IJCRR - 13(12), June, 2021
Pages: 139-146
Date of Publication: 22-Jun-2021
Print Article
Download XML Download PDF
Effectiveness of Obesity-Related Lifestyle Intervention Strategies Among School-Going Adolescents in Selected Schools of Bhubaneswar: A Quasi-Experimental Study
Author: Kundu A, Patnaik L, Sahu T
Category: Healthcare
Abstract:Introduction: Obesity has become a major epidemic causing serious public health concern especially in developing countries. The proportion of children and adolescents in the general population who are overweight and obese has doubled over the past two decades in developed and developing countries including India. Interventions in school are an important strategy to prevent obesity among them. Objectives: To find out the changes in anthropometric parameters and practices following lifestyle interventions related to obesity among school-going adolescents. Methods: A quasi-experimental study conducted from June 2016 to August 2018, in two private schools. A total of 173 students, 86 from the control school and 87 from the intervention school were included. Study participants were interviewed using a pre-designed, pretested and semi-structured interview schedule at baseline and after an intervention. Control school students were given printed educational materials in the form of a carefully prepared poster and intervention school students were intervened for one year by interactive sessions with an integrated educational package, personal and parental counselling for overweight/ obese students followed by reinforcement. Results: No significant difference was seen in anthropometric measurements among the control and intervention group at baseline. In the intervention group, a significant decrease was observed in body mass index (BMI) (P=0.000), the proportion of overweight and obese students (P=0.012), students with elevated BP(P=0.008). A significant increase in physical activity was found among the intervention group in doing regular physical exercise (P=0.004). Conclusion: This school-based intervention program on a healthy lifestyle significantly decrease BMI, blood pressure and improve eating habits, physical activity among adolescents.
Keywords: Overweight, Pediatric obesity, Teens, Body Mass Index, Schoolchildren
Full Text:
INTRODUCTION
Obesity has become a major epidemic causing serious public health concern and the researchers estimated that elevated body weight contributed to 7 per cent of the deaths from any cause in 2015. The number of overweight or obese infants and young children increased from 32 million globally in 1990 to 41 million in 2016. In developing countries, the vast majority of overweight or obese children live in, where the rate of increase was more than 30% higher than that of developed countries (WHO). The proportion of children in the general population who are overweight and obese has doubled over the past two decades in developed and developing countries including India.1,2
Overweight in early childhood has been shown to track to adulthood in one-third to one-half of cases and, where it becomes associated with an increased prevalence of chronic diseases such as type 2 diabetes, cardiovascular disease (CVD), hypertension and polycystic ovarian syndrome (PCOS) later in life.3,4,5 By the year 2035, it is estimated that the prevalence of coronary heart disease will increase by 5% to 16%, with more than one lac excess cases, attributable to increased obesity among today’s adolescents. It is predicted that pediatric obesity may shorten life expectancy by 2 to 5 years by mid-century in the United States.6 It is observed that 30% of obesity begins in childhood and out of that 50-80% become obese adults. 7
Therefore, effective school-based interventions to reduce overweight and obesity in the adolescent age group is needed. For overweight and obesity, factors like consumption of energy-dense foods, low levels of physical activity, sedentary lifestyle play a major role. So, diet and energy expenditure – these two components are the cornerstones of prevention and treatment programs of obesity. Healthy lifestyle approaches to treat younger children with obesity can successfully decrease body mass index (BMI) and implementation of these approaches among adolescents and adults is much effective.8
To address the overweight and obesity problems among children and adolescents, interventions in school is an important strategy. There are no school-based intervention studies to address adolescent obesity in this part of India. With this background, an interventional study was planned to find out the effects of lifestyle interventions among school-going adolescents, as such type of study has not been conducted in this region so far. So this study was conducted to find out the changes in anthropometric parameters and to study the changes in practices following lifestyle interventions related to obesity among school-going adolescents
MATERIALS AND METHODS
This study was a quasi-experimental study conducted over two years and four months from June 2016 to August 2018, carried out in two private schools of Bhubaneswar. All students of two randomly selected section, one from class VIII and one from class IX were constituted the study population. A total of 173 students, 86 from the the control school and 87 from the intervention school were included. Due care was taken to include the absentees.
