IJCRR - 10(15), August, 2018
Pages: 15-19
Date of Publication: 16-Aug-2018
Print Article
Download XML Download PDF
Development of Polymerase Chain Reaction Assay for Targeting Cytochrome C Maturation F (ccmF) Gene of Leptospira
Author: Potdar Gayatri A., Dhotre Dheeraj P., Pol Sae S., Bharadwaj Renu S.
Category: Life Sciences
Abstract:Leptospirosis is a bacterial zoonotic disease caused by spirochetes of the genus Leptospira. The direct method of diagnosis of Leptospirosis has been so far by culture isolation but isolation rate of the microorganism from clinical specimens is low. The additional conventional method is the detection of antibodies which is done by ELISA, that fails to identify the infecting serovar. MAT is used as the gold standard, but it can only confirm the disease at a later acute phase because anti-Leptospira antibodies usually become measurable only 5 to 7 days after onset of illness. Thus, serology does not contribute to early diagnosis of Leptospirosis. To overcome these limitations, we developed PCR assay targeting ccmF gene of Leptospires using in-house designed RGf and RGr primers, with a product size of 910bp. The protocols were standardized. PCR could detect the target bacterial gene without any ambiguity. This simple, cost-effective and rapid method can be applied to detect causative Leptospira interrogans serovars from the isolates.
Keywords: PCR, ccmF gene, Molecular detection
Full Text:
Introduction:
Leptospirosis is a disease that is caused by spirochetes, members of the genus Leptospira. It is well illustrated as the frequent zoonosis in the world. Leptospirosis is most common in the tropics and distributed worldwide (except in the Polar Regions) (1). Under reporting is a major concern in analyzing the actual incidence of leptospirosis in many Asian countries (2). In India, it is directly related to either monsoons or poor sanitary conditions, with multiple epidemics reported (3–6).
For quick epidemiological response and also for timely treatment paradigms, rapid and simple assays that can reliably detect and distinguish Leptospira are necessary. Combining clinical proficiency and alertness with confirmatory laboratory back up noticeably increases the recognition of patients with Leptospirosis. As the clinical features are imprecise, laboratory test play a key role in diagnosis of Leptospirosis (7).
Since isolation rate of the microorganism from clinical specimens is low, often due to the prior indiscriminate use of antibiotics, serological techniques remain the cornerstone of diagnosis. The analysis of acute- and convalescent-phase sera by ELISA and the microscopic agglutination test (MAT). MAT is used as the gold standard, but it and can only confirm the disease at a later acute phase because anti-Leptospira antibodies usually become measurable only 5 to 7 days after onset of illness.
Hence, serology does not contribute to early diagnosis of Leptospirosis. Early diagnosis is obligatory because antibiotic treatment is most valuable when it is initiated early in the course of the disease. It is imperative to note that, in distinction to many of the resembling diseases (e.g. dengue), leptospirosis can easily be treated with antibiotics. This is provided that the diagnosis is confirmed in the first week of disease onset, when treatment with antibiotics is most effectual. Thus to facilitate preliminary treatment at the most effective time point, the availability of an accurate diagnostic test that is needed in the early acute phase of the disease.
Alternative methods were developed to assess the presence of leptospires in clinical samples like immune peroxidase staining (8), Immuno fluorescence staining (9) and DNA hybridization (10). These were useful methods for the detection of Leptospira, provided that the micro-organisms should present in fairly large numbers. These were not satisfactory for routine diagnostic purposes, mainly because of their lack of sensitivity.
Rapid recognition of small numbers of leptospires may become realistic due to precise amplification of Leptospiral DNA (11,12). PCR is a sensitive, specific, and rapid technique which has been successfully applied to the detection of several microorganisms and viruses in a variety of clinical specimens, including sputum, serum, cerebrospinal fluid, urine, faeces, and various tissues. PCR can rapidly confirm the detection in the early phase of the disease and before antibody titres are at detectable levels.
