IJCRR - 13(18), September, 2021
Pages: 44-47
Date of Publication: 26-Sep-2021
Print Article
Download XML Download PDF
Giant Renal Angiomyolipoma with Incidental Finding of Serous Cystadenoma - A Rare Case Report
Author: Bhalsod Harsh D, Khan Imran Ali
Category: Healthcare
Abstract:Introduction: Angiomyolipoma (AML) also known as hamartoma is a rare benign tumour composed of an admixture of adipose tissue, smooth muscle and abnormal blood vessels. AMLs of the kidney are seen in 20% of patients with tuberous sclerosis. In an enlarged form, an angiomyolipoma mimics a renal cell carcinoma, therefore it is imperative to rule it out. Surgery management is recommended for confirmatory histological diagnosis and additionally helps by preventing the risk of haemorrhage or malignancy. In our case, we report a 48-year-old female with complaints of lump and pain in the abdomen. Case Report: Contrast-enhanced Computed Tomography (CECT) was suggestive of left renal mass with large cystic lesion over the right ovary. The patient was taken for exploratory laparotomy and a left nephrectomy with right oophorectomy was carried out. On histopathological examination, renal angiomyolipoma with serous cystadenoma of the ovary was seen. Conclusion: Renal angiomyolipoma by itself is a rarity. Therefore, the simultaneous occurrence of a renal AML with serous cystadenoma of the ovary makes us wonder whether this is an isolated incident or a part of a genetic complex yet to be discovered.
Keywords: Renal hamartoma, Renal cell carcinoma, Nephrectomy, Oophorectomy, Exploratory laparotomy, Tuberous sclerosis
Full Text:
INTRODUCTION
Angiomyolipoma (AML) is an uncommon, benign, mesenchymal tumour1which has an incidence of 0.3- 3%.2 Earlier, AMLs were classified under hamartomas, however, they now are listed in the family of perivascular epithelioid cell tumours (PEComas).3 They are composed of adipose tissue cells, smooth muscle cells and abnormal blood vessels in varying proportions.4
AMLs are primarily found in 2 forms; sporadic (80%) and associated with tuberous sclerosis (20%).3 Sporadically occurring AMLs are usually unilateral, unifocal2 and have a preponderance towards women in the 4th- 7th decade of life.1 When associated with tuberous sclerosis, AMLs may be either bilateral or multifocal and tend to occur in a younger age group (3rd decade); hence careful screening is necessary while monitoring for the presence of renal masses.5
Lenk’s triad is formed by the classical symptoms; flank pain (53%), palpable mass (47%) and gross hematuria (23%).2 But most AMLs are small, asymptomatic and are found incidentally from Ultrasonography or CT scans which are performed for other clinical conditions.2 If an AML is more than 4 cm in size it is likely to produce symptoms due to mass effect and therefore requires intervention.3 Other less commonly occurring symptoms include nausea, vomiting, fever, anaemia and blood pressure changes.5
We hereby present a clinical case of a giant renal AML inclusive of investigation and management and an incidental finding of a right serous cystadenoma.
CASE REPORT
A 48-year-old female, with no previous surgical history, got admitted under the Department of General Surgery with complaints of a lump in the abdomen for 2 months along with pain in the abdomen for 10 days. The patient had no complaints of hematuria or weight loss with no family history of malignancy.
On physical examination of the patient, there were 2 masses palpable over the abdomen. One lump measured 20 x 13 cm seen in the umbilical region extending over the hypogastrium, soft, fluctuant with well-defined margins.
Another ballotable lump measuring 15 x 8 cm was palpable over the left lumbar region. Blood profile and urine examination were within normal range. USG abdomen and pelvis was done suggestive of a heterogeneous lesion involving a mid-lower pole with few cystic areas and calcific foci, suggestive of renal neoplasm. Large multiloculated, cystic lesion with thick septation seen arising from right adnexa extending up to lower abdomen s/o right ovarian cyst.