Study tool: The study subjects were interviewed using a predesigned, pretested and semi-structured interview schedule. Data regarding socio-demographic profile and information about their lifestyle, family history of obesity, type and duration of physical activity, dietary/eating habit, the habit of watching TV or computer etc. were obtained. Data collection including all anthropometric measurements and blood pressure measurement was done by the investigator himself.
Data collection: The prospect of the study for improvement of health and nutrition of students and prevention of complications of obesity was explained to the participants. In 1st phase of the study, baseline data of every student have been recorded. The collection of data was done in a friendly atmosphere after obtaining informed consent from parents and assent from students.
Intervention: The schools were allocated to control school and intervention school. Control school students were given printed educational materials in the form of a carefully prepared poster. Intervention school students were intervened by an integrated educational package which included intense lifestyle education using audiovisual presentations, poster and practical demonstration.
The package included materials on nutrition and lifestyle modification for obesity management. Before giving intervention to the students, the package was shared with the principal of the school and class teacher of concerned sections. The intervention was done by arranging interactive sessions with students in their respective classes, personal counselling for overweight/obese students regarding healthy lifestyle and counselling of parents of overweight/obese students during the parent-teacher meeting as well as over the telephone.
During the interactive sessions, a healthy discussion has been done by power-point presentations, videos. To improve their physical activity, yoga classes in the group were arranged during their physical education period. In the initial two months of the intervention, one interactive audio-visual sessions of 40 minutes each, one per week was conducted for each section in the smart classroom with the help of the respective class teacher. A total of 8 interactive sessions were conducted over two months for both the classes of the intervention school. The sessions were regarding food and nutrients, energy and its role in weight gain, maintenance of ideal body weight through dietary modification and physical activity, stress relaxation including meditation & yoga. They were motivated to do a minimum of 30 minutes of physical activity every day which consisted of Surya-namaskar (5 to 10 repetitions), 10 to 15 minutes of brisk walk or run, 15 to 20 minutes of yoga. They were encouraged to play outdoor games minimum of 30 minutes per day.
There was a gap of two months due to the annual examinations of the students. During the summer vacation of the next two months, parents of the overweight/obese students were counselled over the telephone after baseline data analysis.
The intervention activities had been reinforced by personal as well as group interactions in the next six months by conducting one session fortnightly. The activity of each student was observed closely during their physical education class and they were motivated to play outdoor games and to do physical exercises every day. Personal counselling of overweight/obese students was done regarding healthy dietary habits and physical activity. Counselling of the parents of overweight/obese students was done during the parent-teacher meeting. Parents were also contacted over the telephone once in two months. Each parent was contacted at least three times during these six months.
Post-intervention assessment: On completion of the intervention, data were collected to assess the changes in behaviour towards diet and physical activity. All anthropometric measurements and blood pressure measurement of students were again done by the investigator himself both in the intervention school and control school.
Data analysis: The data were entered in a Microsoft Excel spreadsheet and imported to SPSS software version 20 (IBM Corp., Armonk, NY). Descriptive statistics were expressed as proportions, means, median, standard deviations and 95% confidence interval. Independent t-test and paired t-test were performed to compare means of continuous variables. Chi-squared test and McNemer Chi-squared test were used to test the difference of proportions between independent and paired observations respectively. A P-value less than 0.05 considered statistically significant.