Several PCR assays have been developed for the detection of leptospires species, and that are unable to detect Leptospira at serovar level. It is epidemiologically important to identify the infecting Leptospira serovars, as they may be associated with certain animal host species. So the appropriate control measures can be instituted.
The aim of this study was to identify the gene with potential to enhance Leptospira serovar discrimination by sequencing-based methods. We used bioinformatics tools to check the discriminatory power of existing genes. Previously deposited sequence data were evaluated by phylogenetic analyses
Materials and Methods:
Computational determination of discriminatory powers of housekeeping genes
Thirteen housekeeping genes were selected in a present study by comparison between two Leptospira genomic sequences available in gene bank (http://www.ncbi.nlm.nih.gov) those of L. interrogans serovars Copenhageni strain Fiocruz L1-130 chromosome I (accession number AE016823.1) and L. interrogans serovar Lai strain 56601 chromosome I (accession number AE010300.1)
Multiple sequence alignments (MSA) for these sequences were carried out using CLUSTALX Version 2.1 software (13). Multiple Sequence Alignments were manually edited to remove ambiguities using DAMBE software (14). Polymorphic sites were counted and percent polymorphism for each gene was determined (Table: 1).
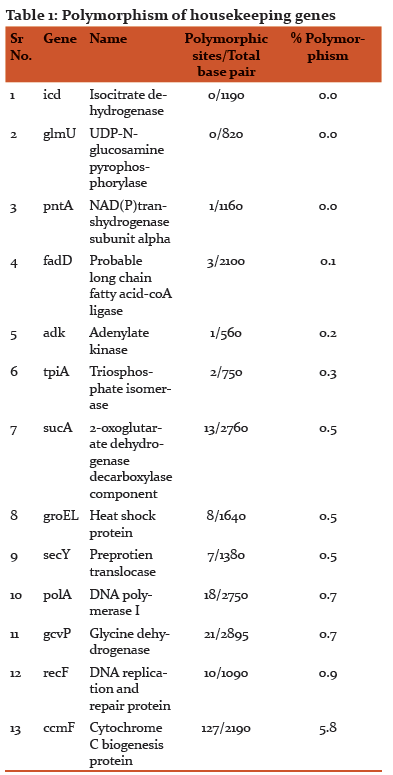
Primer Design:
As ccmF gene was found to have maximum percent polymorphism (i. e. 5.8%), and was selected for further study.
Primer 3 software was used to design primers for the hyper variable region of ccmF gene (15). In order to ensure optimal primer pair, primer length was set 20 bp, Tm was set at 450C to 600C, and the difference between forward and reverse primer sets was minimized (within 20C). The target value for primer GC content was 50–60%. No secondary structures within primers were allowed. All above parameters were manually checked by Generunner (http://ftparmy.com/130936-gene-runner.html) software.
To check the lack of sequence homology with other bacterial or eukaryotic DNA sequences, designed primer sequences were checked for with a primer BLAST (NCBI, Bethesda, MD)(http://blast.ncbi.nlm.nih.gov/Blast.cgi) search. In silico designed primer pairs were synthesized by commercial manufacturer (Sci Fi biological) and were named as RGf and RGr primers.
Utility of primers:
DNA extraction from standard serovars:
Five Leptospira interrogans serovars were obtained from National Leptospirosis Reference Centre, Regional Medical Research Centre in Port Blair, Andaman and Nicobar islands (listed in table: 2).
The serovars were grown in Ellinghausen–McCullough–Johnson–Harris (EMJH) media (BD, Sparks, MD) at 300C for 6–8 days. Leptospiral DNA was isolated from standard cultures with a Qiagen Blood and Cell Culture DNA Mini kit (Qiagen, Valencia, CA).

