IJCRR - 10(15), August, 2018
Pages: 06-09
Date of Publication: 16-Aug-2018
Print Article
Download XML Download PDF
Leiomyosarcoma of Superior Vena Cava and Inferior Vena Cava - Two Rare Case Reports
Author: Puja Khanna, Shilajit Bhattacharya
Category: Healthcare
Abstract:Objective: This article attempts to describe two cases of vascular leiomyosarcoma, one arising from the superior vena cava in a 22 year old male patient, and the other arising from the inferior vena cava in a 53 year old female. The objective was to investigate and diagnose the two cases. Material and Methods: Imaging studies (CT scan) were done in both the cases subsequent to initial clinical examination. After surgical resection, the specimens of the tumors were sent to the Pathology Department for histopathological examination. The sections were stained using Haematoxylin and Eosin (H and E). Immunohistochemistry (IHC) was also done. Results: On gross examination, the first case showed a segment of a large vessel with a mass attached to the inner wall and protruding outside through the lumen. Tumor on cut section was solid, firm, homogenous grayish white with focal necrotic areas. In the second case, the vessel wall with an attached firm to hard lesion was received. On histological examination, both the cases were diagnosed to be malignant spindle cell tumor. Immunohistochemical staining revealed that the tumor cells were diffusely positive for SMA and Desmin and negative for S100 and CK. The two cases were reported as vascular leiomyosarcoma, one of the Superior vena cava and the other case of Inferior vena cava. Conclusion: Vascular leiomyosarcoma is a very rare tumor and the Inferior vena cava is the most common site (50%). The Superior vena cava (SVC) is exceptionally involved and only a dozen cases have been previously reported. An accurate imaging and histopathological diagnosis is essential as they can affect the prognosis and treatment approach. So such cases should be thoroughly examined and followed.
Keywords: Inferior vena cava Superior vena cava, Vascular leiomyosarcoma
Full Text:
INTRODUCTION
Vascular leiomyosarcoma is a very rare tumor and the inferior vena cava is the most common site (50%).1 The superior vena cava (SVC) is exceptionally involved and only a dozen cases have been previously reported.2 Leiomyosarcoma is considered a very locally aggressive tumor with rare distant dissemination and an unfavorable prognosis. An aggressive therapeutic approach, including chemoradiotherapy and large surgical resection, is usually considered the treatment of choice.3
CASE REPORT
The first case was a 22 year old male who came to the medical outpatient department with history of facial edema, engorgement of neck veins, hoarseness of voice and productive cough since 2 months.
CT scan of thorax revealed an intraluminal enhancing lesion in the distal right jugular vein and superior vena cava. It was suggestive of malignant etiology like SVC leiomyosarcoma. A differential diagnosis of intimal sarcoma was also considered.
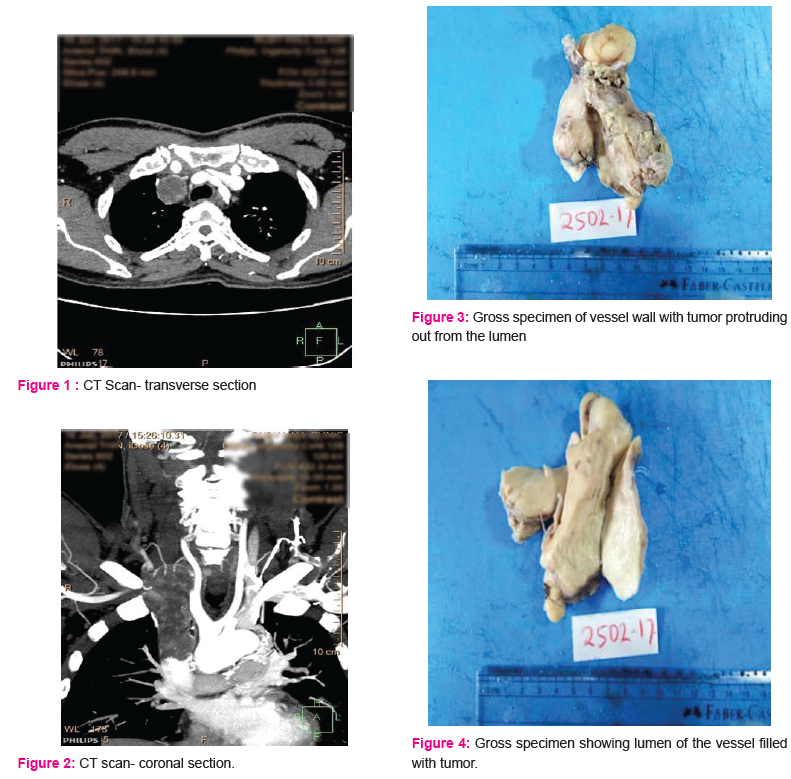
The second case was a 53 years old female who came with the complaints of pain abdomen and weight loss. The CT scan revealed a lesion in Inferior vena cava, 2 cm proximal to IVC bifurcation and 6 cm distal to right renal vein. [Figure 1and 2]
Both the patients underwent excision of the tumor with the vessel and reconstruction with a Dacron graft was done. The specimens were sent for histopathological examination.