Methods adopted physical examination: Height was measured by using a stadiometer without shoes, to the nearest 0.1 cm. Weight was measured by an electronic weighing machine with uniform after removal of shoes. BMI was defined as the weight in kilograms divided by the square of the height in meters (kg/m2). BMI of students was classified as per the recommendation of Khadilkar VV et al.9 They were categorized using BMI percentile curves for Indian boys and girls from 5-17 years with 3rd, 10th, 25th, 50th, 85th and 95th percentiles, along with two additional percentiles corresponding to a BMI of 23 and 28 kg/m2 at 18 years. They were classified as: underweight (BMI <3rd percentile), normal (BMI 3rd percentile to the adult equivalent of BMI <23), overweight (Adult equivalent of BMI 23 to adult equivalent of BMI 27.99) or obese (adult equivalent of BMI >28).
Measurement of waist: Waist circumference was measured done at the approximate midpoint between the lower margin of the last palpable rib and the top of the iliac crest using stretch?resistant tape to the nearest 0.1 cm. Measurement of hip circumference was measured done at around the widest portion of the buttocks to nearest 0.1 cm.10 Blood pressure (BP) was measured with a clinical sphygmomanometer and a stethoscope. Normal BP was defined as systolic blood pressure (SBP) and diastolic blood pressure (DBP) less than the 90th percentile for sex, age, and height. Hypertension was defined as average SBP or DBP greater than or equal to the 95th percentile for sex, age, and height on at least three separate occasions. Average SBP or DBP levels that are greater than or equal to the 90th percentile had been designated as elevated BP and were considered to be an indication of heightened risk for developing hypertension.11 In this study, Blood pressure was measured 3 times at 0, 5 and 30 minutes and the average of readings was taken.
Ethical considerations: Approval for the study was obtained from the Institutional Ethics Committee of the medical college with reference number IMS-SH/SOA/16074.
RESULTS
In this quasi-experimental study conducted in the two private schools, a total of 173adolescent students have participated. Among these students, 86 were from the control school and 87 were from the intervention school.
The mean age was 13.46 ± 0.75 years ranging from 12-15 years. About 60% of participants were boys, 98.8% were Hindus, 95.4 % belonged to the general caste. Near two-third (65.3%) belonged to nuclear families, 50.3% had no siblings. The majority of the father of the students were graduate (69.3%) while the majority of the mothers had higher secondary education (61.8%). The majority of the father of the students were clerical staff/ shop owners (45.7%) while the majority of mothers were homemaker (84.3%). Family history of obesity was found in 35.8% of students had (Father-18%, Mother-10%, Both parents - 8.2%) and 5.8% had a history of obesity among their siblings. No significant difference was found between control and intervention schools in socio-demographic characteristics and family history of obesity between both schools.
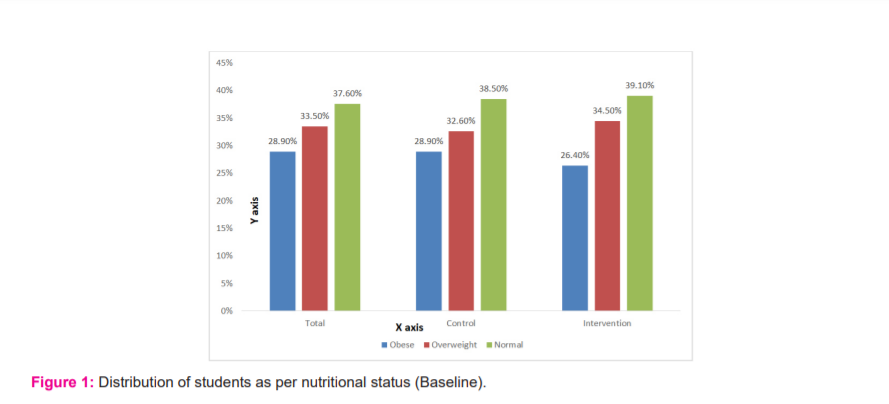
In this study, proportion of overweight/ obesity was found to be 62.4% (obese-28.9%, overweight-33.5%). In control school, 32.6% of the students were overweight and 28.9% were obese. In intervention school, 34.5% were overweight and 26.4% were obese. (Fig 1)There was no significant difference found between the intervention and control group at baseline (p=0.770).
