IJCRR - 9(23), December, 2017
Pages: 01-03
Date of Publication: 15-Nov-2017
Print Article
Download XML Download PDF
Evaluation of Salivary Total Protein in Insulin Dependent Diabetes Mellitus (IDDM) Patients
Author: Syed Shahbaz, Chandrika Katti, Md. Munnawarulla Khan, Kapil Pawar
Category: Healthcare
Abstract:Aims: To evaluate salivary total protein in IDDM patients and to compare with healthy non-diabetic control group.
Methods and Material: The study consisted of 50 IDDM patients and 50 age matched healthy controls. All the subjects were
subjected to the salivary total protein estimations. Salivary total protein estimations were done by Biuret method, end point. All the estimations were performed using an auto analyser. Mean, standard deviation and students 't' test were calculated. All these statistical analysis were performed by using SPSS 20 versionsoftware.
Results: The results showed elevated levels of salivarytotal protein in IDDM group compared to healthy controls.
Conclusion: There are definite changes in salivary composition with increased levels of salivary total protein in IDDM patients
compared to healthy controls.
Keywords: IDDM, Saliva, Total protein
DOI: 10.7324/IJCRR.2017.9231
Full Text:
Introduction
Diabetes mellitus (DM) is an endocrine disease characterized by a shortfall in the production of insulin with consequent alteration of the process of assimilation, metabolism and balance of blood glucose concentration.1 Although all forms of DM are characterized by hyperglycemia, the pathogenic mechanisms by which hyperglycemia arises differ widely. It is thus classified, as type IDDM (Insulin dependent diabetes mellitus) and NIDDM (Non-Insulin dependent diabetes mellitus).2IDDM is a multifactoral autoimmune disease for which susceptibility is determined by environmental and genetic factors. 3, 4It was estimated in 2010, that 76,000 children aged less than 15 years develop type I DM worldwide. The incidence rate of type I DM in India is 4.2/100,000 population per year. 1
Saliva has long been viewed as unique yet complex body fluids, like plasma or serum. Saliva is easy to collect by non-invasive methods and preservation is inexpensive. The diagnostic value of saliva lies in its components, flow and structure of glands. 3, 5Salivary total protein is a vital component of saliva, predominantly comprising proline-rich proteins.6, 7 Noticeably there is spurge of interest in non-invasive diagnostic testing. It has become apparent that saliva has many diagnostic uses especially in large scale screening.8With this consideration present study was done to evaluate salivary total protein in IDDM and compare with healthy non-diabetic controls.
Method and Materials:
The study was conducted on 50 patients with IDDM and 50 age-matched healthy non-diabetic individuals. The IDDM and control group consisted of 32 males and 18 females respectively. The patients included in the study were taken from Diabetic Care Centres. Patients with IDDM and individuals who volunteered to participate in the study were included and patients having systemic diseases other than diabetes mellitus were excluded from the study. The informed consent was obtained from both the groups, and ethical clearance was obtained from institutional ethical committee.
All the subjects included in the IDDM and control group were advised not to eat anything and until the samples were collected. The saliva samples from both study and control groups were collected at 8 am. The unstimulated whole saliva was collected by spitting method. The collected saliva was subjected to total protein estimation.The salivary total protein wasperformed by Biuret method, the peptide bonds of protein react with copper II ions in alkaline solution to form blue-violet complex, (biuret reaction). Each copper ion complexing with 5 or 6 peptide bonds, the colour formed is proportional to the protein concentration and is measured at 546nm (520-560nm).9, 10Allthe estimations were performed using reagent kits of Transasia Bio-Medical Ltd. and on an autoanalyser(ERBA, Mannheim, GERMANY).
Results
The study consisted of 50 diagnosed IDDM patients and 50 age-matched healthy controls. The IDDM and control group consisted of 32 males and 18 females, the age ranged from 4 to 16 years. Fasting saliva samples were collected with their consent and were evaluated for salivary total protein by using autoanalyser. The values obtained for salivary total protein were statistically analysed for mean and standard deviation (SD). Students ‘t’ test was employed to compare the values of IDDM and control group. All these statistical analysis were performed by using 20 Version SPSS software.