GROSS EXAMINATION
The first case showed a segment of large vessel measuring 9.5x4.5x4 cm. A mass was seen attached to the inner wall of vessel and protruding outside through the lumen. Tumor on cut section was solid, firm, homogenous grayish white with focal necrotic areas.
In the second case, the vessel wall with an attached firm to hard lesion was received. It measured 4x3.8x3.2 cm. It also showed some bony hard areas. [Figure 3 and 4]
MICROSCOPIC EXAMINATION
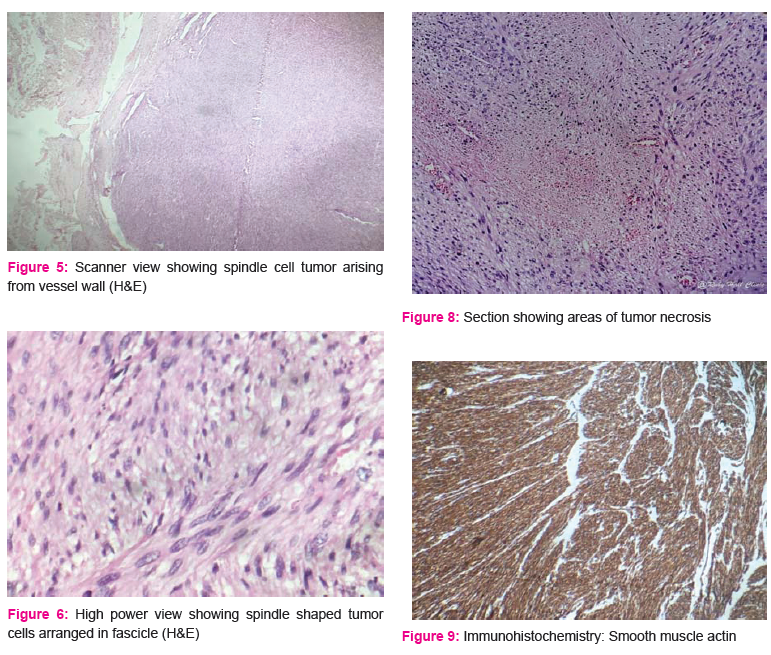
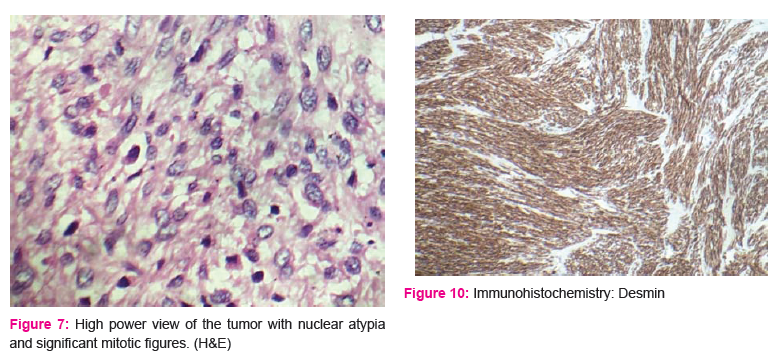
Microscopic features studied from multiple sections showed a cellular spindle cell tumor adherent to and present within the lumen of SVC. Tumor was composed of intersecting fascicles of spindle cells having pleomorphic, vesicular nuclei and moderate amount of eosinophilic cytoplasm. There were 25 mitosis per 10 high power field. Focal tumor necrosis was seen. Surgical margin was unremarkable.
