IJCRR - 7(23), December, 2015
Pages: 40-46
Date of Publication: 10-Dec-2015
Print Article
Download XML Download PDF
PREVALENCE OF CONDOM USE AND ASSOCIATED FACTORS AMONG FEMALE SEX WORKERS IN KARACHI, PAKISTAN
Author: Atif M., Khalil R., GulS, Bilal B.
Category: Healthcare
Abstract:As they have multiple sex partners, female sex workers are at a higher risk of sexually transmitted infections, including human immunodeficiency virus. Consistent and correct use of male condoms can reduce this risk. However, condom use among female sex workers is a complicated issue. Objectives: The purpose of this study was to determine the revalence of condom use and to evaluate the factors associated with its use among female sex workers in Karachi, Pakistan. Methodology: A mixed method study was conducted in Karachi, Pakistan. Quantitative data were collected from 200 female sex workers (FSWs) through a structured questionnaire, while Qualitative methods comprised40 in-depth interviews of every 5th female sex worker participating in the cross sectional survey, and Focus-group discussions. The information on socio-demographic characteristics, prevalence of condom use, factors associated with use of condoms, knowledge and awareness about STIs and HIV/AIDS was gathered. The data were analyzed using SPSS 18 and frequencies with percentages were calculated for all qualitative variables. Results: Average age of the participants was 27.9 \? 6.5 years. More than one third had no formal education with 85% reporting a monthly income of more than 8000 PKR[Mean; 16615 \? 10867 PKR]. Nearly half (52%) had spent 4 or fewer years in sex work. The average number of clients per day was 3 \? 1.5 per sex worker. FSWs attached to a brothel were 6 times more likely to use acondom in comparison with street based FSWs. Whereas, FSWs aged younger than 35 years were 2.7 times more likely to use a condom in comparison to older FSWs. Factors found to be associated with not using a condom included being in the sex work for more than 05 years, having sex with non-paying partners, alcohol use, non-availability of condoms, not being associated with a service delivery program and lack of knowledge that condoms can protect against HIV. Conclusion: The study revealed that the prevalence of condom use among female sex workers was low. FSW's lack of negotiating power for condom use was a major reason for its non-use. Other factors associated with not using condoms included not being attached to a brothel, being over 35 years old, more than 05 years in sex work, having sex with nonpaying partners, use of alcohol, unavailability of condoms, no exposure to a service delivery program and no knowledge about condom being protective against HIV.
Keywords: Condom use, Female sex workers, Commercial sex workers
Full Text:
INTRODUCTION
Sexually transmitted diseases (STDs), including HIV/AIDS, are a major public health problem.1 Globally, there were about 36.9 million people living with HIV at the end of 2014. 2 Young women aged 15 to 24 years are 1.6 times more likely to be living with HIV/AIDS than young men. 3 Among them, female sex workers (FSWs), being a high-risk group, bear a disproportionately large burden of HIV infection worldwide.1 Research data shows that when used consistently and correctly, male condoms protect both partners from STDs, including HIV.4,5Condom effectiveness for STD and HIV prevention has been demonstrated by both laboratory and epidemiologic studies.6,7 Evidence of condom effectiveness is also based on theoretical and empirical data regarding STD transmission, the physical properties of condoms, and the protection provided by condoms.8,9,10,11,12 It has been estimated that condoms have prevented around 50 million new HIV infections since the onset of the epidemic. 13 The control of sexually transmitted diseases, including HIV, among sex workers and their clients in urban areas in developing countries, is considered a valuable and cost-effective intervention to reduce the spread of HIV. 14High risk populations include female sex workers as they have multiple sex partners and engage in unsafe sex. However, condom use among female commercial sex workers is a complicated issue. Experiences from research conducted with FSWs have reported that the choice of using a condom is dependent on several socio-economic, personal and work related factors associated with the sex worker.15These factors can act as a barrier to condom use and lead to unsafe sexual practices among sex workers putting them, their clients and the population at large at a risk of getting infected, especially with HIV, which can lead to significantly higher rates of HIV infection within a country.15 Pakistan, like many other countries in South Asia, has a well-developed commercial sex industry, which is illegal, highly complex and involves a large number of people in a variety of sites. 16Pakistan’s sex industry is very poorly documented and operates largely underground because it is illegal. 17Majority of studies conducted in Pakistan, together with anecdotal evidence are suggestive that the sex industry has and is moving out of traditional sites and concentrations in red light areas and becoming dispersed throughout cities, increasingly operating in private houses where they may use mobile phones or have managers and/or pimps who act as clearly defined authorities and as intermediaries between the sex worker and client. 15,16,17 To effectively address the HIV/AIDS epidemic among sex workers and their clients a multi-faceted approach is required. With HIV/AIDS beginning to change its course from a “low-prevalence epidemic” to “concentrated epidemic” in Pakistan, FSWs form one of the core groups which could play a major role in spreading the virus among the high risk groups as well as to the general population. In 2011, the HIV prevalence was estimated to be 0.63%among FSWs in Pakistan. 16This is, at best, a very conservative figure as it is difficult to accurately measure the size of the sex industry in Pakistan because of its hidden nature and wide geographic distribution of FSWs.15However, it is important to explore the unsafe sexual behaviors in high risk groups such as FSWs to inform policy and programs for STI/HIV prevention. Thus, the purpose of this study was to determine the prevalence of condom use and the factors associated with its use among female sex workers in Karachi, Pakistan.