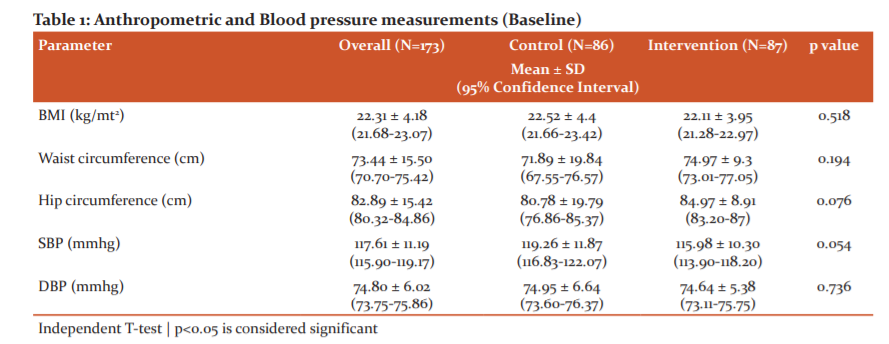
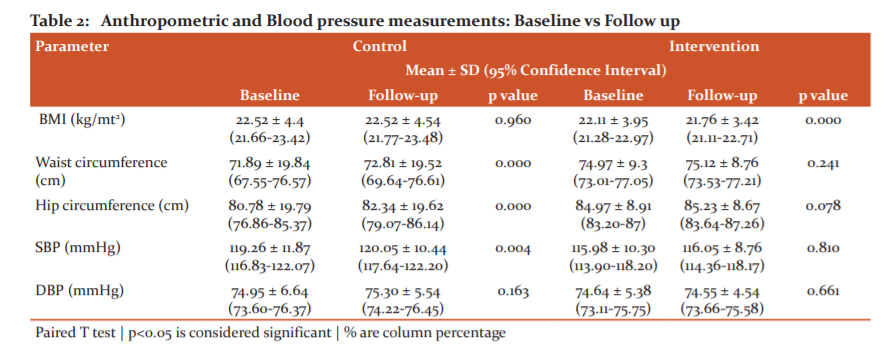
In baseline anthropometric measurements of the students, no significant difference was seen among the control and intervention group. The mean BMI of the students of the control school was 22.52 ± 4.4 and of intervention, the school was 22.11 ± 3.95. (Table 1) After one year, the mean BMI of the students of the control school was 22.52 ± 4.24 and of intervention, the school was 21.76 ± 3.42. A significant decrease was observed in BMI among students of the intervention group. Waist and hip circumference significantly increased in the control group. No significant change was observed in BP in both groups during follow up, except there was a significant increase in SBP in the control group (p=0.004). (Table 2)
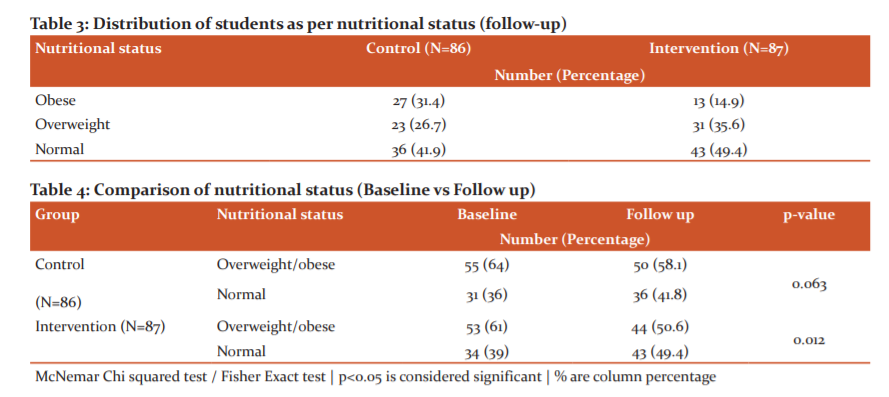
During follow up, in control school, 26.7% of the students were overweight and 31.4% were obese. In intervention school, 35.6% were overweight and 14.9% were obese. (Table 3)There was a significant reduction in the proportion of overweight/obese students in intervention school (p=0.012). (Table 4)
In control school 16.3% students had elevated SBP, 3.5% had elevated DBP and 20.9% had both elevated SBP & DBP. In intervention school, 6.9% had elevated SBP. 6.9% had elevated DBP and 13.8% had both elevated SBP & DBP. There was no significant difference was observed between both the groups at baseline (p=0.084). During follow up, in control school, 36% had elevated BP (elevated SBP-12.8%, elevated DBP- 4.7% and both elevated SBP & DBP-18.6%). In intervention school 18.4% had elevated BP (elevated SBP-8%, elevated DBP- 3.4% and both elevated SBP & DBP-6.9%). There was a significant decrease of students with elevated BP in the intervention group (p=0.008).
