:
-
age-40 to 70 years of age.5
-
Gender- both males and females.
-
Subjects who are clinically diagnosed with primary OA knee according to American College of Rheumatology (ACR).
Exclusion criteria:-
-
Patients with history of hip and/or back injury and lower-limb joint replacement.
-
Participants who had a joint replacement surgery, history of meniscal or other knee surgery in past 6 months.
-
fractures at knee and hip joint, deformity at lower limb, osteoporosis, neurological deficits, systemic illness & metabolic disorder.
Materials:
Measurement procedure
The A and B group subjects took part in identical pre-and post-test protocols.
Group A: conventional Q-drills and short wave diathermy. (n=15)
Group B: MIMG and short wave diathermy. (n=15)
GROUP A- Conventional knee exercises.
-
Static quadriceps.
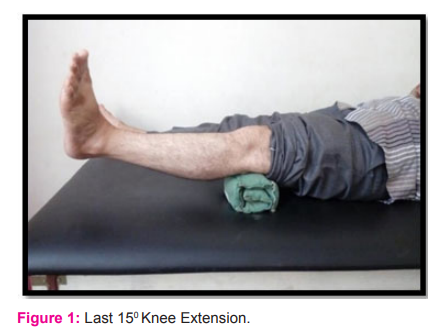
-
last 15 degree knee extension. (figure 1)
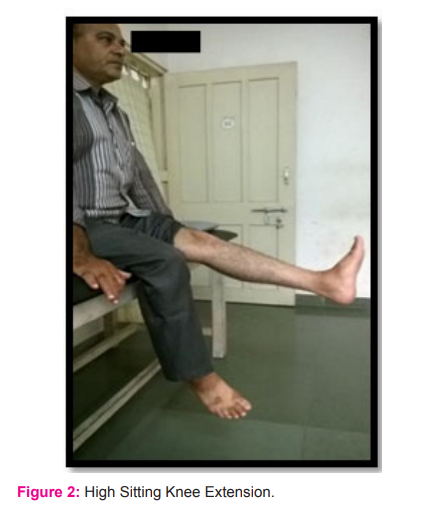
-
high sitting knee extension. (figure 2)
-
unilateral straight leg raising.10
10 repetitions of 5-second hold for each exercise.
GROUP B- MAQUARIE INJURY MANAGEMENT GROUP PROTOCOL (MIMG)6
The intervention group received a MIMG (Macquarie Injury Management Group) chiropractic knee protocol. It consists of a non-invasive myofascial mobilization procedure and an impulse thrust procedure performed on the symptomatic knee of participants. In cases where OA was bilateral; mobilization was performed on both knees.
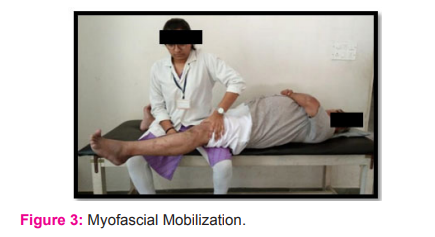
Myofascial mobilization technique: The patient laid supine near the homolateral edge of the couch. The practitioner sat on the homolateral side of the couch with the cephalad thigh under the leg of the patient’s involved limb and superior to the patient’s knee. The patient’s lower hamstring area rested on the practitioner’s thigh with their knee able to rest in 900 of flexion. The practitioner had two choice of contacts:1) a pincer contact with the thumb and index either side of the medial and lateral superior poles of the patella. 2) A reinforced web contact supporting the medial and lateral superior poles of the patella. The second position is recommended for those practitioners who have a hypermobile thumb. The patient was then instructed to begin actively extending their knee through the pain-free range of motion while the practitioner maintained contact at the patella. The force through the patella is in a plane applied at a tangent to the angle of the knee to avoid a compressive load. The patient extended the knee as far as possible in a pain-free manner from the initial starting position. The practitioner maintained contact at the patella during this movement. This was repeated upto 10 times.
