IJCRR - 13(15), August, 2021
Pages: 127-132
Date of Publication: 10-Aug-2021
Print Article
Download XML Download PDF
Current Trends in Utilization of Antidepressants in a Tertiary Care Teaching Hospital: An Observational Study
Author: Nayak Jyotiranjan, Swain Sarada Prasanna, Das Priti
Category: Healthcare
Abstract:Introduction: Antidepressants are used primarily for managing depression and anxiety disorder. With the advent of a newer class of antidepressants with fewer adverse effects, changes in prescription patterns are expected. Aim: To study the current trends of utilization patterns of antidepressant drugs in a tertiary care teaching hospital of Odisha. Methods: A cross-sectional, observational study done in the Pharmacology Department in collaboration with Mental Health Institute (Centre of Excellence) of Sriram Chandra Bhanja (SCB) Medical College and Hospital, Cuttack from September 2017 to September 2019. The study participants were patients irrespective of age and sex, who were prescribed at least one antidepressant drug. Data was collected by interviewing the patients or attendants in a predesigned case record form and was analyzed using Microsoft Excel and SPSS v.20. Results: The number of patients included in the study was 180; among them, females were 55% and 45% were males. The mean age was 47.5 \? 6.7 years. Eighty-two per cent were outpatients and 18% were inpatients. SSRIs (selective serotonin reuptake inhibitors) were the most common class of antidepressants, among the prescribed drugs followed by SNRIs (serotonin and norepinephrine reuptake inhibitors). The most commonly prescribed antidepressant drug was Sertraline followed by escort�citalopram. Most of the patients (more than half) were receiving antidepressants for non-depressive disorders. Conclusion: SSRIs was the most common class of antidepressant used and Sertraline, Escitalopram were the most common medication prescribed for depressive and non-depressive disorders
Keywords: Depression, Antidepressants, Selective serotonin reuptake inhibitors, Serotonin and norepinephrine reuptake inhibitors, Sertraline, Tricyclic antidepressants
Full Text:
INTRODUCTION:
Depression is a pervasive and impairing illness that affects the body, mood and thoughts.1 More than 300 million people are affected worldwide and it is fourth among the leading causes of disability and premature death.2 According to WHO figures, the total cases of depressive disorders in 2015 in India were over 50 million which was 4.5% of the population in 2015 and the total Years Lived with Disability (YLD) in India was over 10 million years (7.1%).3 In the management of depression, antidepressants like TCAs (tricyclic antidepressants), SSRIs (selective serotonin reuptake inhibitor), SNRIs (serotonin-norepinephrine reuptake inhibitors), MAOIs (monoamine oxidase inhibitors) and various newer agents which collectively can be grouped as atypical antidepressants have been instrumental.4 Historically tricyclic antidepressants were one of the first drugs to become first-line antidepressants.5 With time SSRIs became first-line drugs.5
Due to our gradually increasing understanding of mental health and depression over the years as well as new drug discoveries, many different antidepressants have come to be used. Some of these drugs have stood the test of time and are still in use and some are no more marketed or are not preferred by clinicians.6 Over some time changes in the utilization pattern of these drugs is expected and the understanding of the factors affecting this change is a valuable tool. By studying utilization patterns we can evaluate drug use according to sex, age, social class and any comorbid conditions among other characteristics.
As there is little recent data available in terms of utilization of antidepressant drugs in the local population, the present study was conducted to analyze the current pattern of utilization of antidepressant drugs in a tertiary care teaching hospital of Odisha.
METHODS & MATERIALS:
-
This was a hospital-based, cross-sectional, observational study.
-
The study was conducted in the Department of Pharmacology in collaboration with Mental Health Institute(Centre of Excellence), SCB Medical College and Hospital, Cuttack.
-
A study team was constituted comprising of the principal investigator, study guide and co-guide. The study protocol was designed by the team.
Study Period:
Study Population:
-
All patients receiving antidepressants, both as outpatient or inpatient, in the Mental Health Institute, SCB Medical College and Hospital, Cuttack.
Sample Size:

Where ‘a is the prevalence of antidepressant use and ‘d’ is an allowable error.
Ethical Permission:
-
The Institutional Review Board at S.C.B Medical College, Cuttack gave approved the study with reference letter no. 13351.
-
The study was conducted after getting approval from the institutional ethics committee.