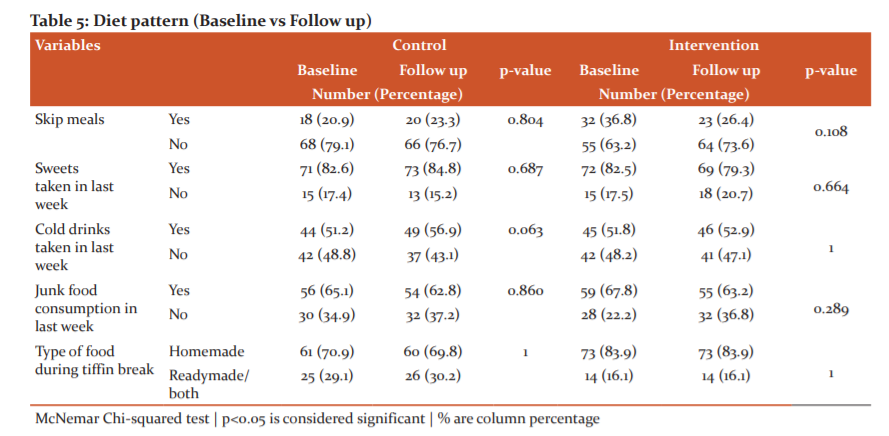
There was improvement seen among the intervention group in terms of not skipping meals as the percentage of students not skipping meal increased 63.2% to 73.6% but it was not statistically significant. No significant difference was observed from baseline to follow up among both the groups in taking junk foods, sweets, cold drinks in last week and type of food in tiffin break in school. (Table 5)
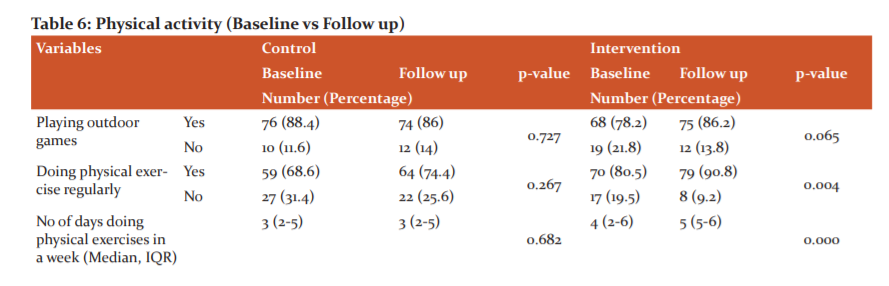
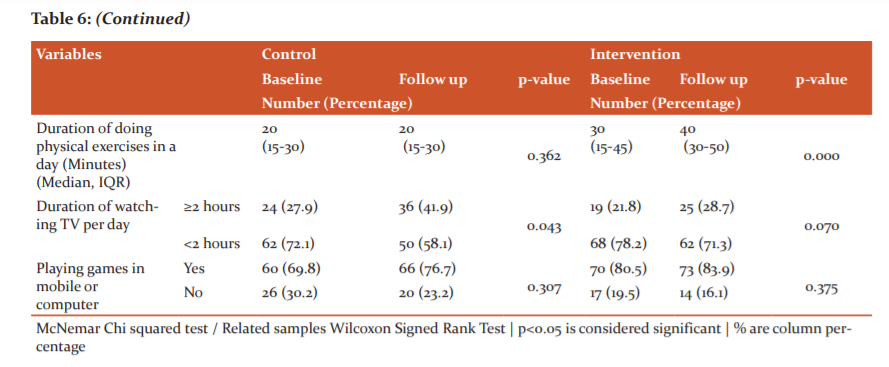
There was increased activity found in the intervention group in doing regular physical exercise (p=0.004). Median days of doing physical exercise as well as the median duration (minutes) of doing physical exercises have been increased significantly among students of intervention school (p=0.000). No significant change was observed in the duration of watching TV and in playing games on mobile or computer in the intervention group. Among the control group, a significant increase of students watching TV for more than two hours was observed (p=0.043). (Table 6)
DISCUSSION
This study was carried out to assess the change in anthropometric parameters following lifestyle interventions related to obesity among school-going adolescents.
Overall, several variables were indicative of positive changes in anthropometric measurements after the intervention. After the intervention, a significant decrease in BMI was seen among students of intervention school. Tracking obesity in adolescents and intervening early may decrease the risk of obesity and non-communicable diseases in adulthood. Robertson et al. reported significant BMI changes in children (7-13 years of age) who were obese and participated in a 12-week intervention involving one 2.5 hour exercise session each week. 12 Savoye et al. also found anthropometric changes of obese children (8-16 years of age) who participated in a 6-month program with weekly two exercise sessions. 13 In this study, no significant change was seen in the waist and hip circumference among students of intervention school while a significant increase in the waist and hip circumference was seen among students of control school. This might be due to lifestyle-related interventions in intervention school.
During the follow up after one year, it was observed that there was a significant reduction in the proportions of overweight/obese students in intervention school (p=0.012), but no significant reduction was found in the control school. Initially, there were 26.4% obese students in intervention school and after one year 14.9% of students were obese in that school. But a slight increase in the percentage of