IJCRR - 5(2), January, 2013
Pages: 38-41
Date of Publication: 26-Jan-2013
Print Article
Download XML Download PDF
EVALUATION OF INTERLEUKIN-1 IN PATIENTS WITH ORAL SQUAMOUS CELL CARCINOMA AS A MARKER OF PERIODONTITIS
Author: Uma Sudhakar, Akila Sivaranjani, Manoj Chand Dayan
Category: General Sciences
Abstract:New insight regarding the etiology as well as the strategies for prevention of oral cancer is needed. This study was carried out in the Department of Periodontics Thai moogambigai dental college, Chennai and Department of Oncology Apollo Research institute Chennai. Study reveals that there was a significant increase in the level of IL-1 in patients with carcinoma and chronic periodontits.
Full Text:
INTRODUCTION
The given statistics of oral cancer incidence and survival have remained essentially unchanged over the past three decades despite the accessibility of the oral cavity to direct examination, promotion effects against known risk factors of oral cancer, and advances in the treatment and diagnosis arguing forcibly for new approaches [1] . New insight regarding the etiology as well as the strategies for prevention is needed. Considerable evidence indicates that chronic infections and persistent inflammation are associated with increased cancer risk2 . Periodontitis is a chronic oral infections thought to be caused by gram negative anaerobic bacteria in the dental biofilm 3 .Recent evidence also suggests a significant role for viruses in the initiation and progression of periodontitis .It leads to irreversible destruction of tissue supporting teeth, clinically detectable as periodontal pockets and alveolar bone loss. Periodontitis results in a continuous release of bacterial and inflammatory markers into the saliva and to a lower degree into the blood 4 .The mediators travel to distant sites and adversely affect systemic health. Periodontitis, characterized by epithelial proliferation and migration, results in chronic release of inflammatory cytokines, chemokines, prostaglandins, growth factors and enzymes all of which are closely associated with carcinogenesis5 . Cytokines produced locally have an influence on the development of a particular immune response 6 . Major advances have been made in the field of cytokines regulation of t cell function and so called Type -1 and Type-2 cytokines may play a predominant roles in determining the outcome of the infection7 .IL-1, is a key mediator of chronic inflammatory disease with the potential to initiate tissue destruction and bone loss in periodontal disease 8 . Studies have shown that patients with oral cancer have elevated levels of inflammatory cytokines in their saliva.(Brailo 2011) IL-1 is also used as a marker for early diagnosis of oral cancer using salivary diagnostics methods (Y.Shing 2011).Number of studies suggests a synergy between chronic periodontitis and squamous cell carcinoma independent of smoking status age, race and ethinicity which generates a hypothesis about a possible relationship between periodontal disease and oral neoplasms 9 . In the present study the level of IL-1 in patients with periodontitis and oral cancer was estimated. The aim of this study was to assess the level of IL-1 in patients with oral cancer as a marker of periodontitis using saliva as a diagnostic tool.
MATERIALS AND METHODS
Ethical Considerations: Approval from the ethical committee has been obtained and informed concern was taken from the patient. . Patient care throughout the study was conducted in accordance with the principles of the Helsinki Declaration of 1975, as revised in 2000.
Patients: The study population consisted of patients seen in the Department of Periodontics Thai moogambigai dental college, Chennai and Department of Oncology Apollo Research institute Chennai. The subjects were grouped under four major categories like chronic periodontits, chronic periodontitis with oral squamous cell carcinoma and squamous cell carcinoma alone and the control. Each group consisted of 10 subjects each. Unstimulated whole saliva was collected from each subject. Subjects were asked to rinse their mouth with normal water and then were asked to expectorate whole saliva in the sterile tube. IL-1 in saliva was measured by enzyme linked immunosorbent assay [Human Dental ELISA kit KOREA]. This IL-1β enzyme linked immunosorbent assay (ELISA) applies a technique called quantitative sandwich immunoassay. The microtiter plate provided in this kit has been pre-coated with a monoclonal antibody specific to IL-1β. Standards or samples are then added to the appropriate microtiter plate wells and incubated. After washing to remove unbound IL-1β and other components of the sample, biotin-conjugated polyclonal antibody specific to IL-1β is added and incubated. Laboratory technicians determined the concentrations of salivary biomarkers IL-1.The resulting yellow colour was then read on an ELISA reader and a standard curve was generated to calculate the results.
STATISTICAL ANALYSIS
Chi-square test was used to assess the P-value.
