IJCRR - 13(15), August, 2021
Pages: 41-43
Date of Publication: 10-Aug-2021
Print Article
Download XML Download PDF
Effect of Addition of TiO2 Nanofiller and Intrinsic Pigment on Tear Strength of Cosmesil M511 and VST50F Silicone Elastomers - A Comparative Study
Author: Komal Singh, Sakina Sadiqe Ali, Harsha Hardiya, Ankita Mangal, Shalini Kumar, Palak Agrawal
Category: Healthcare
Abstract:Introduction: There are numerous materials available for creating maxillofacial prostheses. Maxillofacial silicone elastomers are greatly affected by the presence of intrinsic and extrinsic pigmentation Objectives: The study aimed to evaluate the effect of the addition of TiO2 nanofiller and intrinsic pigment on the tear strength of Cosmesil M511 and VST50F silicone elastomers. Materials and Method: It comprised Cosmesil M511 and VST50F silicone elastomers. Each comprised of 20 samples. Each elastomers sample was further classified into 2 equal groups of 10 each. One group had no additives (control), C Heat-temper�nature-vulcanizing HTV for the HTV elastomer and C RTV(room-temperature-vulcanizing) for the RTV silicone elastomers and the second group had nanofillers such as TiO2 and intrinsic pigment (experimental, E HTV for the HTV silicone elastomer and E RTV for the RTV silicone elastomers). In one part, tear strength and in another part Shore, A hardness was tested. Results: The mean tensile strength (kN/m) in C HTV was 11.6\? 0.12, in E HTV was 13.5\? 0.17, in C RTV was 24.4\? 0.13 and in E RTV was 27.6\? 0.16. The difference was significant (P< 0.05). The mean hardness (Shore A unit) in C HTV was 25.2\? 0.13, in E HTV was 28.4\? 0.19, in C RTV was 27.8\? 0.07 and in E RTV was 28.6\? 0.14. The difference was significant (P< 0.05). Conclusion: Authors found that both tear strength and hardness increased with the addition of nanofillers and intrinsic pigment.
Keywords: Elastomer, Nanofillers, Intrinsic pigment
Full Text:
INTRODUCTION
Facial trauma is common nowadays. Sometimes the injury is such that it requires removal of the facial bony part. The occurrence of pathologies such as cysts and tumors is also common.1 Such pathology demands the removal of bony components along with the dead and decayed bone. Silicone elastomers are the material of choice to replace missing facial parts.2 The ideal requirement of material for external facial prosthesis are tear resistance, high tensile strength, ease of molding, color stability, water absorption, non-toxic, and non-sensitivity to the host tissues.3
There are numerous materials available for creating maxillofacial prostheses. Silicone is a widely used material and is chemically polydimethylsiloxane (PDMS).4 These are of two types such as room-temperature-vulcanizing (RTV) silicone and heat-temperature-vulcanizing (HTV) silicone based on the vulcanizing process used. High temperature vulcanizing (HTV) silicones are relatively tougher, stronger, and stiffer than RTV materials. There are two major types of RTV silicones such as addition and condensation silicones.5
Maxillofacial silicone elastomers are greatly affected by the presence of intrinsic and extrinsic pigmentation.6 This pigmentation helps in making teeth identical to human tissue. Opacifiers such as CeO2, TiO2, and ZnO (nano-oxides) make maxillofacial prostheses durable and improve their mechanical properties.7 Rai et al. in their study revealed that the addition of intrinsic pigment leads to improved tear strength in Cosmesil M 511 silicone and Biomed silicone. The present study aimed at assessing the effect of the addition of TiO2 nanofiller and intrinsic pigment on tear strength of Cosmesil M511 and VST50F silicone elastomers.8
MATERIALS & METHODS
This study was done in department of Prosthodontics. It comprised of Cosmesil M511 and VST50F silicone elastomers.
Each comprised of 20 samples. Each elastomers sample was further classified into 2 equal groups of 10 each. One group had no additives (control, C HTV for the HTV elastomer and C RTV for the RTV silicone elastomers and second group had nanofillers such as TiO2 and intrinsic pigment (experimental, E HTV for the HTV silicone elastomer and E RTV for the RTV silicone elastomers). In one part, tear strength and in another part Shore, A hardness was tested.