Study Subjects:
Inclusion criteria-
Study Procedure
-
Demographic details of selected subjects like age, sex, educational, marital and employment status are noted in prestructured case record form (CRF). Clinical details like diagnosis, an antidepressant used, dosage, route of administration, frequency and duration of treatment noted in CRF.
Statistical Analysis
-
Results were analyzed using descriptive statistics like mean + SD, percentages and proportions. Significance, when required, was tested using the chi-square test at the two-sided α level at 5%. All the analysis was done by using Microsoft Excel and SPSS v.20.
RESULTS.
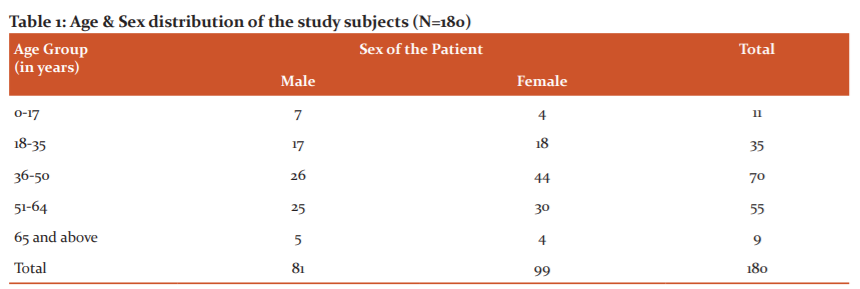
Our study had a total of 180 patients enrolled. Of them majority were females, i.e. 99 (55%) compared to males, i.e. 81(45%). The mean age of the study subjects was 47.5 + 6.7 years. Most of the subjects, i.e. 70 (38.9%) belonged to the age group of 36-50 years, followed by 51-64 years age group with 55 (30.5%). Females were taking antidepressants significantly more than males only in the age group of 36-50 years. (Chi-Square Test, p = 0.03). [Table-1]
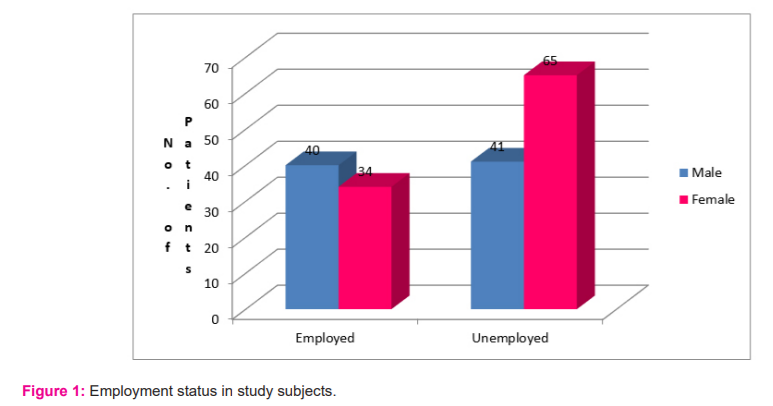
Among the study subjects a significantly higher number of patients, i.e. 106 (58.9%) did not have any employment (Chi-Square Test, p= 0.017). Of the 106 unemployed subjects, 41(39%) were males and 65 (41%) were females. There was no significant effect of unemployment on the rate of antidepressant usage between the genders. (Chi-Square Test, p= 0.19) [Fig.- 1]
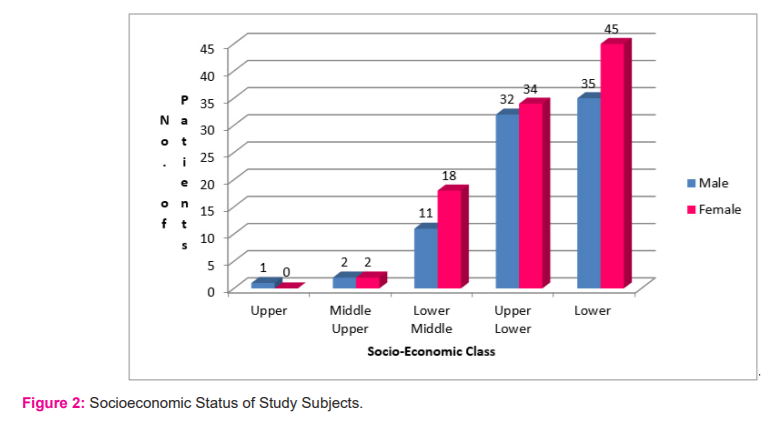
Most of the participants of our study belonged to the ‘Lower’ socioeconomic class in the modified Kuppuswamy Scale, i.e. 80 (44.4%) followed by the ‘Upper Lower’ socioeconomic class with 66 (37.7%). [Figure – 2]
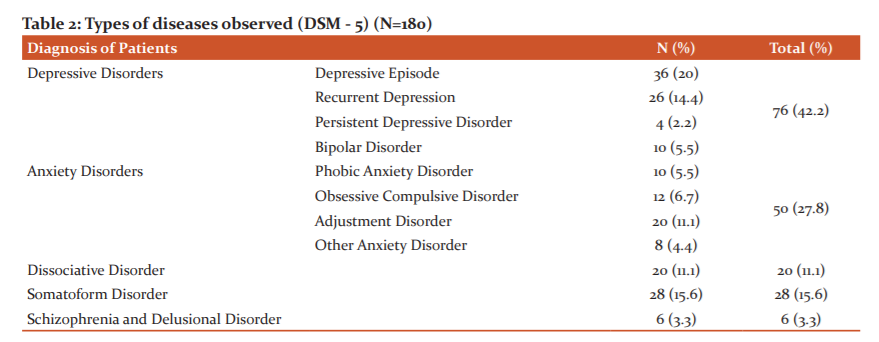
Depressive disorders were the primary reason for taking antidepressants (42%) followed by anxiety disorders with 28%. [Table – 2]
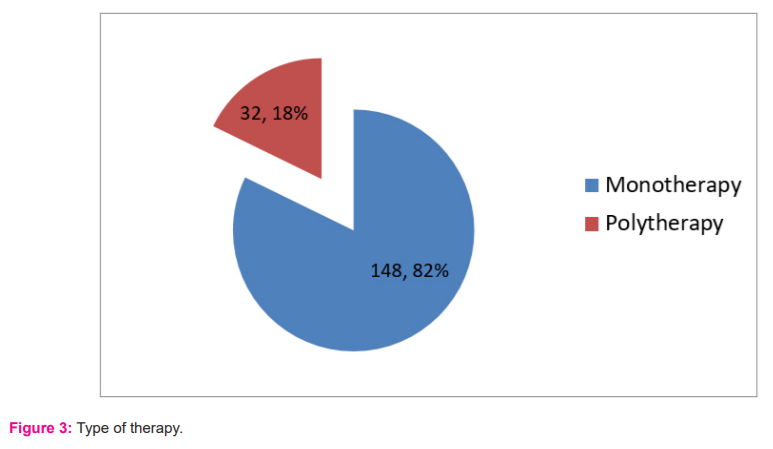
A total of 212 antidepressant prescriptions were given to 180 patients. Monotherapy was practiced to a greater extent, i.e. 148 (82.2%). Polytherapy was seen in 32 (17.8%) patients and comprised of patients receiving two drugs, an SSRI along with a TCA or a newer antidepressant. [Figure – 3]
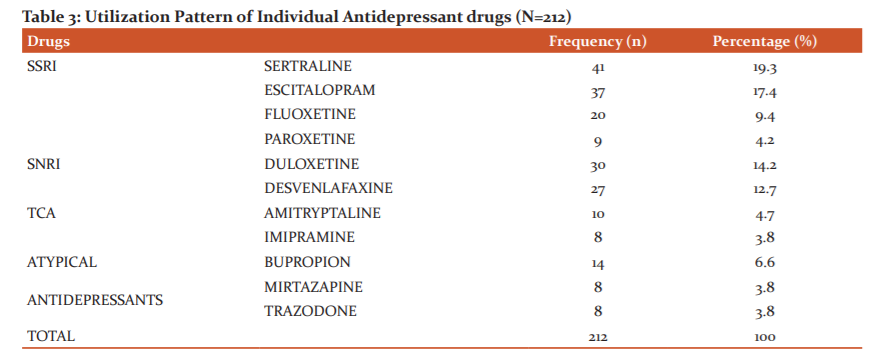
Altogether 107 (50.5%) prescriptions were for SSRIs followed by 57 (27%) for SNRIs. A total of 18 (8.5%) prescriptions contained TCAs and 30 (14%) contained newer atypical antidepressants. Sertraline was the most common drug prescribed (19.3%) followed by Escitalopram (17.4%) and Duloxetine (14.2%). Among the atypical antidepressants, Bupropion with 14 (6.6%) prescriptions was most common. In the combinations, Sertraline plus Bupropion was most common followed by Fluoxetine plus Bupropion. [Table – 3]