overweight students has been detected (from 34.5% to 35.6%) among them. This might be due to the inclusion of those students who have entered into the overweight category from the obese category after the intervention. In a study done by Gortmaker S L et al. significant reduction of the prevalence of obesity was seen from 23.3% to 20.3% among the students of intervention school after two years of intervention.14 In a randomised controlled trial RCT done by Simon et al. it was observed that intervention students had a lower increase in BMI over time than controls. 15 In another study done by Sichieri R et al. after one year of intervention, a non-significant overall reduction was seen in BMI but the intervention group showed greater BMI reduction, and this difference was statistically significant among girls, but no change was observed in the prevalence of overweight/ obesity. 16 In another policy-based school intervention, it was seen that intervention resulted in a 50% reduction in the incidence of overweight in two years.17
In this study, it was observed that elevated blood pressure was more in overweight/ obese adolescents (P=0.000). Many researchers have already said that overweight or obesity greatly increased the risk of hypertension in children and adolescents.12,18 There were no significant differences seen in changes in mean SBP and DBP among the students of the intervention group but a significant increase in SBP was observed among the students of the control school. A significant decrease was observed among the intervention group in the proportion of elevated BP during follow up. A similar finding was seen in an RCT done by Savoye et al.13 In another study done by Bayne-Smith M et al. significant decrease was observed in both SBP and DBP after 12 weeks of intervention. 19
The lifestyle changes and personal development in adolescence to early adulthood period may influence dietary behavior. It was observed that among the students, breakfast was the most skipped meal at baseline. During the follow up, change observed in diet habits of students of intervention school and proportion of students not skipping meals was increased but not statistically significant, while no change was seen among students of control school. Similar finding was seen in the study done by Bayne-Smith M et al.19 Changing the dietary habit is difficult to introduce in children and adolescents, suggestions for interventions to change dietary habits in adolescents who are overweight or obese could include increasing the supervision during eating by guardians, increase awareness among parents and restricting junk foods in tiffin break by school authorities.