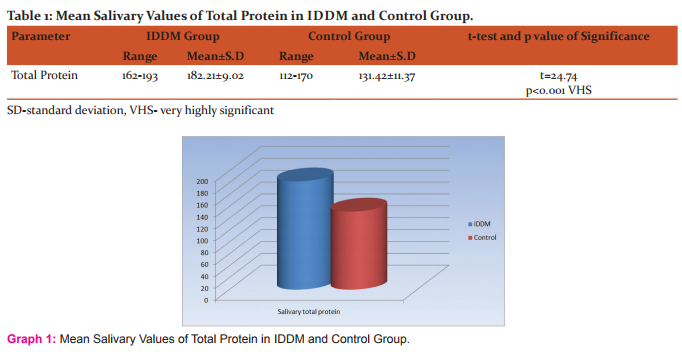
The mean salivary total protein level in control group was 131.42 mg/dl and SD 11.37 and the protein levels were ranged from 113 to 170 mg/dl.The mean salivary total protein level in IDDM group was 182.21 mg/dl and SD 9.02 and the levels were ranged from 162 to 192 mg/dl.The ‘t’ value for the comparison of salivary total protein in IDDM and control group was t= 24.74 and p<0.001 which denotes statistically VHS.[Table 1 and Graph 1]
Discussion
It is beautifully said by Mandel that “saliva lacks the drama of blood, sincerity of sweat and emotional appearance of tears”, but still the fact is that, it is the vital element that sustains life in the oral cavity. The constituents of saliva not only maintains the oral health but also plays a vital role in diagnosis of various oral diseases like oral cancer, candidiasis, periodontal disease, etc. as well as it detects numerous systemic diseases like HIV, diabetes, heart diseases, etc.11Saliva indeed is a mirror of our blood as these bio-fluids and their molecular components share many similarities. Saliva as a diagnostic fluid offers distinctive advantages over serum because it can be collected non-invasively. Furthermore, it may provide a cost effective approach for the large scale diagnostic screening.6Amongst various systemic diseases, the most routinely encountered disease is the diabetes mellitus. Hyperglycaemia in diabetes results from defects in insulin secretion, insulin action or both. Diabetes is broadly classified into IDDM and NIDDM. IDDM is a severe disease that raises blood glucose concentration because of hyperglycaemia and insulinopenia.12
The salivary total protein is a vital component of saliva, predominantly comprising proline rich proteins. The levels of proteins depend on the salivary flow rate, as the flow rate decreases the protein levels increases. Proteins found in saliva such as lactoferin, lysozyme, peroxidase, defensins and histatins can destroy or inhibit the growth of micro-organisms in the oral cavity. They can also maintain an ecological balance among the diverse bacteria that affect oral and general health.13
Our results revealed that levels of salivary total protein were higher in IDDM group as compared to control group [Table 1]. These results are in accordance with the previous studies done by Lopez et al14, Gheena S. et al1, Ezel Yavuzylmaz et al15, Antonio D. et al16, Anita N et al17, Ben Aryeh H et al18 and Rosamund Harrison et al19. However few studies done by Maria A Belazi et al20, S. Tweetman et al21 and J. Tenovo et al22 showed no significant difference between the diabetic patients and controls. This contradiction can be explained by the fact that the studies might have incorporated different methodology and metabolic control status of the patients.The elevated levels could be explained with abnormal binding of serum proteins to salivary gland basement membranes may be a reflection of increased permeability; this basement membrane permeability is often associated with diabetes which leads to increased passage of proteins, IgG, albumin, and polyvalent immunoglobulins from exocrine glands into their secretions.22 The salivary flow rate in diabetes is also diminished which is related to salivary viscosity and foam. Viscosity otherwise called “spinbarkeit” and foam are reflected by the higher levels of proteins.14
Conclusion:
There are elevated levels of salivary total protein in IDDM patients compared to the healthy controls.These findings may be attributed to the disease process; hence a more extensive research with more sample size will put a light on its effect with disease progression.
Acknowledgement
Authors acknowledge the immense help received from the scholars whose articles are cited and included in references of this manuscript. The authors are also grateful to authors/ editors/ publishers of all those articles, journal and books from where this article has been reviewed and discussed.
Conflict of interest: None
References:
- Gheena S., Chandrashekhar T, Pratibha Ramani. Salivary characteristics of diabetic children. Braz J Oral Sci 2011;10:93-7.