DISCUSSION:
The current study is a cross-sectional observational study focusing on the sociodemographic profile of patients receiving antidepressants and the pattern of their utilization. A total of 81 males and 99 females were our study subjects. This slight (1.2:1) female preponderance in antidepressant use is consistent with findings of Ghosh et al (1.2:1), Mukherjee et al (1.3:1) and Mishra et al (1.3:1).6,7,8 However some studies by Avanthi et al (1.9:1), Chattar et al (1.6:1) and Gummadi et al (1.5:1) have found a much higher female preponderance.9,10,11 Some even have found higher male preponderance by Tripathi et al.12
In this study majority of the subjects belonged to the middle-aged group of 36 – 50 years (39%) followed by the 51 – 64 years age group (30.5%). The average age of participants was 47.5 years. Mishra et al have similar findings with the majority of study subjects in 36-50 years age group and 41.7 years of average age.8 However many studies by Ghosh et al, Mukherjee et al, Avanthi et al and Gummadi et al found a lower age group of about 18-40 years taking the most amount of antidepressants with an average age ranging from 35 to 39 years.6,7,9,11
Among our study subjects, almost 59% did not have any employment suggesting a relationship between unemployment and consumption of antidepressants. However, a study by Grover et al finds the rate of unemployment at 23%.13 This drastic difference could be due to demographic differences, as most patients visiting our center come from a semi-urban to rural background compared to the multicentric study by Grover et al involving bigger Indian cities like Delhi, Bengaluru, Chennai, Lucknow, Mumbai, Ahmedabad etc. Based on the modified Kuppuswamy scale of socioeconomic status 44% of our subjects belonged to the ‘Lower’ class and about 38% to the ‘Upper Lower’ class. These findings are in congruence with findings by Van Soest et al which claims higher rates of antidepressant prescription with lower socioeconomic status.14 Only 3% of all subjects belonged to ‘Upper Middle’ and ‘Upper’ class which may not be a true reflection of their antidepressant prescription. This could be due to the factor of affluent people opting to avail treatment in a more private set-up.