A metal mold for the HTV elastomer and an acrylic mold for the RTV elastomer was produced. In the type C sample in each group tear strength with the universal testing machine was measured based on the formula, tear strength = F/D, where F is force (kilonewtons) and D is the average thickness (meters). The Shore A hardness value was measured with a digital durometer at 4 different areas of the sample. The mean was taken as the final reading. Data were analyzed statistically using Two-way ANOVA and Tukey test. P-value below 0.05 was considered significant.
RESULTS
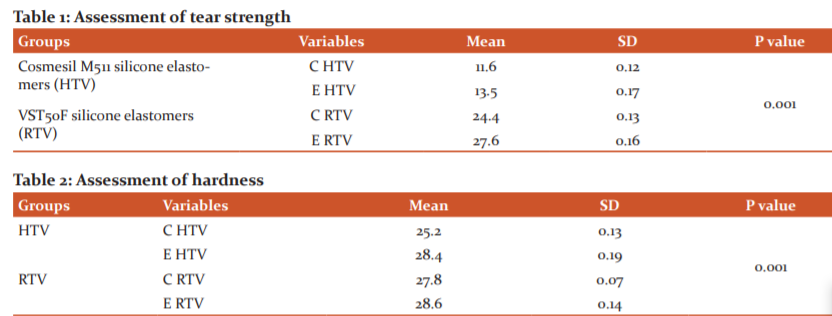
Table 1, shows that mean tensile strength (kN/m) in C HTV was 11.6± 0.12, in E HTV was 13.5± 0.17, in C RTV was 24.4± 0.13 and in E RTV was 27.6± 0.16. The difference was significant (P< 0.05). Table 2, shows that mean hardness (Shore A unit) in C HTV was 25.2± 0.13, in E HTV was 28.4± 0.19, in C RTV was 27.8± 0.07 and in E RTV was 28.6± 0.14. The difference was significant (P< 0.05).
DISCUSSION
Maxillofacial prosthetic materials are used to substitute facial parts that vanished during disease or trauma.9 Facial defects require artificial maxillofacial prostheses. Silicone rubbers are the materials of choice. The average lifetime of such prostheses is 1.5–2 years.10 It shows fine and thin boundaries that bind with the surrounding facial structures. Moreover, it has got high tear strength. Polyzois et al. suggested that a high percentage elongation and high tear strength produce the most desirable combination.11 The present study aimed at assessing the effect of the addition of TiO2 nanofiller and intrinsic pigment on tear strength of Cosmesil M511 and VST50F silicone elastomers.
In the present study, we compared room-temperature-vulcanizing (RTV) silicone and heat-temperature-vulcanizing (HTV) silicone. It is comprised of Cosmesil M511 and VST50F silicone elastomers. Abdul-Ameer compared tear strength and hardness of Cosmesil M511 and VST50F silicone and found significant differences in tear strength among all tested groups. The tear strength of the study subgroups suggestively raised in comparison to the control subgroups (P < 0.05). A non-significant difference in Shore A hardness between the experimental subgroups of both materials was found whereas all tested groups showed significant difference. 12
It is suggested that the percentages and type of thermal initiator, the additives, the fillers, the temperature required for curing, and the time required for polymerization may affect the hardness between the two elastomers. There is a hydrogen bond between a chain of PDMS and surface hydroxyl groups, resulting in an increase in polymer density and producing a stronger and stiffer material. In the present study, we observed that Cosmesil M511 silicone elastomers (HTV) exhibited low tensile strength as compared to VST50F silicone elastomers (RTV). This may be due to the variation in time of curing leading to the differences in polymerization and cross-linking. We found that subgroup C HTV exhibited lower hardness as compared to subgroup C RTV. This may be due to less density of the polymer and hardness because of the low degree of polymerization and cross-linking of Cosmesil M511 silicone elastomers.
Begum et al. compared tear strength, tensile strength, percentage elongation, hardness, and water absorption of Cosmesil, Cosmesil high compliance, and Prestige elastomers. Results demonstrated that there was significantly higher tear strength of osmosis high compliance as compared to other materials and tensile strength was also higher than the other materials but not statistically significant. For all the materials, the hardness and percentage elongation were exactly similar.13 Prestige elastomer though exhibited higher water absorption than the other two materials, but it was not statistically significant.