SUBJECTS AND METHODS
A mixed method approach incorporating both a cross sectional survey followed by qualitative techniques were used among female sex workers during March 2015 to June 2015 in Gulshan-e-Iqbal town, Karachi, Pakistan. A WHO sample size calculation softwarewas used to calculate the required sample size. A minimum sample size of 200 was required while taking 5% bound on error of estimation, 95% confidence level, and assuming 50% prevalence of condom use among sex workers. 100 street based and 100 brothel based female sex workers were selected conveniently through a chain referral process and interviewed for the study. For qualitative assessment, in-depth interviews and focus group discussions were conducted with every 5th FSW who participated in the cross sectional survey. Principal Investigator herself conducted face-to-face interviews and data was recorded on a pre-coded questionnaire. A total of 40 in-depth interviews were conducted and each interview lasted about 60 to 90 minutes. All the questionnaires were field edited after each interview to check for legibility, missing fields and any illogical responses. SPSS version 18 was used to analyze the data. In order to identify any type of errors during data entry, 5% of the fields were randomly checked against the physical questionnaires. Mean with standard deviation was calculated for age (in years) while frequency with percentages was calculated for qualitative scale variables such as factors associated with use/non-use of condoms, and knowledge and awareness about STIs and HIV/AIDS. The “use of a condom at the last sexual intercourse” was the dependent variable for the study. Focus Group Discussions Focus Group Discussions with ‘hard to reach’ population of female sex workers and their managers is a very valuable technique to obtain insightful and complex information. A total of three focus group discussions were held. Groups comprised six to eight participants, ideal group range being six. A semi-structured, open-ended focus group guideline/ questionnaire was developed for conducting the sessions. All focus groups followed the same discussion guide that allowed comparisons between various responses of the different groups. The guideline contained eight open-ended questions, designed to discuss effusively during time period of two hours with each group. However, the respondents were allowed to converse for more time, till it was considered appropriate and constructive for generating data. The notes were taken in the local language, in order to retain the literal sense of the responses. The notes were later expanded, immediately after the focus group concluded.
ETHICAL CONSIDERATIONS
Informed verbal consent was obtained prior to the interview. Participation was voluntary and no coercion was used in the data collection process. They were fully informed of the nature of the study and the use of the data. They were free to withdraw from the interview at any time or refuse to answer any particular question. Participants were also ensured of confidentiality. No personal identifying information was obtained for any part of the investigation. Participants were offered information and referral to health and social services available in the community.