PCR standardization:
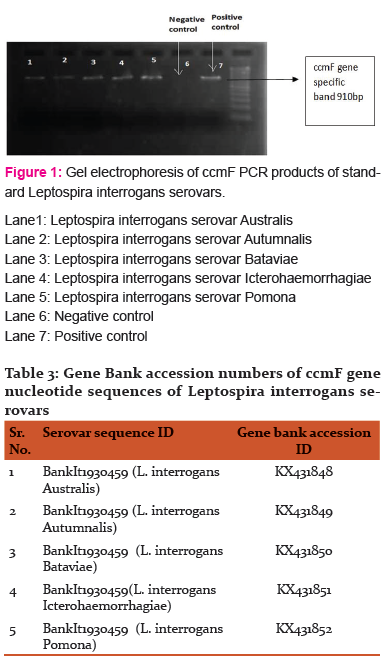
A total reaction volume of 25 µL consisted of 10 µL Qiagen Master Mix, 1.5 µL of forward primer (2 pmol /µL stock), 1.5 µL of reverse primer (2 pmol /µL stock), 10 µL nuclease-free water and 2 µL DNA template. For negative controls, nuclease-free water was used instead of the DNA template. Samples were run for 2 min at 940C, followed by 30 cycles of 30 s at 94 0C, 30 s at 550C and 30 s at 72 0C on a Gene Amp PCR System 9700 (Applied Biosystems, Foster City, CA) At the end of the 30 cycles was an extension period of 7 min at 720C. PCR products were visualized on a 2% agarose gel and documented with a Gene Flash gel documentation system (Syngene, Frederick, MD). Each sample was run at least two times for reproducibility (Fig 1).
Gene amplicons were sequenced using ABI 3730xl and sequences were submitted to NCBI to get accession numbers (Table 3).

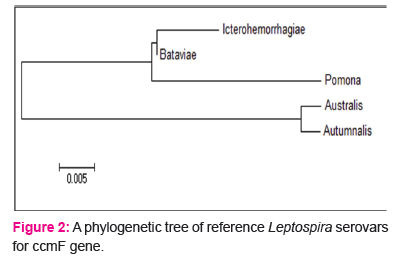
Phylogenetic tree of L. interrogans serovars for ccmF gene
Multiple sequence alignment (MSA) for sequences of standard leptospira serovars was carried out using CLUSTALX Version 2.1 software. Multiple Sequence Alignment was manually edited to remove ambiguities using DAMBE software.
Polymorphic sites were counted and percent polymorphism for ccmF gene was determined. Phylogenetic tree was constructed by Neighbour Joining method using MEGA5 software package (16).
Specificity testing of primers
To check cross-annealing of primers with other species, ccmF primers designed were tested against the isolates of Bacillus cereus, Escherichia coli, Candida tropicalis, Salmonella typhi, Staphylococcus aureus and Mycobacterium tuberculosis.
DNA was isolated from these cultures with a Qiagen Blood and Cell Culture DNA Mini kit, and were tested by ccmF gene PCR.
Results:
ccmF gene (encoding Cytochrome C biogenesis protein) had maximum percent polymorphism i.e 5.8% among other genes studied. Thus it was selected for further studies and primers were designed and PCR was standardized.
BLAST output of primers showed high degree of specificity for Leptospira species.
The size of the amplification products corresponded to the expected fragment size i.e. 910 bp.
The genetic distance between the L. interrogans serovars in the phylogenetic tree is represented by a bar which represents 0.005 nucleotide substitutions per alignment position among the serovars. This demonstrates variations in the sequence homology of ccmF gene which reflects in genetic diversity. All the Leptospira interrogans serovars under study were segregated from each other (Fig: 2).
Primer sets produced only amplification products for standard Leptospiral serovars and not the other test organisms.
Discussion
In the last two decades, several PCR assays for the detection of Leptospires have been illustrated. PCR should generate an amplicon with sequence variability appropriate for phylogenic assessment for molecular epidemiological purposes.
The techniques such as, Restriction fragment length polymorphism analysis (17,18), ribotyping (17), pulsed-field gel electrophoresis (19) DNA hybridization (20), variable-number tandem-repeat analysis, arbitrarily primed PCR (APPCR), low-stringency single specific primer PCR (LSSP-
PCR), PCR restriction endo- nuclease analysis (PCR-REA) (21) etc. are available for Leptospira serovar identification.