Myofascial manipulation technique: the patient laid supine and the therapist stood on the same side of the plinth with the patient’s leg grasped between the thighs to apply a distractive force to produce traction over the tibio-femoral joint. The practitioner contacted the knee with hands either side. Both thumbs contact on the tibial tuberosity and the fingers wrap around the knee to the distal end of the popliteal space. A thrust was then delivered, in the caudal direction in order to mobilize the joint in a near full extension position.
Treatment given in both the groups: Both the groups were given shortwave diathermy for 15min.11
STATISTICAL ANALYSIS
Statistical software:
All statistical analysis was done by SPSS statistics version 20.0 for windows software. Microsoft excel was used to calculate mean and Standard Deviation (SD), and to generate graphs and tables.
Statistical test:
Means and Standard Deviation (SD) were calculated as a measure of central tendency and measure of dispersion respectively. Within-group comparison of WOMAC and VAS value was analyzed by Wilcoxon signed-rank test and between-group comparison of WOMAC and VAS value was analyzed by Wilcoxon sum rank test or Mann-Whitney U test.
Pretreatment and post-treatment data of active knee flexion-extension range of motion and visual analog scale was analyzed by Paired t-test and Wilcoxon signed-rank test respectively and comparison between two groups of active knee flexion-extension range of motion and visual analog scale was analyzed by unpaired t-test and Mann-Whitney U test (Wilcoxon sum rank test).
Level of significance (p-value) was set to 0.05.
RESULT
Thirty eight subjects were randomly divided into two Groups:- Group A conventional Q-Drills treatment (n=19) and Group B MIMG protocol (n=19). Outcome measures WOMAC, ROM and VAS for pain were taken before and after the completion of twelve sessions of treatment (6 times/ week).
The below findings suggest that there is a statistically significant difference for pre-treatment and post-treatment comparison for WOMAC in Group-A (Conventional Q-Drills) and Group-B (MIMG Protocol). There is a statistically significant difference in pre-treatment and post-treatment comparison of VAS in both groups. There is no significant difference for between-group comparisons of WOMAC & VAS. Hence, null hypothesis was accepted and the experimental hypothesis was rejected.
DISCUSSION
In present study, when the values of pre-treatment and post-treatment VAS and WOMAC were analyzed, it was statistically significant in both the groups but when a comparison was done between them, both the techniques were equally effective in reducing pain and improving functional mobility.
Conventional exercise therapy is regarded as the cornerstone of conservative management of the OA knee.2,3 Exercise regimens containing repetitive movements increase the ability of the person’s control over joint movements in all positions. Dynamic stability may help to control abnormal joint translation that occurs during daily movements. This shows as an improvement in WOMAC score.
Knee-extension exercises provide additional vastus medialis obliques (VMO) activity and thus have a greater impact on strengthening the VMO. The VMO functions to control patella alignment by pulling the patella medially during extension and under normal knee function acts as a dynamic medial stabilizer of the patella once the knee reaches terminal extension12 and the final arc of 30 degrees of extension is suggested for strengthening the quadriceps.13
Debra Kushion et al.,(2012)performed a study to compare four common rehabilitation exercises: straight leg raise with neutral and externally rotated hip positions (SLRN, SLRER), and short arc quad with neutral and externally rotated hip positions (SAQN, SAQER) in subjects of PFPS(patellofemoral pain syndrome) for activating the vastus medialis oblique (VMO) and vastus lateralis (VL) and concluded that exercises including short arc quad knee extensions are more effective for both the VMO and VL activation than those incorporating straight leg raises.14 social interaction should have been included as well15 as a part of awareness about the condition and its degeneration. Vandana J. Rathod in 2011 stated that supervised exercises and home based exercises are effective in reducing pain and improving physical function in subjects with osteoarthritis of knee, when given with proper dosage.16
The other objective of this study was to find out the effectiveness of MIMG protocol. Gail Deyle(2000) concluded from their interventional study that a combination of manual therapy and supervised exercise is effective in improving walking distance, decreasing pain, dysfunction and stiffness in patients with OA knee.
The MIMG protocol used for the intervention consisted of a non-invasive myofascial mobilization procedure and an impulsive thrust procedure specific to the patello-femoral articulation. The patient is able to actively articulate through knee flexion and not excessively tighten the quadriceps to cause a vector that compresses the patella onto femur. The mobilization procedure stretches the joint capsule in a sagittal plane, gently mobilizes any restriction to normal movement within the limits of patient tolerance and likely loosens adhesions to the patello-femoral articulation. Together these effects allow the knee greater mobility with less effort, restriction and pain.