RESULTS
A total of 200 sex workers comprising 100 street based and 100 brothel based female sex workers(FSWs) participated in the cross-sectional survey. 144 (72%)FSWs interviewed were full time female sex workers(FSWs), while 56 (28%) reported that they were involved in sex work on a part time basis. Average age of the participants was 27.9 ± 6.5 years. Nearly half (99) 49.5% of the female sex workers(FSWs) were less than 25 years of age. 85% of the female sex workers(FSWs) had a monthly income of more than Rs.8000 income [Mean; 16615 ± 10867 PKR per month]. Prevalence of condom use was defined as the use of a condom on the last sexual intercourse. Based on this definition, 116 (58%) female sex workers(FSWs)had not used a condom, while 84 (42%) reported condom use during the last sexual intercourse. 172 of 200 (86%) respondents had heard about HIV/AIDS. 78% of the respondents knew that HIV is transmitted through sex and 56% knew that condoms can prevent its transmission. (see Chart 1) More than half (104) 52% of the female sex workers(FSWs) were into this profession since less than 5 years, whereas (54) 27% had 5 to 8 years of experience. About 55% of the female sex workers(FSWs) reported 30 or more clients in the last one month. 62% of the female sex workers(FSWs) got clients without involvement of a pimp, whereas 44% said they had to share the money with either a pimp or an auntie. Female sex workers(FSWs) attached to a brothel were 6 times more likely to use a condom in comparison with street based female sex workers(FSWs). Almost 85% participants had their last sexual intercourse with a paying customer. About 42% used alcohol during their last sex encounter. Duration of last sex was up to an hour in (152) 76% subjects, 36 (18%) spent 2 to 3 hours, while 12 (6%) of the respondents reported that they were paid for a full night.
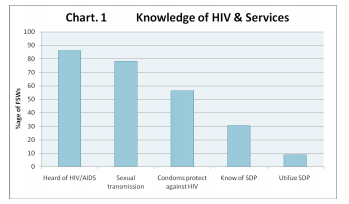
Regarding service delivery programs, 31% respondents had heard about some services provided for sex workers and 10% of them had utilized these services at least once (see Chart 1) 90%of the female sex workers(FSWs) who were using condoms reported that they could easily access condoms, whereas only 33% of the non-users had access to condoms. While about 44% of the non-users felt no need to use a condom. The in-depth interviews and focus-group discussions correlated various factors associated with condom use among female sex workers. As a proxy to determine the negotiating power of the study subjects, they were asked if they could convince clients for the use of a condom. The responses were categorized into three themes; • They could easily convince clients to use condoms, • They had some difficulty in convincing clients to use condoms • They were unable to convince their clients for using a condom, 27% of the female sex workers(FSWs) reported that they were unable to convince the client to use a condom. Despite availability of condoms, the in-depth interviews revealed various reasons for not using them. The main reason for not buying condoms was that the female sex workers(FSWs) did not feel safe while carrying condoms on their person. Some expressed the fear of being stigmatized or harassed if found buying or carrying condoms. Table 1 lists the consequences of insisting condom use on the FSW’s part, the most common being the fear that the client would get angry. 35% of the participants considered that the female sex workers(FSWs) had no say in deciding whether to use a condom or not.
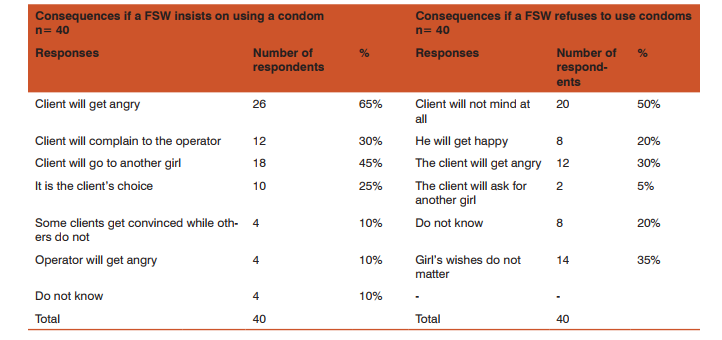
Table 2 lists the various reasons associated with the FSW agreeing or not agreeing to use a condom. Majority of the FSWs wanted to use a condom to avoid pregnancy, while the most common reason to refuse condom use was the fear that it causes allergy and pain.