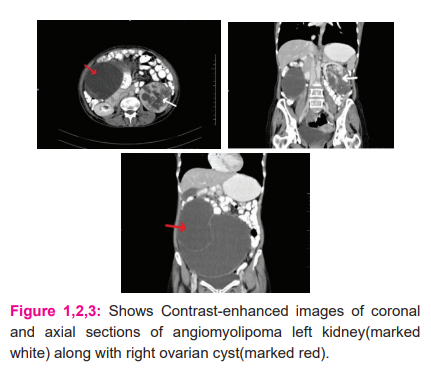
CECT- abdomen & pelvis was s/o well defined exophytic, heterogeneously enhancing soft tissue mass measuring 9.3 x 7.4 x 6.9 cm arising from the mid-lower pole of a left kidney showing central stellate scar with multiple calcifications s/o renal carcinoma along with large multiloculated, multiseptated cystic lesion arising from right adnexa measuring 20.5 x 13.5 x 21.7 cm s/o right ovarian cyst (Fig 1,2 and 3).
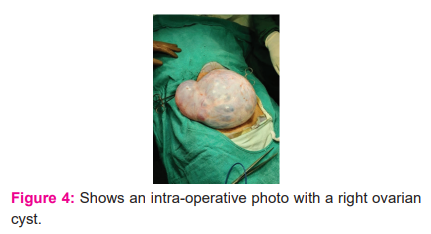
Right oophorectomy and left nephrectomy were carried out and the specimens were sent to the Pathology department (Figure 4,5,6). The post-operative period was uneventful, and the patient was discharged on a postoperative day 10 after complete removal of sutures.
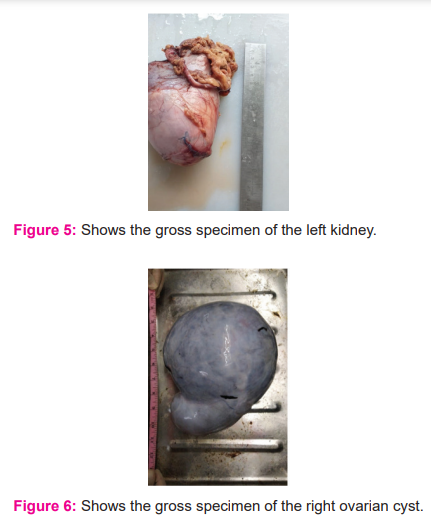
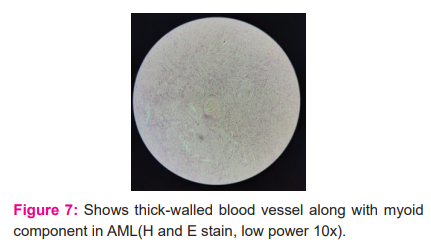
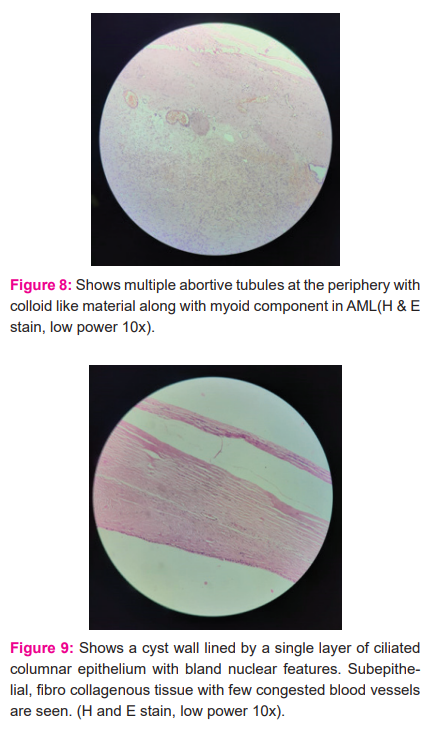
On histopathology, grossly the left kidney measured 13 x 10 x 6 cm with intact hilum with perinephric fat attached. On cut section greyish white area to brownish hemorrhagic area, cystic area, solid variegated to the dark blue area with intact capsule identified. Mass is identified occupying the lower pole extending to the upper 2/3rd of the kidney. The upper pole appears normal. While the right ovarian cyst measured 22 x 18 x 10 cm in size and 50 cm in circumference. On the cut section, it shows a unilocular cyst with a thin wall and blood vessels. No solid areas are identified. On microscopy, AML shows thick-walled blood vessels along with myoid component (Fig 7), multiple abortive tubules at the periphery with colloid-like material along with my myoid component (Fig 8). On microscopy, serous cystadenoma shows a cyst wall lined by a single layer of ciliated columnar epithelium with bland nuclear features. Subepithelial, fibro collagenous tissue with few congested blood vessels are seen (Fig 9).