The second case also showed similar histological appearance with large areas of metaplastic bone with adjoining areas showing osteoclastic giant cells. [Figures 5-8]
IMMUNOHISTOCHEMISTRY
Tumor cells were diffusely positive for Smooth muscle actin and Desmin and negative for S100 and Cytokeratin. [Figures 9 and 10]
DISCUSSION
Primary vascular leiomyosarcomas are very rare malignant tumors.4 The tumor originates from proliferation of smooth muscle cells of the media and may grow intravascularly or extravascularly or both.5 Growth pattern of the tumor varies from intraluminal to extraluminal or both. About 62% of cases have extraluminal, 33% have both, and only 5% of cases have intraluminal growth pattern.6
Distant dissemination is rarely described. It involves large veins almost five times more than arteries, and the most common site is inferior vena cava and its branches.3 The SVC localization is extremely rare.7
IVC leiomyosarcoma is most frequently seen in the sixth decade with a female predominance.8
The diagnosis is often challenging due to rarity of the tumor and nonspecific complaints. The optimal treatment for IVC leiomyosarcoma is still not known as few cases have been reported. Complete wide resection of the tumor with adjunctive radiotherapy or chemotherapy is the most preferred treatment.9
Nonmyogenic sarcomas, which are derived from the intima, are even more infrequent and are typically seen in the arterial system, particularly the pulmonary artery.10 Intimal sarcomas have also been reported in the Superior vena cava, Inferior vena cava and brachiocephalic vein.11,12
Typically leiomyosarcoma and angiosarcoma carry a better prognosis than undifferentiated intimal sarcoma with a mean 5-year survival of 33–53%.13
Immunohistochemical examination reveals positivity for Smooth muscle actin and Desmin in one half to nearly 100% of tumors.14
In the present cases, tumor cells displayed nuclear atypia and IHC stains were positive for Smooth muscle actin and Desmin.
CONCLUSION
Leiomyosarcoma of the Superior and Inferior Vena Cava are rare tumors and often malignant. An accurate imaging and histopathological diagnosis is essential as they can affect the prognosis and treatment approach. Immunohistochemistry helps in differentiating it from other entities. CT scan helped in localizing the position of the tumor and also its relationship to the surrounding structures. Long term survival depends on obtaining an early diagnosis and performing an extensive surgical resection with tumor free margins. So such cases should be thoroughly examined and followed.
Acknowledgement
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors / editors / publishers of all those articles, journals and books from where the literature for this article has been reviewed and discussed.
Conflict of interest: None
References:
-
Spaggiari, L., Regnard, J.F., Nottin, R. et al. Leiomyosarcoma of the superior vena cava. Ann Thorac Surg. 1996; 62: 274–276.
-
Picquet, J., Blin, V., Dussaussoy, C. et al. Surgical reconstruction of the superior vena cava system: indications and results. Surgery. 2009; 145: 93–99
-
Chaumont A, Pierret C, Kerangal X, Le Moulec S, Laborde F. Leiomyosarcoma of the Superior Vena Cava. The Annals of Thoracic Surgery. 2014;98(2):725-727.
-
Levett JM, Meffert WG, Strong WW, et al. Leiiomyosarcoma of the superior vena cava and azygous vein. Ann Thorac Surg 1995;60:1415-7.
-
Tovar-Martin E, Tovar-Pardo AE, Marini M, et al. Intraluminal leiomyosarcoma of superior vena cava: a cause of superior vena cava syndrome. J Cardiovasc Surg 1997;38:33-5.
-
Huang J, Liu Q, Lu JP, Wang F, Wang L, Jin AG. Primary intraluminal leiomyosarcoma of the inferior vena cava: Value of MRI with contrast-enhanced MR venography in diagnosis and treatment. Abdom Imaging 2011;36:337-41.
-
Benvenuti M, Lorusso R, Gelsomino S, et al. Resection of a primary leiomyosarcoma of the superior vena cava and right atium on a beating heart. Int J Cardiol 2011;15:151-3.
-
Hemant D, Krantikumar R, Amita J, Chawla A, Ranjeet N. Primary leiomyosarcoma of inferior vena cava, a rare entity: Imaging features. Australas Radiol 2001;45:448-51.
-
Kieffer E, Alaoui M, Piette JC, Cacoub P, Chiche L. Leiomyosarcoma of the inferior vena cava: Experience in 22 cases. Ann Surg 2006;244:289-95.
-
Fujita H., Kawata K., Sawada T., et al. Rhabdomyosarcoma in the inferior vena cava with secondary Budd-Chiari syndrome. Internal Medicine. 1993;32(1):67–71.
-
Sebenik M, Ricci A, Di Pasquale B, et al. Undifferentiated intimal sarcoma of large systemic blood vessels: report of 14 cases with immunohistochemical profile and review of the literature. The American Journal of Surgical Pathology. 2005;29(9):1184–1193.
-
Rytina E. R. C., Govil Y. K., Sabanathan K., Ball R. Y. Intimal sarcoma of the right brachiocephalic vein presenting as the superior vena caval syndrome. Journal of Clinical Pathology. 1996;49(4):347–349.
-
Burke A. P., Virmani R. Sarcomas of the great vessels. A clinicopathologic study. Cancer. 1993;71(5):1761–1773.
-
Weiss SW, Goldblum JR. Enzinger and Weiss’s soft tumor: 5th ed (Mosby Elsevier, Philadelphia, USA) 2008; 545-62.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License