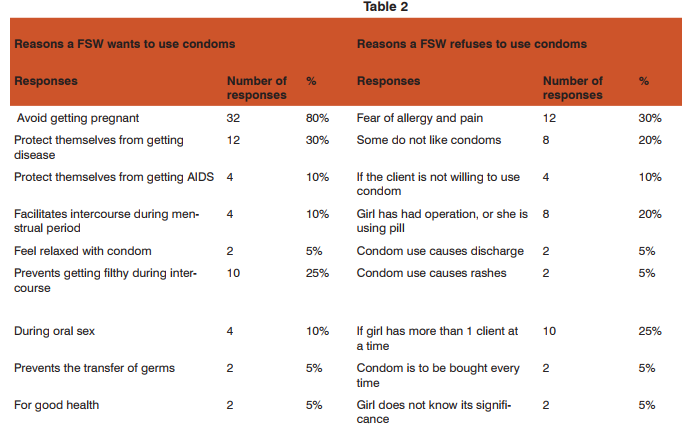
DISCUSSION This study aimed to assess the prevalence of condom use among FSWs and factors associated with its use. Less than half (42%)of the participating FSW reported using a condom during their last sexual intercourse. This was despite the fact that a majority of them were aware of HIV transmission through sexual route. Studies from Uganda18 and Ethiopia19 have also found that despite high levels of knowledge about using condoms as protection against HIV, consistent condom use among FSWs was low. Another study from Indonesia reported that only 12% FSWs reported using a condom although 78% knew the benefits of using one. 20It seems that just having knowledge did not always translate into safe sexual behavior. The study participants were of a unanimous opinion that all girls in commercial sex work knew about condoms and had used them at some occasion during sex work. However, only one third of the participants had heard of health service delivery programs and a mere 10% had actually ever used such services. Sex workers comprise a highly stigmatized and marginalized group in our society, 16 which makes them highly vulnerable to HIV infection by decreasing their likelihood of accessing and participating in any health or social services for STD and HIV prevention. Therefore, FSWs may not be able to take advantage of health services even where they are available. A study in India has reported that exposure to an HIV intervention for FSWs resulted in a higher prevalence of condom use. 21Another study from Pakistan 16 also found that exposure to service programs was associated with increased prevalence of condom use. FSWs reported that condoms were easily available, but they expressed fear of being stigmatized if someone caught them buying or carrying condoms. Especially if a policeman checked their bag it could mean either an arrest or losing a share of their income. Moreover, most of them also feared that their families might find out about their profession if condoms were found in their possession. Thus even though availability of condoms was not a problem per se, purchasing them and carrying them was. Although a fair proportion of the respondents knew that condoms protect them from contracting any disease from their clients, this did not appear to be a major reason for condom use. The main reason quoted for using a condom was to avoid pregnancy. The consistency of condom use also decreased as the number of clients increased. Studies in Ethiopia 19, India22, and Cambodia23have also reported that as the number of clients for a FSW increased the odds of using a condom decreased. FSWs’ lack of negotiation power was found to be a major factor that discouraged condom use with clients. The common theme for not pushing for condom use was the fear of losing a client lest the client got angry or opted for another girl. About half of the participants believed that the FSW did not have any say in deciding whether to use a condom or not. Even where the FSWs tried to negotiate condom use, the final decision was made by the client. This shows that knowledge alone cannot ensure practice unless these workers are empowered to negotiate with clients. Even when the FSW had a condom available, failure to negotiate its use with a client meant unsafe sex. A study in China 24also reported that FSWs lacked the ability to negotiate condom use with their clients and the authors advocated that services and programs should also be directed towards the community at large in addition to specific programs for the sex workers.24Studies from Congo25, Nepal 26, and Nigeria27 have also reported that FSWs’ lack of ability to negotiate condom use with their clients was a major reason for unsafe sex. Research is needed to explore factors that impact FSW’s ability to negotiate condom use, and interventions must be designed to address these factors. The present study showed an association of condom use with age and number of years spent in sex work. Older and more experienced FSWs were less likely to use condoms. The reason may be that they are less open to change and continue with the same practice that they have been following for a long time. Association of condom use with age and duration of work have also been reported by other studies. 18, 19, 25Moreover, FSW who perceived condoms to be protective against STD/HIV were more likely to use them. It is very important to create awareness of STD and HIV/AIDS transmission among the sex workers and the general population, as the clients of the sex workers act as the bridging population in transmitting STI/HIV. The fact that girls working through brothels were more likely to use condoms in comparison to those operating through streets is an important finding. Previous studies have reported that brothel based FSWs are more likely to use condoms probably because the brothels provide the condoms28 thus sparing the FSW the embarrassment of buying them, and they seem to have better negotiating skills as compared to street based FSWs.29 Any interventions must be tailored to address the particular category of the FSWs, therefore, contextual factors need to be researched further. Research has shown that FSWs are more likely to use condoms with their commercial partners/clients in contrast to their regular partners.21,26In the present study the prevalence of condom use decreased with non-paying partners or the girls’ boyfriends and husbands. Studies have found that familiarity and closeness with the male partner decreased condom use 21,26,27 thus putting them at risk of acquiring STI/HIV. Interventions need to target the regular partners of FSWs as well as their paying clients.
