IJCRR - 13(6), March, 2021
Pages: 96-100
Date of Publication: 20-Mar-2021
Print Article
Download XML Download PDF
Assessment of Awareness of Glaucoma Patients on Risk of Glaucoma in Close Relatives and to Determine its Prevalence
Author: Meena M, V. Panimalar A. Veeramani, Divya N, Bindu Bhaskaran
Category: Healthcare
Abstract:Introduction: Glaucoma is a multifactorial, chronic and progressive optic neuropathy that results in visual field defects and it is commonly associated with increased intraocular pressure. It is one of the most important causes of irreversible blindness left untreated. Objective: This study aims to assess awareness of glaucoma patients on the risk of development of glaucoma in close relatives and to determine the prevalence of glaucoma in close relatives. Methods: This is a self-designed questionnaire-based study with three sections consisting of demographic details and questions about knowledge and awareness of the patients. One hundred participants attending the ophthalmology outpatient department of a tertiary care hospital filled the questionnaire. Results: According to the responses obtained, 44 (44%) patients were unaware of the term glaucoma until they were diagnosed with the disease. Only 24(24%) patients had actual knowledge about glaucoma. It is also seen that positive family history is seen as a risk factor in only 30(30%) patients. Only 19(19%) of the patients urged their relatives to get screening to post their diagnosis out of which 7(36.8%) patients had one or more relatives diagnosed with glaucoma. Conclusion: Awareness can be increased by mass media announcements, health programs and Ophthalmologists at the time of diagnosis and follow up by educating diagnosed patients and also encouraging them to instruct their relatives to undergo screening. This creates positive health-seeking behaviour leading to early diagnosis and better prognosis of glaucoma.
Keywords: Knowledge, Awareness, Glaucoma, Family History, Relatives
Full Text:
INTRODUCTION
Glaucoma is one of the leading causes of irreversible blindness worldwide. Based on the available data, there are approximately 11.2 million people aged 40 years and older with glaucoma in India.1 Studies have shown that 50 - 90% of glaucoma cases remain undiagnosed2 and a large number of cases are diagnosed at a later stage of the disease.3 Lack of awareness about glaucoma is an important reason for its late presentation,4 which increases the risk of blindness due to glaucoma.5 It has been estimated that almost 90% of glaucoma-related blindness can be prevented with early and proper treatment.6 For effective treatment to be possible, awareness about the disease is extremely crucial.
The spread knowledge regarding some well-recognized risk factors of glaucoma may enhance more awareness. These include positive family history. A positive family history of glaucoma encourages a search for the presence of the disease and its assessment among the family members and thus increases health-seeking behaviour. A study by Leske et al. reported a positive family history of 13% to 25% and has been proven to be an important risk factor for the disease.7 Several studies have also indicated that most individuals do not have an accurate understanding and knowledge of this disease despite being aware of this disease8. Thus the assessment of awareness is the first step in the planning of disease management.
This study deals with the assessment of awareness and knowledge of glaucoma in diagnosed patients, awareness about positive family history and prevalence of the same.
MATERIALS AND METHODS
This is a population-based study, using a questionnaire exploring the details of awareness and knowledge of glaucoma among known glaucoma patients with special interest in the inheritance and positive family history. It was conducted in the ophthalmology outpatient department of Saveetha Medical College, a tertiary care centre between January 2020 and March 2020. The study was approved by the Institutional Medical Ethics Committee. Written informed consent was obtained from all the participants after explaining the nature of the study. IEC no: SMC/IEC/2020/03/377
Data collection
All the patients above 40 years, diagnosed with glaucoma were chosen randomly and a self-designed questionnaire (in English and Tamil) was distributed to the participants. Illiterate patients had questions read out to them by nurses and interns to prevent interviewer bias. Patients with any other eye disorder except glaucoma were excluded.
The questionnaire had three sections – The first section about information about the patient's demographic characteristics (age, gender, education level and socioeconomic data). Section two was designed to know the patient's awareness of the disease through six multiple-choice questions. Section three was based on knowledge about glaucoma, through eleven multiple-choice questions. Awareness was defined as ‘having heard of glaucoma’. Knowledge was defined as when the subject had some understanding of glaucoma in terms of cause and/or symptoms.
Data analysis
All responses were tabulated using Microsoft Excel software. Graphical representations were made in places necessary. Statistical analysis was done using SPSS software and p-value <0.05 was considered to be significant.