- Ana Carolina U. Vasconcelos, Maria Sueli M. Soares, Paulo C. Almeida, Teresa C. Soares.Comparative study of the concentration of salivary and blood glucose in type 2 diabetic patients. Journal of oral science2010;52:293-8.
- Roland Tisch and Hugh Macdevitt. Insulin dependent diabetes mellitus. Cell 1996;85:291-7.
- Hedge A, Shenoy R, Prajwal D’Mello, Smitha A, Tintu A, Manjrekar P. Alternative markers of glycemic status in diabetes mellitus. Biomedical research 2010;21:252-6.
- Maria-Sueli-Marques Soares, Mario-Marcio-Vasconcelos Batista-Filho, Marcele-Jardim Pimentel, Isabela-Albuquerque Passos, Eduardo Chimenos-Kustner. Determination of salivary glucose in healthy adults. Med Oral Patol Oral Cir Buccal2009;14:e510-3.
- Krishna BA, Ashalatha G, Baghirath VP, Rajani Kanth AV, Malathi N. Saliva as a diagnostic biofluid-review. J OrofacSci 2010; 2:66-70.
- Arati S. Panchbhai, Shirish S. Degwekar, Rahul R. Bhowle. Estimation of salivary glucose, salivary amylase, salivary total protein and salivary flowrate in diabetics in India. Journal of oral science2010;52:359-68.
- Amer S, Yousuf M, Siddiqui PQR, Alam J. Salivary glucose concentrations in patients with diabetes mellitus- a minimally invasive technique for monitoring blood glucose levels. Pakistan journal of pharmaceutical sciences 2001;14:33-7.
- Thomas L. Clinical laboratory diagnostics. 1st ed. Frankfurt: TH books Veriagsgessell chaft; 1998;131-7.
- Tietz. N. W. Text book of clinical chemistry, W.B. Saunders, 1986;231-46.
- Mandel ID. The diagnostic uses of saliva. J Oral Pathol Med 1990;19:119-25
- American Diabetes Association. Diagnosis and classification of Diabetes Mellitus. Diabetes Care 2010;33:S62-9.
- Herenia P. Lawrence. Salivary markers of systemic disease: noninvasive diagnosis of disease and monitoring general health. J Can Dent Assoc 2002;68:170-4.
- Lopez ME, Colloca ME, Paez RG, Schallmach JN, Koss MA, Chervonagura A. Salivary characteristics of diabetic children. Braz Dent J 2003; 14:26-31.
- Yavuzyilmaz E, Yumak O, Akdoqanli T, Yamalik N, Ozer N, Ersoy F, Yeniay I. The alterations of whole saliva constituents in patients with diabetes mellitus. Australian Dental Journal 1996;41:193-7.
- Antonio D. Mata, Duarte Marques, Sara Rocha, Helena Francisco, Carolina Santos, Maria F. Mesquita, et al. Effects of diabetes mellitus on salivary secretion and its compostion in the human. Molecular and Cellular Biochemistry 2004;1-6.
- Amita Nawalkar and Anilkumar Bhoweer. Alterations in whole saliva constituents in patients with diabetes mellitus and periodontal disease. Journal of Indian Academy of Oral Medicine and Radiology 2011;23:498-501.
- Ben Aryeh H, Cohen M., Kanter Y., Szargel R., Laufer DZ. Salivary composition in diabetic patients. J Diabet Complications 1988;2:96-9.
- Rosamund Harrison and William H. Bowen. Flow rate and organic constituents of whole saliva in insulin-dependent diabetic children and adolescents. Pediatric Dentistry 1987;4:287-91.
- Maria A. Belazi, Galli-Tsinpoulou A, Drakoulakos D, Fleva A, Panayaiotis H. Papanayiotou. Salivary alterations in insulin-dependent diabetes mellitus. International Journal Of Pediatric Dentistry 1998;8:29-33.
- Svante Tweetman, Tommy Nederfors, Birgitta Stahl Stefen Aronson. Two year longitudinal observations of salivary status and dental caries in children with insulin-dependent diabetes mellitus. Pediatr Dent 1992;14:184-88.
- J. Tenovuo, O. Lehtonen, J. Vkari, H. Larjava, P. Vilja and P. Tuohimaa. Immunoglobulins and innate antimicrobial factors in whole saliva of patients with insulin-dependent diabetes mellitus. J Dent Res 1986;65:62-66.
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License