DISCUSSION
Periodontitis is a chronic oral infection caused by inflammatory reactions to gram negative anaerobic bacteria 10 which results in continuous release of toxins and inflammatory markers in the blood stream and saliva. In the present study, IL-1 was significantly more in patients with cancer and periodontitis than patients with only cancer. When compared with the normal subjects IL-1 value was significantly more in subjects with carcinoma (0.016).This is to our knowledge is one of the first study to estimate the level of IL-1 in both oral cancer and chronic periodontitis. Recent evidence suggests a significant role for viruses in the initiation and progression of periodontitis. More interestingly ,studies suggests that periodontal pockets acts as a reservoir for Human papilloma Virus (HPV), 8 cytomegalovirus and Epstein bar virus which are the suspected agents associated with oral cancer. The question of how infection and inflammation can influence carcinogenesis has interested scientists for the past one and half centuries but only now have come up with the certain principles and currently the complexities of this association are emerging. Chronic periodontitis can play a direct or indirect role in carcinogenesis11: 1. Direct effect of micro organism: Micro organisms and their products such as endotoxins, metabolic by products and enzymes [collagenase proteases etc] are toxic to surrounding cells and may directly induce mutations in tumor suppressor genes or alter the signaling path ways that affect the cell proliferation. 2. Indirect effect through inflammation-chronic infection may stimulate the formation of epithelialized tumors through an indirect mechanisms involving activation of surrounding inflammatory cells. Micro organisms activate, [A] The host cells like macrophages, monocytes, lymphocytes to generate reactive O2 species (H2O2 +OXY RADICALS) and matrix metalloproteases which can induce DNA damage in epithelial cells [B] Produce cytokines, chemokines, growth factors and other signals that provide an environment for cell survival, proliferation, migration, angiogenesis and inhibition of apoptosis. This environment may help epithelial cells to accumulate mutations and drive these mutant epithelial cells to proliferate, migrate and give them a growth advantage.
CONCLUSION
In the present study there was a significant increase in the level of IL-1 in patients with carcinoma and chronic periodontits. This study present us to our knowledge the first evidence of association between level of salivary biomarker interleukin 1 in subjects with periodontitis and in oral squamous cell carcinoma. The present study had a smaller sample size, the association needs to be compared by larger studies with a more comprehensive assessment. A specific association between chronic periodontitis and oral cancer is possible .There is a growing need to and explore this possibility, which will have a potential impact on understanding the etiology of oral cancer as well as on its prevention and control.
References:
1. Canto MT, Devesa SS.Oral cavity and pharynx cancer incidence rates in United States 1975-1998.Oral oncology 2002; 38: 610-617.
2. Karin M, Lawrence T, Nizet V, Innate immunity gone away:linking microbial infection to chronic inflammation and cancer.Cell.2006;124:823-835.
3. Mine Tezal, Mayreen A, Sullivan, Andrew Hyland et al, Chronic periodontitis and the head and neck squamous cell carcinoma, Cancer epidemiology biomarkers prevention 2009;18(9) September 2009.
4. Champagne CME,Buchanan W,Reddy MS,Pressier JS,Beck JD,Offenbaxher S.Potential for gingival crevice fluid measures as predictors of risk of periodontal disease.Periodontal 2000,2003;31:167-80.
5. Loesche WJ, Grossman NS,Periodontal diseases as a specific,albeit chronic infection :diagnosis and treatment .Clinical microbiology Rev 2001;14:727-752.
6. E.Gemmell and GJ.Seymour, cytokine profiles of extracted from humans with periodontal diseases; J Dental Research 77(1):16-26,January 1998.
7. Cytokine profiles of cells extracted from humans with periodontal diseases,E.Gemmel and G.J.Seymour,J Dent Res 77(1):16-26.
8. Horimia M,Willberg J,Ruokonen H,Syrjanen S,Marginal periodontium as a potential reservoir of human papilloma virus in oral mucosa.J Periodontal.2005;76(3):358-363.
9. SaygunI,Kubar A,Ozdemir A,et al Periodontitis lesions are source of cytomegalovirus and Epstein Barr Virus .J.Periodontal Res.2005;40:187-191.
10. Tezal M, Grossi SG, Genco RJ, Is Periodontitis associated with oral neoplasms?J Periodontology 2005:76:406- 10.
11. Chronic periodontitis and risk of tongue cancer Mine Tezal, DDS, Phd ;MaureenA.Sullaivan, DDS; Mary E.et al; Arch Otolaryngol Head Neck Surg. 2007; 133: 450-454.
STATISTICAL ANALYSIS:
Chi-square test was used to assess the P-value.
RESULTS
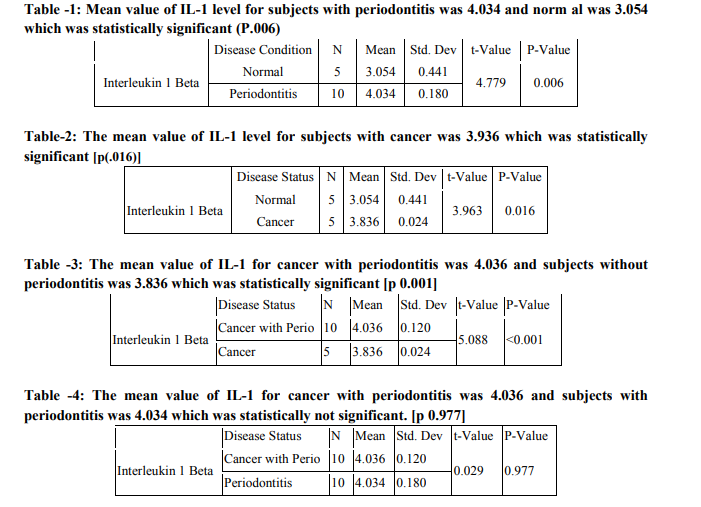
|






 This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License