RESULTS
Data of all the patients diagnosed with glaucoma attending the ophthalmology department was collected. In total, 100 patients were included in the study based on inclusion and exclusion criteria.
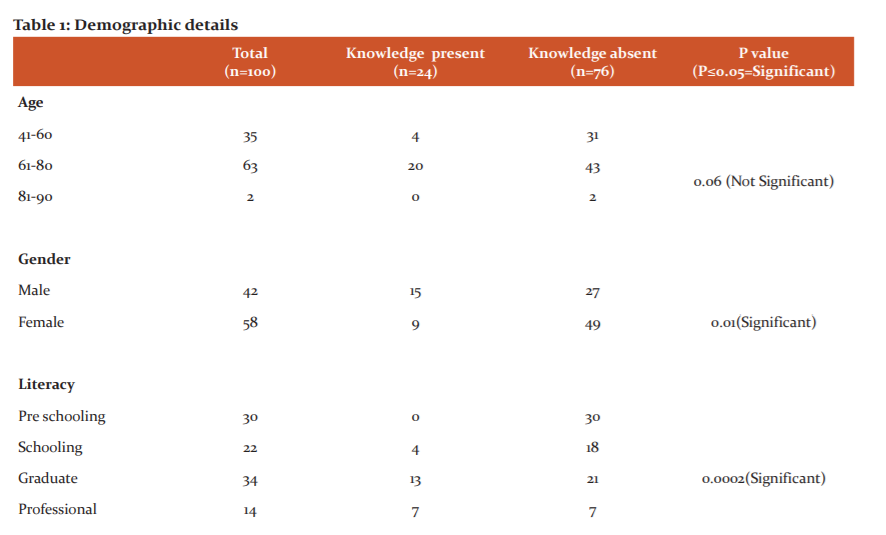
Demographic details
Table 1 showed different demographic characteristics of the population participated in this study.
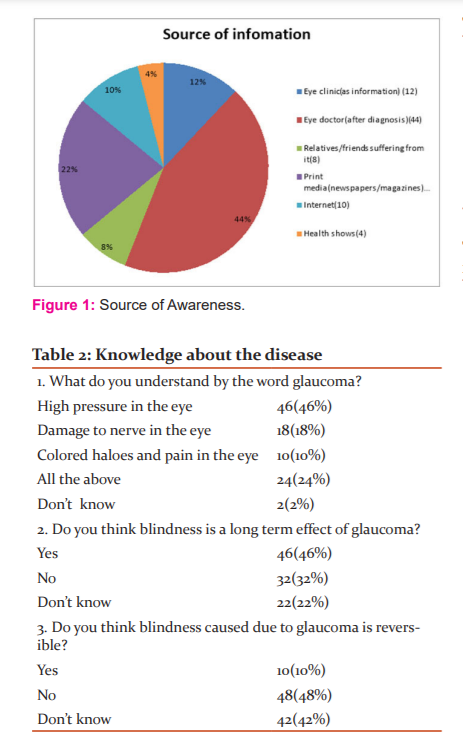
Awareness
All 100 subjects were aware of glaucoma as they were diagnosed with the disease. In Chart 1 source of information about glaucoma is presented. 74(74%) people were not aware of the normal intraocular pressure. Out of 100 patients, 54(54%) patients got a check-up every six months or less and 42 (42%) patients got a check-up every year. The most common form of treatment seen in diagnosed patients was eye drop medication (74%) followed by laser(18%).
Knowledge
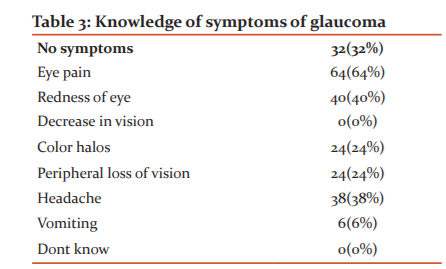
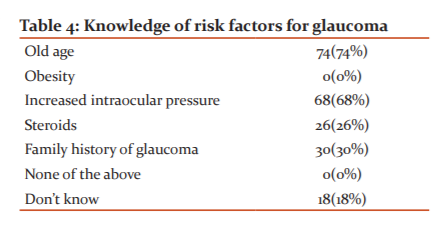
Table 2 showed understanding of the term glaucoma. Only 24(24%) patients understood the term glaucoma. Table 3 represented knowledge about symptoms is seen. Only 32 (32%) patients are aware of the presence of an asymptomatic course of glaucoma. Table 4 depicted knowledge about risk factors is seen. Old age (74%), increased intraocular pressure (68%) were considered to be the most common risk factors.