FSWs informed that condom use was difficult with clients who were drunk. So the girls did not use condoms when the clients were too intoxicated or under the influence of alcohol. Studies have reported that FSWs find it difficult to negotiate condom use where a client has been drinking 30or under the influence of drugs. 25 The present study did find that FSWs with access to condoms were more likely to use them as compared to those with no access. This means that access to condoms needs to be increased to encourage more consistent use. A study in Congo has also reported that access is an important factor in determining condom use. 25
CONCLUSION
The prevalence of condom use among female sex workers was low despite a high percentage having knowledge about condom use as a protective measure against HIV and STDs. Major barriers to consistent use of condoms included lack of negotiating power of the FSWs and limited access to health and social programs. Other factors associated with not using condoms included, not being attached to a brothel, being over 35 years old, more than 05 years in sex work, having sex with nonpaying partners, use of alcohol, low access to condoms, and no knowledge about condom being protective against HIV. There is a need to improve FSW’s access to health services and counseling regarding safe sex. Interventions also need to target the clients of sex workers and the general population.
LIMITATIONS
There are limitations to this study. Since FSWs are a hard to reach group so non-probability convenient sampling was used for recruitment. The study only included two categories of FSWs, brothel based and street based; therefore, it may not be generalizable to all categories of FSWs.
ACKNOWLEDGEMENT
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
SOURSE OF FUNDING
There is no source of funding for this manuscript.
CONFLICT OF INTEREST
We have no pecuniary or other personal interest, direct or indirect, in any matter that raises or may raise a conflict with our duties as researchers.
References:
1. Shannon, K, Strathdee, SA, Goldenberg, SM et al. Global epidemiology of HIV among female sex workers: influence of structural determinants. Lancet. 2014.
2. WHO. HIV/AIDS. Factsheet No. 360. 2015. Available at: http://www.who.int/mediacentre/factsheets/fs360/ en/
3. Women and HIV/AIDS: Confronting the Crisis. Geneva, Switzerland and New York, NY: Joint United Nations Programme on HIV/AIDS, United Nations Population Fund, and United Nations Development Fund for Women; 2004.
4. UNAIDS. The public health approach to STD control. UNAIDS Best Practice Collection. Technical Update. May, 1998.
5. Richard A. Crosby et al. Associations Between Sexually Transmitted Disease Diagnosis and Subsequent Sexual Risk and Sexually Transmitted Disease Incidence Among Adolescents. Sexually Transmitted Diseases , Vol. 31, No. 4, p.205–208. April 2004.
6. Fitch J Thomas et al. Condom Effectiveness: Factors That Influence Risk Reduction. Sexually Transmitted Diseases, Vol. 29. No. 12, p.811-817. December 2002.
7. Pinkerton SD. Abramson PR. Effectiveness of condoms in preventing HIV transmission. Social Science and Medicine. 44(9):1303-12, 1997 May.
8. Holmes KK, Levine R, Weaver M. Effectiveness of condoms in preventing sexually transmitted infections. Bull World Health Organ 2004;82:454-461.
9. CDC (2006). Sexually Transmitted Diseases Treatment Guidelines, 2006. Morbidity and Mortality Weekly Report, 55(RR-11).
10. Steiner, Cates, and Warner (1999). The real problem with male condoms is non-use. Sex Transm Dis, 26(8): 459-62.
11. Warner, Stone, Macaluso, Buehler, and Austin (2006). Condom use and risk of gonorrhea and Chlamydia: A systematic review of design and measurement factors assessed in epidemiologic studies. Sex Transm Dis, 33(1): 36-51.
12. Weller and Davis (2001). Condom effectiveness in reducing heterosexual HIV transmission. Cochrane Database Syst Rev; 3:CD003255.