The second part of the procedure utilizes a manual therapy procedure that is not under the voluntary control of the patient. It involves the application of longitudinal traction of the tibio-femoral joint in a manner designed to distract the knee and mobilize the joint in a near-full extension position. An impulsive type of thrust directed in a caudal direction is delivered to the knee of the patient. The object of this procedure is not to produce joint cavitation, more so to mobilize the joint. In cases of tibial rotational restriction, the pre manipulative setup could include a rotated tibia as a start point. The thrust component remains the same and is directed purely caudal in direction.
Pollard H and Chiro Grad Dip et al. (2008) studied that the MIMG had benefits in a short term period on self-reported pain and knee function, their study used placebo effect of TENS where intensity was set at zero.
CONCLUSION
The result of the present study showed that patients belonging to both the groups that are conventional knee exercises and MIMG group had relief from pain and other symptoms, increase the activity of daily living and knee-related quality of life. Hence, concluded that both the techniques were effective for osteoarthritis of knee joint. It can be further recommended that both the techniques can be included together in OA treatment regime for better results for patients.
ACKNOWLEDGEMENTS
Author acknowledges extensive support received from the guide Dr. Sheetal Patel, associate professor at Shri K.K.Sheth Physiotherapy College, who thoroughly guided me throughout the research, scholars whose articles are cited and included in the references of this manuscript. The author also shows gratitude to authors/ editors/ publishers of all those articles, journals and books from where the literature for this research work has been reviewed and discussed.
CONFLICT OF INTEREST
There was no conflict of interest.
SOURCE OF FUNDING
Self-funded.
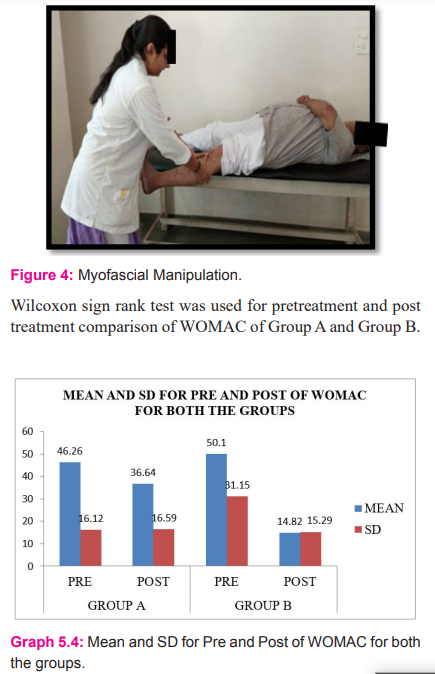
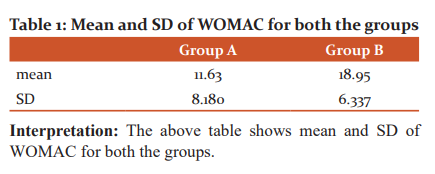
Interpretation: The above table and graph shows mean and SD for group A and group B
Mann Whitney U test was used for between-group comparison of WOMAC of Group A and Group B.
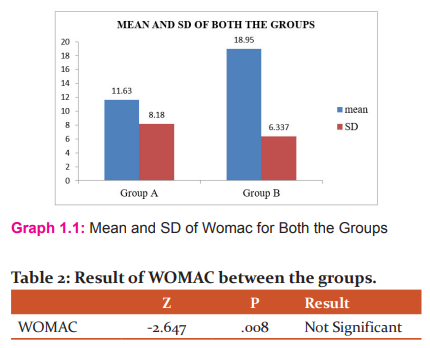
Interpretation: The result shows no significant difference for WOMAC (Z=-2.647, p=0.008).
Wilcoxon sign rank test was used for pre-treatment and post-treatment comparison of VAS of Group A and Group B. Mann Whitney U test was used for between group comparison of VAS of Group A and B.