Our study suggested that depressive disorders (42%) and anxiety disorders (28%) were the most common diagnoses where antidepressants were used. These results are similar to findings by Mukherjee et al which suggested corresponding numbers of 54% and 26% respectively.7 This study also confirmed that more than half of the patients who were receiving antidepressants had diagnoses other than depression. An earlier international study by Uchida et al reported that 38.4 percent of prescriptions of antidepressants were for patients with diagnoses other than depressive disorders.15
Monotherapy was the most common modality of treatment in our study suggesting that the patients responded well to single drugs. These findings are similar to many Indian studies.7,8,12 This effect could be because using more than one antidepressant drug increases the cost of therapy as well as the chances of drug interactions and side effects resulting in loss of compliance.
SSRIs (51%) were the most commonly prescribed medications among antidepressants in comparison to other groups, a finding similar in all recent studies. Among individual drugs, Sertraline (19%) was the most commonly used drug very closely followed by Escitalopram (17%). In studies by Grover et al, Tripathi et al, Mukherjee et al and Mishra et al Escitalopram is the most commonly used drug.7,8,12,13Among SNRIs Duloxetine was the most prescribed drug and was also the third most prescribed drug overall with 14.2% prescriptions. Desvenlafaxine was the other SNRI with 12.7% prescriptions. Among the atypical antidepressants, Bupropion with 6.6% prescriptions was most common. TCAs were the least used drug class. This is similar to studies by Grover et al, Mishra et al and Tripathi et al8,12,13but in contrast with findings by Mukherjee et al. and Siddiqui et al where TCAs were the second most prescribed drug class after SSRIs.7,16 In the combinations Sertraline plus Bupropion was most common followed by Fluoxetine plus Bupropion. The reason for higher usage of SSRIs and SNRIs compared to TCA could be their better safety profile while having similar efficacy.17
Though 180 prescriptions were studied, it is not sufficient to generalize to a state’s population. Also being done in a tertiary set up this study may not be a proper indicator of the utilization pattern of smaller rural areas.
CONCLUSION:
Among the prescribed antidepressants SSRIs were the most common class of drug followed by SNRIs.Sertraline was the most common drug to be prescribed followed by Escitalopram. More than half of the patients receiving antidepressants suffered from non-depressive disorders. Monotherapy was preferred over combination therapy.