Eye drop medication was believed to be the mode of treatment in 54(54%) people. The most common comorbid conditions associated with glaucoma was diabetes and hypertension. Table 5 is details about the knowledge about Family history. Only 30 people (30%) mentioned that positive family history of glaucoma could be a risk factor and it is important for first degree relatives to be concerned with getting the disease, out of these people only 19 (19%) people encouraged first-degree relatives to get a check-up. Prevalence of the disease was seen in one relative in 4 (21.1%) patients, two relatives in 2 (10.5%) patients, three relatives in 1 (5.2%) patients.
DISCUSSION
This study focuses on awareness and knowledge about glaucoma exclusively in diagnosed patients. High levels of awareness and exact knowledge about the disease are important in diagnosed patients to create awareness and encourage family members and friends to get tested. Here in our study, we found out that, in the majority of the patients (44%) source of information of glaucoma was only after their diagnosis of the disease and this indicates a lack of awareness in patients. This was not found following other studies where mass media9, as well as information from friends and family, was the most common source of information.8,10-12 Some studies found that accurate knowledge and awareness was found in patients whose source of information was family members.7,8 Hence this validates the need for proper knowledge and awareness in diagnosed patients.
In this study, only 24% of the patients knew the actual definition of glaucoma. It is also seen that 32% of patients were aware that glaucoma can have an asymptomatic course. This was found to be more when compared to the previous study8 where only 0.7% were aware of a possible asymptomatic course of glaucoma. 10% of the patients thought blindness due to glaucoma was reversible and 42 % didn’t have any knowledge of it. This percentage is more when compared to the study done by Ichhpujani et al13 where 39.5% thought damage due to glaucoma was reversible. Increased intraocular pressure was considered to be an important risk factor in 68% of the patients. This is a significant increase when compared to the study done by Sathyamangalam et al10 where only 8% of patients considered increased intraocular pressure to be a risk factor. 18% of the people were not aware of any risk factors. It is noted that patients in our study had a better knowledge of glaucoma compared to other studies. This could be attributed to the fact that all the subjects were known as glaucoma patients and had some knowledge of glaucoma. But for diagnosed patients this knowledge seems to be less and they need to be further educated.
Even though all were diagnosed glaucoma patients, only 30% of the patients considered presence of positive family history to be a risk factor for glaucoma. This was found in the previous study.14 Though 30% of patients were aware that their relatives had to get tested, only 19% of the patients encouraged their relatives to get tested and this was of major concern. This highlights the lack of complete knowledge regarding the inheritance of the disease and potential danger to the vision if not diagnosed and treated properly. Hence providing information to patients diagnosed with glaucoma regarding the inheritance of the disease and the necessity of screening of their relatives is crucial. This would encourage patients to inform their family regarding the prognosis of the disease and their high chance of being affected by this disease compared to the general population. To achieve this, ophthalmologists and optometrist should educate the diagnosed patients on the serious nature of the disease and urge their patients to encourage their family members to undergo glaucoma screening. Out of the 19 people who encouraged their relatives to get a checkup, 7(36.8%) patients had a prevalence of glaucoma and ocular hypertension in 1 or more members of their family. This was seen following some studies.15-17 In studies conducted by Wolfs et al18 and Vegini et al19 prevalence was found to be 10.4% in siblings of patients and 1.1% in offsprings and 3.9% in siblings and 12.9% in offsprings respectively. The current study cannot be compared with these studies as prevalence in siblings and springs was not found but our study adds to the fact that glaucoma is hereditary and screening of the relatives is mandatory for early detection of glaucoma. It is important to note that increased knowledge, awareness and screening aids in early diagnosis and thus leads to better prognosis and prevention of permanent damage.
CONCLUSION
This study provides data on knowledge and awareness of glaucoma patients on the risk of development of glaucoma in close relatives. The majority of the patients were unaware of the term glaucoma until they were diagnosed with it. Awareness and knowledge can be increased by mass media announcements, health programs and spreading awareness through diagnosed patients to family members. Thus precise knowledge about glaucoma in diagnosed patients is very important and this can be brought about by ophthalmologists educating them and also encouraging them to instruct their relatives to undergo screening. This creates positive health-seeking behaviour leading to early diagnosis and better prognosis of glaucoma.