13. UNFPA, WHO and UNAIDS: Position statement on condoms and the prevention of HIV, other sexually transmitted infections and unintended pregnancy. 2015; Available at: http://www.unaids.org/en/resources/presscentre/featurestories/2015/july/20150702_condoms_prevention
14. M Laga, M Alary, F Behets, J Goeman, Prof P Piot,N Nzila, A.T Manoka, M Tuliza, M St Louis, Condom promotion, sexually transmitted diseases treatment, and declining incidence of HIV-1 infection in female Zairian sex workers, Volume 344, No. 8917, p246–248, 23 July 1994. Retrieved from: http://www.thelancet. com/journals/lancet/article/PIIS0140-6736(94)93005-8/abstract
15. Emmanuel F, Thompson LH, Athar U, et al. The organization, operational dynamics and structure of female sex work in Pakistan. Sex Transm Infect. 2013;89(Suppl 2):ii29–ii33.
16. Mishra, S, Thompson, LH, Sonia, A, Khalid, N, Emmanuel, F, and Blanchard, JF. Sexual behaviour, structural vulnerabilities and HIV prevalence among female sex workers in Pakistan. Sex Transm Infect. 2013; 89: ii34–ii42.
17. WHO. STI/HIV.Sex work inAsia. 2001; Available at: http:// www.who.int/hiv/topics/vct/sw_toolkit/sex_work_asia.pdf
18. Matovu JKB, Ssebadduka BN. Knowledge, Attitudes and Barriers to Condom Use among Female Sex Workers and Truck Drivers in Uganda: a Mixed-Methods Study. Afr Health Sci. 2013;13(4):1027–1033.
19. Masresha Molla Tamene, Gizachew Assefa Tessema, Getahun Kebede Beyera. Condom utilization and sexual behavior of female sex workers in Northwest Ethiopia: a cross-sectional study. The Pan African Medical Journal. 2015;21:50.
20. Family Health International (2001). What drives HIV in Asia? A summary of trends in sexual and drug-taking behaviours. Arlington: Family Health International.
21. Deering, KN, Boily, MC, Lowndes, CM et al. A dose-response relationship between exposure to a large-scale HIV preventive intervention and consistent condom use with different sexual partners of female sex workers in southern India. BMC Public Health. 2011; 11: S8
22. Hemalatha R, Kumar RH, Venkaiah K, Srinivasan K, Brahmam G. Prevalence of and knowledge, attitude and practices towards HIV and sexually transmitted infections (STIs) among female sex workers (FSWs) in Andhra Pradesh. The Indian journal of medical research. 2011;134(4):470.
23. Bui TC, Markham CM, Tran LT, Beasley RP, Ross MW. Condom negotiation and use among female sex workers in PhnomPenh, Cambodia. AIDS and behavior. 2013;17(2):612-622.
24. Jie W, Xiaolan Z, Ciyong L, Moyer E, Hui W, Lingyao H, et al. (2012) A Qualitative Exploration of Barriers to Condom Use among Female Sex Workers in China. PLoS ONE 7(10): e46786. doi:10.1371/journal.pone.0046786
25. Kayembe PK, Mapatano MA, Busangu AF, et al. Determinants of consistent condom use among female commercial sex workers in the Democratic Republic of Congo: implications for interventions. Sex Transm Infect 2008;84:202–6.
26. Ghimire L, Smith WC, van Teijlingen ER, Dahal R, Luitel NP (2011) Reasons for non- use of condoms and self- efficacy among female sex workers: a qualitative study in Nepal. BMC Womens Health 26 11: 42.doi: 10.1186/1472-6874-11-42.
27. Pattern of condom use and perceived risk of HIV infection among female sex workers in selected Brothels in Ogun State, Nigeria Adeneye A.K.1, Adeneye A.A.2, Mafe M.A.1, Adeiga A.A.3 Int. J. Public Health Epidemiol. 2013; Vol 2(5); pp. 090- 100.
28. Larios SE, Lozada R, Semple SJ, Roesch S, Orozovich P, Fraga M, et al. An exploration of contextual factors that influence HIV risk in female sex workers in México: the Social Ecological Model applied to HIV risk behaviors. AIDS care. 2009;21(10):1335– 1342.
29. Alam N, Chowdhury ME, Mridha MK, Ahmed A, Reichenbach LJ, et al. (2013) Factors associated with condom use negotiation by female sex workers in Bangladesh. Int J STD AIDS 24:813.
30. Nemoto T, Iwamoto M, Colby D, et al. HIV-related risk behaviors among female sex workers in Ho Chi Minh City, Vietnam. AIDS Educ Prev. 2008;20:435–453.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License