Acknowledgment: Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors/editors/publishers of all those articles, journals, and books from where the literature for this article has been reviewed and discussed
Source of Funding: Nil
Conflict of Interest: None declared.
Authors’ Contribution: Dr. Jyotiranjan Nayak was the principal investigator. He along with the co-authors designed the study. He questioned the participants, reviewed their case record forms and collected all relevant data from the participants. Dr. Sarada Prasanna Swain was the psychiatrist involved in the study. He guided in the clinical aspects of the study. Dr Priti Das is the corresponding author of this study. She provided valuable inputs in the design and conduct of the study.

References:
1. Bromet E, Andrade LH, Hwang I, Sampson NA, Alonso J, de Girolamo G, et al. Cross-national epidemiology of DSM-IV major depressive episode. BMC Med. [Internet]. 2011 Dec 26 [cited 2019 Dec 14];9(1):90.
2. Becker AE, Kleinman A. Mental Health and the Global Agenda. N Engl J Med. [Internet]. 2013 Jul 4 [cited 2019 Dec 12];369(1):66–73.
3. Depression and Other Common Mental Disorders: Global Health Estimates. Geneva: World Health Organization; 2017. Licence: CC BY-NC-SA 3.0 IGO.
4. Kupfer DJ. The pharmacological management of depression. Dialog Clin Neurosci. 2005;7:191–205.
5. Hillhouse TM, Porter JH. A brief history of the development of antidepressant drugs: From monoamines to glutamate. Exp Clin Psychopharmacol. 2015 Feb 1;23(1):1–21.
6. Ghosh S, Roychaudhury S. Prescribing pattern of antidepressant drugs in a tertiary care hospital of eastern India. J Chem Pharm Res. 2014;6(6):2593–7.
7. Sen S, Tripathi S, Chatterjee S, Era N, Ghosal M, Mukherjee S. Adverse drug reaction monitoring of antidepressants in the psychiatry outpatient department at tertiary care teaching hospital in India: A cross-sectional observational study. Eur J Psychol Educ Stud. 2015;2(1):14.
8. Mishra S, Swain T, Mohanty M. Patterns of prescription & efficacy evaluation of Antidepressants in a tertiary care teaching hospital in Eastern India. Asian J Pharm Clin Res. 2012;5(SUPPL. 3):193–6.
9. Avanthi E, Somashekar H, Kumar L, Sushma H, Sudarshan C, Raja B. Prescribing pattern of antidepressants in psychiatric unit of a tertiary care hospital. Int J Basic Clin Pharmacol. 2014;3(4):667.
10. Chattar KB, Karve A V., Subramanyam A, Tondare SB. Prescription pattern analysis of antidepressants in psychiatric outpatient department of tertiary care hospital in India. Asian J Pharm Clin Res. 2016;9(4):77–9.
11. Gummadi T, Harave VS, Aiyar LN, Rajalekshmi SG, Kunnavil R. Adverse drug reaction monitoring in a tertiary care psychiatry setting: A comparative study between inpatients and outpatients. Indian J Psychol Med. 2017;39(3):306–11.
12. Tripathi A, Avasthi A, Desousa A, Bhagabati D, Shah N, Kallivayalil RA, et al. Prescription pattern of antidepressants in five tertiary care psychiatric centres of India. Indian J Med Res. 2016;143(April):507–13.
13. Grover S, Avasth A, Kalita K, Dalal P, Rao G, Chadda R, et al. IPS multicentric study: Antidepressant prescription patterns. Indian J Psychiatry. 2013;55(1):41–5.
14. Von Soest T, Bramness JG, Pedersen W, Wichstrøm L. The relationship between socio-economic status and antidepressant prescription: A longitudinal survey and register study of young adults. Epidem Psych Sci.2012;21:87–95.
15. Uchida N, Chong MY, Tan CH, Nagai H, Tanaka M, Lee MS, et al. International study on the antidepressant prescription pattern at 20 teaching hospitals and major psychiatric institutions in East Asia: Analysis of 1898 cases from China, Japan, Korea, Singapore and Taiwan. Psychiatry Clin Neurosci. 2007 Oct;61(5):522–8.
16. Siddiqui RA, Shende TR. Prescription Pattern of Antidepressant Drugs in a Tertiary Care Centre of Central India. J Contemp Med Dent. 2014;2(2):14–6.
17. Richelson E. Pharmacology of antidepressants. Mayo Clinic Proceedings. 2001;76: 268-279.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License