There is good evidence that school-based physical activity interventions are effective in promoting a healthy lifestyle and fitness but the evidence for a beneficial effect on obesity levels and cardio-metabolic outcomes remains inconsistent.20 In our study, the physical activity of the students of the intervention group has improved after this intervention program. The proportion of students doing regular physical exercises found to be increased significantly (p=0.004) in intervention school. A significant increase was also seen in the duration of doing physical exercises among them. Haerens L et al. reported a statistically significant increase in the duration of physical activity among adolescents after 6 months of intervention.21 Other studies have also reported improvement in physical activity after intervention done in schools.15, 22, 23 It is evident that school-based interventions are effective, in increasing the time, children and adolescents engaged in physical activity, particularly during school hours.
There was no significant change was seen in watching TV and playing games on mobile or computer in both the groups during the follow-up. A decrease in the duration of TV watching was seen after intervention in studies done by James J et al. and Simon C et al.24,15
Integrating educational programs on healthy lifestyle in schools may be an effective strategy to have an impact on changing lifestyle and prevent and control obesity among adolescent children which was seen in this study.
CONCLUSION
Schools are the best avenue to address the problem of overweight and obesity. This school-based intervention program on healthy lifestyle significantly decreased BMI, blood pressure, and improved eating habits, physical activity among adolescents. Therefore, school-based simple educational intervention program along with more game periods and yoga classes should be emphasized to reduce overweight/obesity among adolescents.
LIMITATIONS
The study included only private school students, so the generalization of the outcome of this study may be limited. The dietary habit and physical activity of the study participants were assessed based on self-reported information.
Acknowledgement:
We extend our sincere thanks to the study participants and school authorities for their support and involvement in the study.
Conflict of interest: Nil
Funding: Self-funded
Contribution of authors:
Dr Arijit Kundu: 1. Concept and design; 2. Collection and interpretation of data; 3. Drafting the article; 4. Final approval of the version to be published.
Dr Lipilekha Patnaik: 1. Concept and design; 2. Collection and interpretation of data; 3. Drafting the article; 4. Final approval of the version to be published.
Dr Trilochan Sahu: 1.Concept and design 2. Drafting the article; 3.Collection and interpretation of data. 4. Final approval of the version to be published.

References:
- Bundred P, Kitchiner D, Buchan I. Prevalence of overweight and obese children between 1989 and 1998: population-based series of cross-sectional studies. Br Med J. 2001;322:326-28.
- Ogden CL, Flegal KM, Carroll MD, Johnson CL. Prevalence and trends in overweight among US children and adolescents, 1999-2000. JAMA. 2002; 288: 1728-32.
- Lavie CJ, Milani RV, Ventura HO. Obesity and cardiovascular disease: risk factor, paradox, and impact of weight loss. J Am Coll Cardiol. 2009;53: 1925-1932
- World Health Organisation (WHO) 2005. Preventing chronic diseases: A vital investment, WHO Global report.
- Singh AS, Mulder C, Twisk JW, Mechelen VW, Chinapaw MJ. Tracking of childhood overweight into adulthood: A systematic review of the literature. Obes Rev.2008; 9:474–88.
- Ludwig DS. Childhood obesity- the shape of things to come. N Engl J Med 2007;357:2325-27.
- Obesity: preventing and managing the global epidemic. Report of a WHO consultation. (WHO Technical Report Series, No.894). Geneva, World Health Organisation 2000.
- Caroline M. Apovian. The Obesity Epidemic — Understanding the Disease and the Treatment. N Engl J Med [Internet]. 2016; 374 (2):176–7.