However, fragment length polymorphism, ribotyping and pulsed-field gel electrophoresis are laborious, and time-intensive and require significant amounts of genomic DNA, whereas methods such as AP-PCR and LSSP-PCR result in complex banding patterns, DNA-DNA hybridisation is laborious and requires the use of radio-labelled isotopes. Hence cannot be used for routine diagnostic purposes.
Here we described the use of bioinformatics to identify novel gene i.e ccmF gene which is having potential of discrimination between Leptospira serovars.
PCR tests developed by other researchers also provide fast testing platforms, but the primers used can only differentiate between Leptospira species and have some disadvantages.
Primers presented in this study provide the ability to detect and differentiate between Leptospira interrogans serovars, that will be especially useful in epidemiological studies as the source for disease outbreaks.
ccmF gene codes for cytochrome c-type biogenesis protein CcmF. Cytochrome C is found in respiratory or photosynthetic electron transport chain, contain covalently bound heme. Bacterial C type cytochromes are extra cytoplasmic proteins and can be soluble and membrane bound. Presently we know 12 bacterial genes which control cytochrome C maturation ccm (ABCDEFGHI) res ABC and four genes that control redox state of the cell.
ccmF gene is housekeeping gene, present in pathogenic and non pathogenic Leptospira which codes for cytochrome c-type biogenesis protein ccmF. It has an average length of 650 amino acids. As this gene has a housekeeping function, hence it is less susceptible to some forms of lateral gene transfer (22) .
The species L. interrogans is one of the dominant pathogen majorly found in the most infections related to Leptospirosis when compared to other pathogenic species like Leptospira borgpetersenii, Leptospira santarosai, Leptospira noguchii, Leptospira weilii, Leptospira kirschneri and Leptospira alexanderi. Cerqueira et al, 2009 demonstrated that the L. interrogans species is associated with severe human Leptospirosis, while the other strains like L. santarosai have shown their association with pigs and cattle. Hence, we first analyzed the various serovars related to species L. interrogans (23).
The potential of this assay must be balanced by a limitation: As ccmF gene is housekeeping gene, so it is present in non pathogenic Leptospira also. Hence DNA sequencing will be needed to discriminate between pathogenic and non pathogenic Leptospira.
Conclusion
The ccmF encoding gene had higher nucleotide divergence that allowed identification and also the potential for the discrimination between closely related Leptospiral serovars. The ccmF gene PCR may also likely to detect other L. interrogans serovars hence it may be valuable tool for early diagnosis of Leptospires directly from biological samples with clinical suspicion of leptospirosis. This new PCR could be useful in epidemiological studies to identify the source for disease outbreaks.
Acknowledgements
The authors gratefully acknowledge Dr.Yogesh Shouche of Microbial Culture Collection, National Centre for Cell Sciences, Pune, MS, India for performing sequencing of Leptospira serovars.
We thank the Director, Dr.P. Vijayachari of National Leptospirosis Reference Centre, Regional Medical Research Centre (ICMR), Port Blair, India for providing us the leptospiral reference serovars.
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature of this article has been reviewed and discussed.
Conflict of interests
The authors declare that they have no conflict of interests.
References:
1. Effler PV, Bogard AK, Domen HY, et al. Evaluation of eight rapid screening tests for acute leptospirosis in Hawaii. J Clin Microbiol.2002; 40: 1464-9.
2. Pappas G, Papadimitriou P, Siozopoulou V, et al. The globalization of leptospirosis: Worldwide incidence trends. Int J Infect Dis. 2008;12:351-7.
3. Sharma S, Vijayachari P, Sugunan AP, et al. Seroprevalence of leptospirosis among high-risk population of Andaman Islands, India. Am J Trop Med Hyg. 2006;74:278-83.
4. Manocha H, Ghoshal U, Singh SK, et al. Frequency of leptospirosis in patients of acute febrile illness in Uttar Pradesh. J Assoc Physicians India. 2004;52:623-5.