ACKNOWLEDGEMENT
We the authors of this study are grateful to the management of Saveetha Medical College and hospital for providing us with the necessary facilities for this study. We also acknowledge immense help received from scholars whose articles are cited and referenced in this manuscript. We are also grateful to authors/editors/publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
CONFLICT OF INTEREST: NIL
SOURCE OF FUNDING: NIL


References:
1. Usha BR, Usha MS, Brinda Prasad M, Outcome of conventional trabeculectomy with or without cataract surgery. Int J Curr Res Rev 2015;7(17):20-26.
2.. Vijaya L, George R, Baskaran M, Arvind H, Raju P, Ramesh SV, et al. Prevalence of Primary Open-angle Glaucoma in an Urban South Indian Population and Comparison with a Rural Population. The Chennai Glaucoma Study. Ophthalmology 2008;115(4):648-654.e1.
3. Oliver JE, Hattenhauer MG, Herman D, Hodge DO, Kennedy R, Fang-Yen M, et al. Blindness and glaucoma: a comparison of patients progressing to blindness from glaucoma with patients maintaining vision. Am J Ophthalmol 2002;133(6):764–772.
4. Fraser S, Bunce C, Wormald R. Risk factors for late presentation in chronic glaucoma. Investig Ophthalmol Vis Sci 1999;40(10):2251–2257.
5. Javitt JC. Preventing blindness in Americans: the need for eye health education. Surv Ophthalmol 1995;40(1):41–44.
6. Quigley HA. Number of people with glaucoma worldwide. Br J Ophthalmol 1996;80(5):389–393.
7. Leske MC, Connell AMS, Wu SY, Hyman LG, Schachat AP. Risk Factors for Open-angle Glaucoma: The Barbados Eye Study. Arch Ophthalmol 1995;113(7):918–924.
8. Rewri P, Kakkar M. Awareness, knowledge, and practice: A survey of glaucoma in north Indian rural residents. Indian J Ophthalmol 2014;62(4):482–486.
9. Kizor-Akaraiwe NN, Monye HI, Okeke S. Awareness and knowledge about glaucoma and proportion of people with glaucoma in an urban outreach programme in Southeast Nigeria. BMJ Open Ophthalmol 2017;1(1):e000018.
10. Sathyamangalam RV, Paul PG, George R, Baskaran M, Hemamalini A, Madan R V., et al. Determinants of glaucoma awareness and knowledge in urban Chennai. Indian J Ophthalmol 2009;57(5):355–360.
11. Pfeiffer N, Krieglstein GK, Wellek S. Knowledge about glaucoma in the unselected population: A German survey. J Glaucoma 2002;11(5):458–463.
12. Tenkir A, Solomon B, Deribew A. Glaucoma awareness among people attending ophthalmic outreach services in Southwestern Ethiopia. BMC Ophthalmol 2010;10:17.
13. Ichhpujani P, Bhartiya S, Kataria M, Topiwala P. Knowledge, attitudes and self-care practices associated with glaucoma among hospital personnel in a tertiary care center in North India. J Curr Glaucoma Pract 2012;6(3):108–12.
14. Celebi ARC. Knowledge and Awareness of Glaucoma in Subjects with Glaucoma and their Normal First-Degree Relatives. Med hypothesis, Discov Innov Ophthalmol J 2018;7(1):40–7.
15. Mitchell P, Rochtchina E, Lee AJ, Wang JJ. Bias in self-reported family history and relationship to glaucoma: The Blue Mountains Eye Study. Ophthalmic Epidemiol 2002 Dec;9(5):333–345.
16. Gramer G, Weber BHF, Gramer E. Results of a patient-directed survey on frequency of family history of glaucoma in 2170 patients. Investig Ophthalmol Vis Sci 2014;55(1):259–264.
17. Nguyen RL, Raja SC, Traboulsi EI. Screening relatives of patients with familial chronic open angle glaucoma. Ophthalmology 2000;107(7):1294–1297.
18. Wolfs RCW, Klaver CCW, Ramrattan RS, Van Duijn CM, Hofman A, De Jong PTVM. Genetic risk of primary open-angle glaucoma: Population-based familial aggregation study. Arch Ophthalmol 1998;116(12):1640–1645.
19. Vegini F, Figueiroa Filho N, Lenci RF, Neto DG, Susanna R. Prevalence of open angle glaucoma in accompanying first degree relatives of patients with glaucoma. Clinics ((Sao Paulo) 2008;63(3):329–32.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License