Shakir and Abdul-Ameer assessed the outcome of adding titanium oxide (TiO2) nanofillers on the tensile strength, tear strength, hardness, and elongation percentage of high-temperature-vulcanized (HTV), room-temperature-vulcanized (RTV) VST50F, and Cosmesil M511 maxillofacial silicone elastomers. They established that VST50F and Cosmesil M511 maxillofacial silicone material's mechanical properties were enhanced with the addition of nano-TiO2 concentration. 14
Addition of intrinsic silicone liquid suspension pigment may also contribute to the increase in tear strength and hardness of the elastomers because the pigments may fully interfere with the matrix of the silicone elastomer.15
Mousa et al. evaluated the effect of hot and dry weather on the surface roughness and hardness of 4 dissimilar maxillofacial silicone elastomeric materials (MFSEM) and found the least hard MFSEM with Cosmesil M-511. A-2000 showed the hardest material and become smoother in weather followed by A-2186. 16
The shortcoming of this study is the small sample size. Only two elastomers were compared. The inclusion of different elastomers could have given different results.
Conclusion
The authors found that both tear strength and hardness increased with the addition of nanofillers and intrinsic pigment.
Conflict of interest: Nil
Source of funding: self
Authors contribution
Singh K – Data collection
Sadiqe Ali S- Analysis
Hardiya H- Investigation
Mangal A- Manuscript writing
Kumar S- Analysis
Agrawal P- Editing
References:
-
Mitra A, Choudhary S, Garg H, Jagadeesh H G. Maxillofacial prosthetic materials – An inclination towards silicones. J Clin Diagn Res. 2014;8: 8-13.
-
Assaad HI, Hou Y, Zhou L, Carroll RJ, Wu G. Rapid publication-ready MS-word tables for two-way ANOVA. Springerplus. 2015;4:33.
-
Pesqueira AA, Goiato MC, dos Santos DM, Haddad MF, Ribeiro Pdo P, Coelho Sinhoreti MA, et al. Effect of disinfection and accelerated aging on color stability of colorless and pigmented facial silicone. J Prosthodont. 2011;20:305-309.
-
Sun L, Gibson R, Gordaninejad F, Suhr J. Energy absorption capability of nanocomposites: A review. Compos Sci Technol. 2009;69:2392-2409.
-
Guiotti AM, Goiato MC, Dos Santos DM, Vechiato-Filho AJ, Cunha BG, Paulini MB, et al. Comparison of conventional and plant-extract disinfectant solutions on the hardness and color stability of a maxillofacial elastomer after artificial aging. J Prosthet Dent. 2016;115:501-508.
-
Wypych G. Plasticizers Use and Selection for Specific Polymers. Toronto, Canada: Chem Tec Publishing; 2004.
-
Hu X. Analyses of Effects of Pigments on Maxillofacial Prosthetic Material. PhD Thesis. The Ohio State University; 2010
-
Rai SY, Guttal SS. Effect of intrinsic pigmentation on the tear strength and water sorption of two commercially available silicone elastomers. J Indian Prosthodont Soc. 2013;13:30-35.
-
Chi YH. Effect of Silica Filler on the Mechanical Properties of Silicone Maxillofacial Prosthesis. MSc Thesis, Indiana University School of Dentistry, Indianapolis (MI); 2014.
-
Abdullah HA, Abdul-Ameer FM. Evaluation of some mechanical properties of new silicone material for maxillofacial prostheses after addition of intrinsic pigments. Saudi Dent J. 2018;30:330-336.
-
Polyzois GL. Mechanical properties of two new addition-vulcanizing silicone prosthetic elastomers. Int J Prosthodont. 1999; 12: 359- 362.
-
Abdul-Ameer FM. Impact of a mixture of nanofiller and intrinsic pigment on tear strength and hardness of two types of maxillofacial silicone elastomers. Dent Res J. 2020;17:251-257.
-
Lewis DH, Castleberry DJ. An assessment of recent advances in external maxillofacial materials. J Prosthet Dent. 1980;43:426-432.
-
Begum Z, Kola Mohammed Zaheer, Joshi P. Analysis of the properties of commercially available silicone elastomers for maxillofacial prostheses Int J Contr Del. 2011; 2(4): 1-5.
-
Shakir DA, Abdul-Ameer FM. Effect of nano-titanium oxide addition on some mechanical properties of silicone elastomers for maxillofacial prostheses. J Taibah Univ Med Sci. 2018 Apr 3;13(3):281-290.
-
Han Y, Zhao Y, Xie C. Color stability of pigmented maxillofacial silicone elastomer: Effects of nano-oxides as opacifiers. Journal of dentistry. 2010; 38(2):e100-105.
-
Mousa MA. Influence of Weather on Hardness and Surface Roughness of Maxillofacial Elastomeric Materials. J Contemp Dent Pract 2020;21(6):678–682.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License