DISCUSSION
Angiomyolipoma is a rare benign tumour of the kidney.1It was originally described by Fischer in 1911 and was named by Morgan in 1951.6 AMLs are classified under Perivascular Epithelioid Cell Neoplasms (PEComas). PEComas have been defined by the World Health Organization (WHO) as “mesenchymal tumours composed of histologically, ultra-structurally and immunohistochemically distinctive perivascular epithelioid cells”.2 Differential diagnoses of AMLs are subtypes of sarcomas - fibrosarcoma, leiomyosarcoma and renal cell carcinoma.1 Earlier report stated that a renal AML could grow by about 4 cm annually in its maximum diameter. When the diameter of renal AML reaches >10 cm, the tumour is referred to as ‘giant’. Renal AMLs growing to a diameter more than 10 cm, have been termed as ‘giant’. Citations of giant renal AMLS are few to be found, with the largest renal AML (39x25cx9 cm) being reported by Taneja et al.,2013.7
It is of paramount importance to differentiate angiomyolipoma from renal cell carcinoma.8 Renal cell carcinomas and AMLs are both hypervascular lesions that share many radiological findings and may be indistinguishable.8 Hence, radiological investigations are imperative for the diagnosis of AMLs. On USG, AMLs normally display a mass with high or mixed echogenicity. On CT, an AML is shown to be well-circumscribed, with adipose and soft tissue is present in varying proportions.5The presence of fat inside a renal nodule, although not pathognomonic, virtually leads to the diagnosis of AML. CT presents a 95% accuracy rate for diagnosis of AMLs.6
The majority of AMLs are less than 4 cm in size and are not accompanied by any signs or symptoms. Management for these patients is mainly conservative. If required, radiofrequency ablation can also be carried out.7 A half-yearly follow-up CT is required for asymptomatic lesions > 4 cm in size. Symptomatic lesions are usually >8cm in size.5Several reports in the literature suggest that surgical treatment should be used in tumours measuring larger than 4.0 cm.6 In high-risk patients, with lesions more than 4cm, prophylactic embolization is advised, before surgery.5 However, the primary objective of management is always to retain maximal renal function and to prevent haemorrhage.5 It has been observed that as the size of angiomyolipoma increases, symptoms associated with mass effect begin to appear and there is an increased risk of bleeding. Studies indicate that there is a risk of 13% and 51% risk of bleeding if the lesion is < 4 cm or > 4 cm respectively.5 In our case report, the size of the lump measured 12 cm, therefore, classifying it as a “giant” AML. Hence, a left nephrectomy was carried out.
CONCLUSION
The unusual occurrence of two benign neoplasms, renal angiomyolipoma and serous cystadenoma of the ovary has not been reported in the literature. This unique occurrence whether an accidental case or it carries any genetic implication may be discovered in future years.
References:
-
Singh LO, Singh SO, Chongtham C, Maibam C, Singh TS. Renal Angiomyolipoma: A case report, Int J Res Health Sci. 2016; 4(3):73-76.
-
Sarma U, Sangma RA, Deka R. Angiomyolipoma of kidney–a case report. Medico Res Chron. 2015 ;2(3):311-314.
-
Strahan A, King J, McClintock S. Retroperitoneal angiomyolipoma: a case report and review of the literature. Case Reports in Rad. 2013; 2013 : 1-2.
-
Marcuzzi A, Haider EA, Salmi ISA. Hepatic epithelioid angiomyolipoma with renal metastasis: radiologic-pathologic correlation. Radiol Case Rep. 2018;13(4):829–833.
-
Wright T, Sooriakumaran P. Renal angiomyolipoma presenting with massive retroperitoneal haemorrhage due to deranged clotting factors. Case Report. Cases J. 2008 ;1(1):213.
-
Pinto AC, Campos RS, Pereira DA, Gomes GC, Carnevale FC, Pinto AF. Renal angiomyolipoma rupture: case report. Case Reports in Rad. 2006;4(1):25-26.
-
Chen P, Jin L, Yang Y, Chen Z, Ni L, Yang S, Lai Y. Giant renal angiomyolipoma: A case report. Molec Clin Onc. 2017;7(2):298-300.
-
Malone MJ, Johnson PR, Jumper BM, Howard PJ, Hopkins TB, Libertino JA. Renal angiomyolipoma: 6 case reports and literature review. J Urol. 1986 ;135(2):349-353.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License