- Khadilkar V, Khadilkar A, Sa C, Borade A, SA C. Body Mass Index Cut-offs for Screening for Childhood Overweight and Obesity in Indian Children. Indian Pediatr. 2012; 49(1):29–34.
- WHO. Waist Circumference and Waist-Hip Ratio: Report of a WHO Expert Consultation. Geneva, World Heal Organ. 2008;8–11.
- Flynn JT, Kaelber DC, Baker-Smith CM, Blowey D, Carroll AE, Daniels SR, de Ferranti SD, Dionne JM, Falkner B, Flinn SK, Gidding SS. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Paediatrics. 2017;140(3).
- Robertson W, Friede T, Blissett J, Rudolf MCJ, Wallis M, Stewart-Brown S. Pilot of “families for health”: Community-based family intervention for obesity. Arch Dis Child. 2008;93(11):921–26.
- Savoye M, Shaw M, Dziura J, Tamborlane W V., Rose P, Guandalini C, et al. Effects of a Weight Management Program on Body Composition and Metabolic Parameters in Overweight Children. J Am Med Assoc. 2007;297(24):2697–704.
- Gortmaker SL, Peterson K, Wiecha J, Sobol M, Dixit S, Fox MK, et al. Reducing Obesity via a School-Based Intervention Among Youth. Arch Pediatr Adolesc Med. 1999;153(4):409–18.
- Simon C, Schweitzer B, Oujaa M, Wagner A, Arveiler D, Triby E, et al. Successful overweight prevention in adolescents by increasing physical activity: A 4-year randomized controlled intervention. Int J Obes. 2008; 32(10):1489–98.
- Sichieri R, Paula Trotte A, De Souza RA, Veiga G V. School randomised trial on prevention of excessive weight gain by discouraging students from drinking sodas. Public Health Nutr. 2009;12 (2):197–202.
- Foster GD, Sherman S, Borradaile KE, Grundy KM, Vander Veur SS, Nachmani J, et al. A Policy-Based School Intervention to Prevent Overweight and Obesity. Paediatrics. 2008;121(4):794–802.
- Njelekela MA, Muhihi A, Mpembeni RNM, Anaeli A, Chillo O, Kubhoja S, et al. Knowledge and attitudes towards obesity among primary school children in Dar es Salaam, Tanzania. Niger Med J . 2015;56(2):103–8
- Bayne-Smith M, Fardy PS, Azzollini A, Magel J, Schmitz KH, Agin D. Improvements in heart health behaviors and reduction in coronary artery disease risk factors in urban teenaged girls through a school-based intervention: The PATH program. Am J Public Health. 2004;94(9):1538–43.
- Chen Y, Ma L, Ma Y, Wang H, Luo J, Zhang X, et al. A national school-based health lifestyles interventions among Chinese children and adolescents against obesity: rationale, design and methodology of a randomized controlled trial in China. BMC Public Health. 2015;15:210.
- Haerens L, De Bourdeaudhuij I, Maes L, Cardon G, Deforche B. School-Based Randomized Controlled Trial of a Physical Activity Intervention among Adolescents. J Adolesc Heal. 2007;40(3):258–65.
- Caballero B, Clay T, Davis SM, Ethelbah B, Rock BH, Lohman T, et al. prevention of obesity in American Indian schoolchildren. Am J Clin Nutr.2003;78(5):1030–8.
- Kafatos A, Manios Y, Moschandreas J, Ioanna A, Froso B, Caroline C, et al. Health and nutrition education in primary schools of Crete: Follow-up changes in body mass index and overweight status. Eur J Clin Nutr. 2005;59(9):1090–2.
- James J, Thomas P, Kerr D. Preventing childhood obesity: Two-year follow-up results from the Christchurch obesity prevention programme in schools (CHOPPS). Br Med J. 2007;335 (7623):762–4.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License