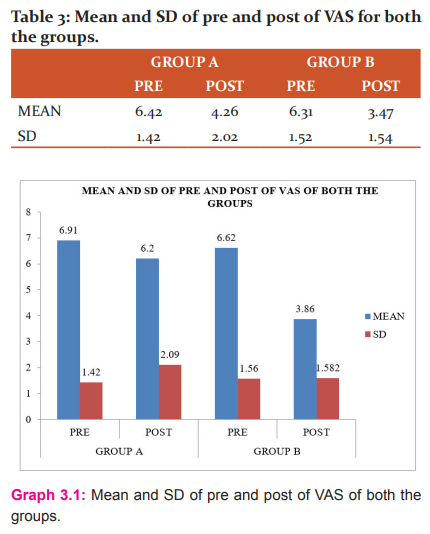
Interpretation: The above table and graph shows mean and SD of VAS of Group A and Group

Interpretation: The above table shows mean and SD of VAS for both groups.
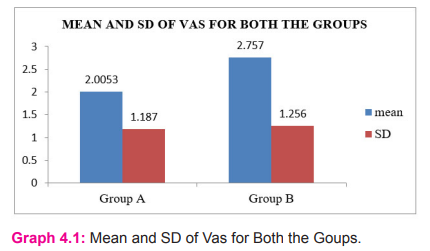
Interpretation: The above table and graph shows mean and SD of VAS for both the groups.

References:
-
Mohan H (2005), textbook of pathology fifth edition. JAYPEE brothers’ medical publishers (p) ltd.
-
Malgaonkar P, Kumar S, Babu V. Short term effect of mulligans mobilization versus kinesiotaping in knee pain and disability for OA knee. Int. J. Physiother. 2014; 1(4);233-240.
-
Essential orthopedics, J Maheshwari 3rd edition; 2011; 278-285.
-
Altman R. Alarcon G. Arthritis and rheumatism;1991;34;505-51
-
Kellgren JH, Lawrence JS. Osteoarthritis and disk degeneration in an urban population. Annals rheumatism;1958;17;388-97.
-
Pollard H. The effect of a manual therapy knee protocol on osteoarthritic knee pain: a randomized controlled trial; J Can Chiropr Assoc;2008;52(4);229-242.
-
Sambajon VV, Cillo JE, Gassner RJ, Buckley MJ, The effects of mechanical strain on synovial fibroblasts, J. Oral Maxillofac. Surg. 61 (2003), pp. 707–712.
-
Melzack R, Wall J, Textbook of pain (4th ed), Churchill Livingstone, Edinburgh (1999).
-
Wright A, Pain-relieving effects of cervical manual therapy. In: R. Grant, Editor, Physical therapy of the cervical and thoracic spine, Churchill-Livingstone, New York (2002), pp. 217–238.
-
Deyle GD, Allison SC, Matekel RL, Physical therapy treatment effectiveness for osteoarthritis of the knee: A randomized comparison of supervised clinical exercise and manual therapy procedures versus a home exercise program. Phys Ther 2005; 85(12):1301–1317.
-
Roddy E, Zhang W, Doherty M.Aerobic walking or strengthening exercise for osteoarthrosis of the knee: A systematic review. Ann Rheum Dis. August 2005;64:544-548.
-
Deyle GD, Henderson NE, Matekel RL. Effectiveness of manual physical therapy and exercise in osteoarthritis of the knee. A randomized, controlled trial. Ann Intern Med2000; 132(3):173–181.
-
Moss P, Sluka K, Wright A. The initial effects of knee joint mobilization on osteoarthritic hyperalgesia. Man Ther 2007; 12: 109–18.
-
Susan OS, Thomas S. Physical rehabilitation. Fifth edition. Philadelphia: FA Davis Company; 2007.
-
Exercise interventions in Knee Osteoarthritis in Aging adults: A Systematic Review of Randomized Clinical Trials Ranveer Kumar Mahato, Int J Cur Res Rev | Vol 11 Issue 23 December 2019
-
Effect of supervised exercise program and home based exercise program in osteoarthritis of knee joint Int J Cur Res Rev www.ijcrr.com Vol. 03 issue 01 Jan 2011
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License