5.Karande S, Bhatt M, Kelkar A, et al. An observational study to detect leptospirosis in Mumbai, India, 2000. Arch Dis Child. 2003;88:1070-5.
6. Jena AB, Mohanty KC, Devadasan N. An outbreak of leptospirosis in Orissa, India: the importance of surveillance. Trop Med Int Health. 2004;9:1016-21.
7.Turner LH. Leptospirosis III. Maintenance, isolation and demonstration of leptospires.Trans R Soc Trop Med Hyg. 1970; 64: 623-646.
8.Terpstra WJ, Jabboury-Postema J, Korver H. Immunoperoxidase staining of leptospires in blood and urine. Zentralbl Bakteriol Mikrobiol Hyg. 1983; 254:534-539.
9.Terpstra WJ, Schoone GJ, Schegget J. Detection of leptospiral DNA by nucleic acid hybridization with 32P- and biotin-labelled probes .J Med Microbiol. 1986; 22:23-28.
10. Van Eys GJJM, Gravekamp C, Gerritsen MJ, et al. Detection of leptospires in urine by polymerase chain reaction. J Clin Microbiol. 1989;27:2258-2262.
11.Mulli KB, Faloona FA. Specific synthesis of DNA in vitro via a polymerase-catalyzed chain reaction. Methods Enzymol. 1987; 155: 355-350.
12. Mullis K, Faloona F, Seharf S, et al. Specific amplification of DNA in vitro: the polymerase chain reaction. Cold Spring Harb Symp Quant Biol. 1986; 51:263-273.
13. Larkin MA, Blackshields G, Brown NP, et al. Clustal W and Clustal X version 2.0. Bioinformatics.2007; 23:2947-2948.
14. X. Xia and Z. Xie DAMBE: Software Package for Data Analysis in Molecular Biology and Evolution. J Hered. 2001; 92 (4): 371-373.
15. Untergasser A, Cutcutache I, Koressaar T, et al. Primer3 - new capabilities and interfaces. Nucleic Acids Research.2012; 40(15):e115.
16. Koichiro Tamura, Daniel Peterson, Nicholas Peterson, et al.MEGA5: Molecular Evolutionary Genetics Analysis Using Maximum Likelihood, Evolutionary Distance, and Maximum Parsimony Methods Mol Biol Evol. 2011 Oct; 28(1).
17. Perolat P, Merien F, Ellis WA, et al. Characterization of Leptospira isolates from serovar hardjo by ribotyping, arbitrarily primed PCR, and mapped restriction site polymorphisms. J Clin Microbiol.1994; 32: 1949–1957.
18.Kawabata H, Dancel LA, Villanueva SYAM, et al. flaB-polymerase chain reaction (flaB-PCR) and its restriction fragment length polymorphism (RFLP) analysis are an efficient tool for detection and identification of Leptos.
19.Hermann JL, Belleger E, Perolat P, et al . Pulsed-field gel electrophoresis of NotI digests of leptospiral DNA: a new rapid method of serovar identification. J Clin Microbiol.1992; 30: 1696–1702.
20. Zuerner RL and Bolin CA. Differentiation of Leptospira interrogans isolates by IS1500 hybridization and PCR assays. J Clin Microbiol.1997; 35: 2612–1617.
21.Brown PD and Levett PN. Differentiation of Leptospira species and serovars by PCR-restriction endonuclease analysis, arbitrarily primed PCR and low-stringency PCR. J Med Microbiol.1997; 46: 173–181.
22.Carsten Sanders, Serdar Turkarslan, Dong-Woo Lee, et al. The Cytochrome c Maturation Components CcmF, CcmH, and CcmI Form a Membrane-integral Multisubunit Heme Ligation Complex J Biol Chem. 2008 Oct 31; 283(44): 29.
23.Gustavo M. Cerqueira, Alan J. A. McBride, Mathieu Picardeau, et al. Distribution of the leptospiral immunoglobulin-like (lig) genes in pathogenic Leptospira species and application of ligB to typing leptospiral isolates. J Med Microbiol. 2009 Sep;58(Pt 9):1173-81.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License